Introduction
The growing prevalence of class III obesity (BMI ≥ 40 kg/m²) is transforming perioperative care worldwide. Patients with obesity present unique respiratory and cardiovascular challenges, particularly during general anesthesia and mechanical ventilation. A 2026 narrative review by Boesing et al. (BJA) highlights the critical role of positive end-expiratory pressure (PEEP) in optimizing outcomes for this high-risk population.
Understanding obesity-related respiratory physiology
Key physiological changes
Obesity significantly alters pulmonary mechanics, increasing the risk of complications during surgery.
- reduced functional residual capacity (FRC)
- increased pleural pressure
- decreased lung compliance
- increased airway resistance
- ventilation–perfusion mismatch
According to the review by Boesing et al., FRC decreases by 5–15% for every 5 kg/m² increase in BMI, leading to early airway closure and alveolar collapse.
Why PEEP matters in obese surgical patients
Role of PEEP in lung protection
PEEP is a cornerstone of lung-protective ventilation. It works by:
- preventing alveolar collapse (atelectasis)
- increasing end-expiratory lung volume (EELV)
- improving oxygenation
- enhancing ventilation–perfusion matching
When applied correctly, PEEP counteracts elevated pleural pressures seen in obesity.
Risks of improper PEEP
However, inappropriate PEEP levels can lead to:
- alveolar overdistension
- increased lung stress and strain
- reduced venous return
- cardiovascular instability
Atelectasis: a major perioperative risk
Why obese patients are vulnerable
Up to 90% of patients under general anesthesia develop atelectasis, with higher rates in obesity.
Contributing factors include:
- increased abdominal pressure pushing the diaphragm upward
- reduced lung volumes
- impaired surfactant function
- high pleural pressures
Clinical consequences
Personalized PEEP: the emerging standard
Why fixed PEEP is insufficient
Traditional fixed PEEP strategies (e.g., 4–12 cm H₂O) often fail to address individual variability.
Studies show:
- many obese patients require PEEP > 15 cm H₂O
- some cases (BMI > 50) may require 20–25 cm H₂O
Benefits of personalized PEEP
- improved respiratory compliance
- reduced driving pressure
- better oxygenation
- decreased atelectasis
Step-by-step PEEP optimization strategy
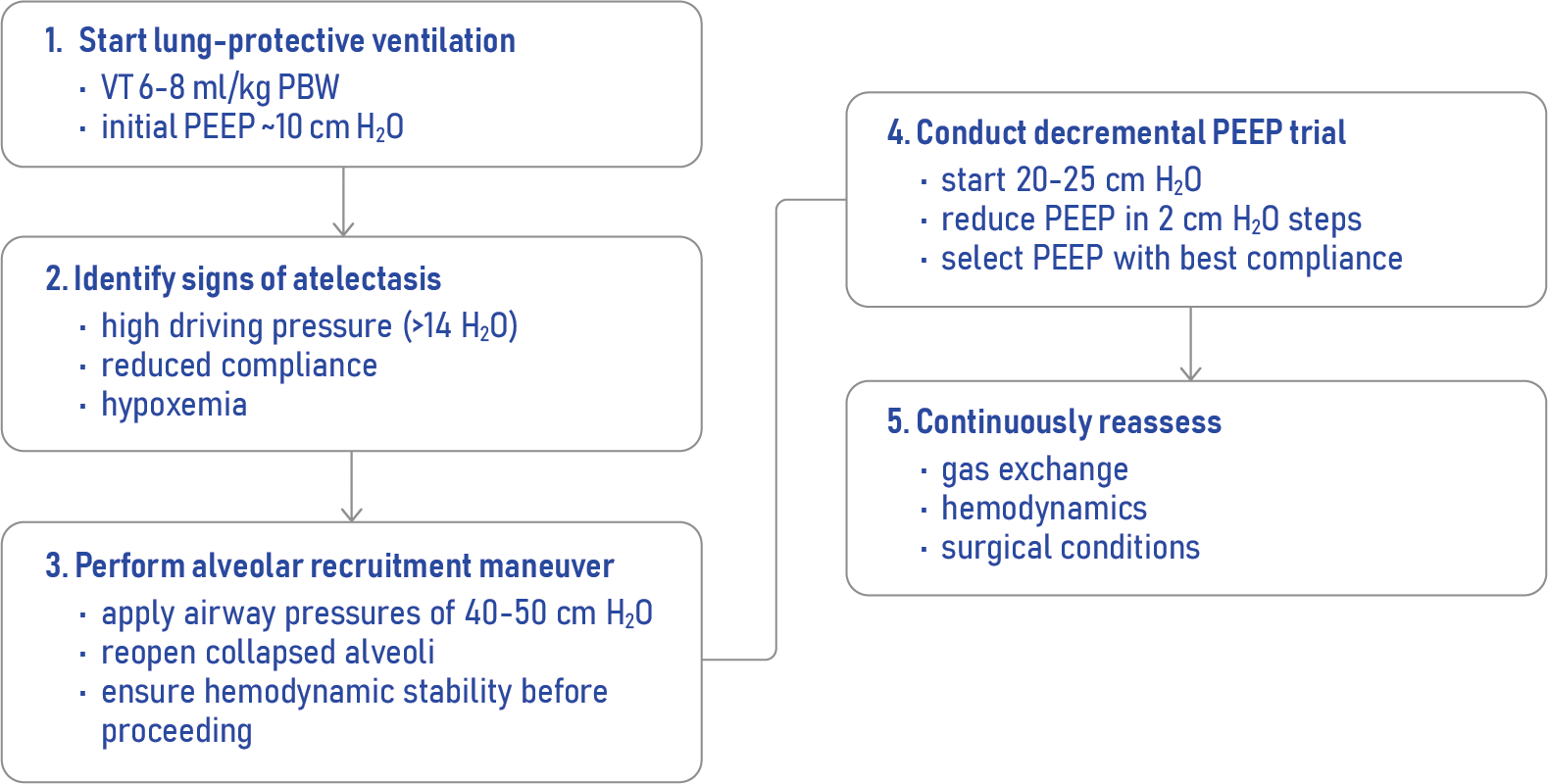
Clinical indicators for PEEP adjustment
- driving pressure > 14 cm H₂O
- decreasing lung compliance
- worsening oxygenation
- increasing FiO₂ requirements
Cardiovascular effects of PEEP
Positive effects
- reduced left ventricular afterload
- improved oxygenation
- decreased pulmonary vascular resistance (with proper use)
Potential adverse effects
- reduced venous return
- hypotension
- bradycardia (especially during recruitment maneuvers)
Interestingly, in obese patients:
- elevated pleural pressures may protect against hemodynamic compromise
- cardiac output often remains stable even at higher PEEP levels
Interplay between lung and heart
PEEP influences:
- cardiac preload
- right ventricular afterload
- pulmonary circulation
Key takeaway:
- balance is essential. Optimize lung function without impairing circulation
Postoperative challenges
Even with optimal intraoperative PEEP:
- benefits may disappear within hours after extubation
- atelectasis can recur quickly
This highlights the need for:
- postoperative respiratory support
- continued lung recruitment strategies
Practical recommendations
Core clinical principles
- anticipate obesity-related physiology
- identify atelectasis risk early
- use recruitment maneuvers cautiously
- personalize PEEP settings
- monitor continuously for complications
Conclusion
PEEP optimization in obese patients undergoing general anesthesia is complex but essential. A personalized, physiology-driven approach offers the best balance between improving respiratory function and maintaining cardiovascular stability.
While current evidence supports individualized strategies, further large-scale studies are needed to confirm their impact on patient-centered outcomes.
Reference: Boesing C et al. Positive end-expiratory pressure optimisation during general anaesthesia in patients with obesity: a narrative review of respiratory and cardiovascular outcomes. Br J Anaesth. 2026;136:970-982.
For real-time clinical educational support, dosing information, and case simulations, explore the NYSORA Anesthesia Assistant App.