Learning objectives
- Definition of euglycemic diabetic ketoacidosis (EDKA)
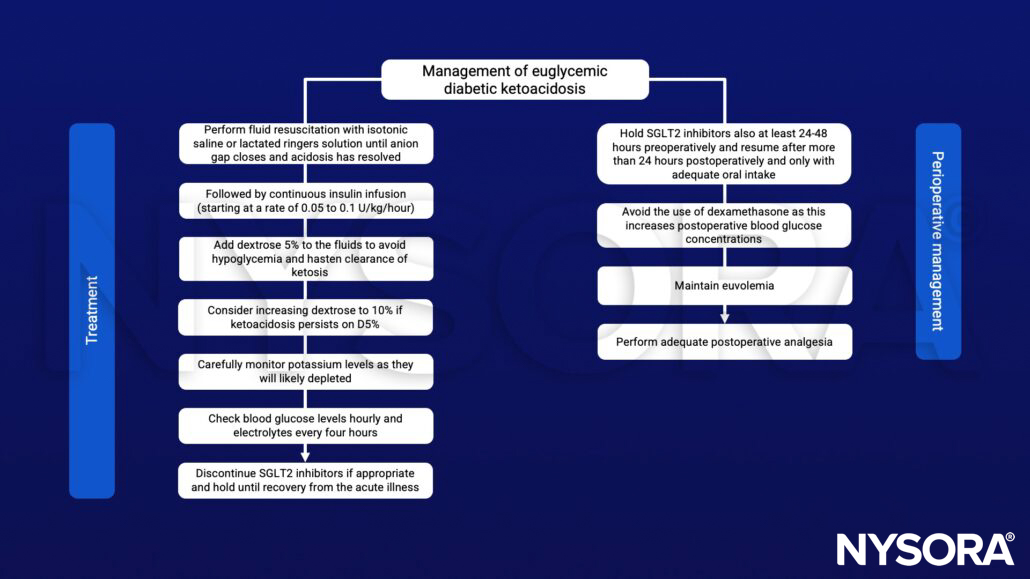
- Management of EDKA
Definition and mechanisms
- Diabetic ketoacidosis (DKA) is defined as metabolic acidosis with hyperglycemia and increased ketone bodies in the blood and urine, with hyperglycemia the hallmark for the diagnosis of DKA
- However, in a subset of patients, are the serum glucose levels within the normal limits, this is defined as euglycemic diabetic ketoacidosis (EDKA)
- This rare condition is a diagnostic challenge as euglycemia masquerades the underlying diabetic ketoacidosis
- Occurs in both type 1 and type 2 diabetes mellitus and can be life-threatening
- EDKA is secondary to a carbohydrate deficit resulting in generalized decreased serum insulin and excess hormones such as glucagon, epinephrine, and cortisol
- The increased glucagon/insulin ratio leads to increased lipolysis, increased free fatty acids, and ketoacidosis
- The resulting anion gap metabolic acidosis triggers respiratory compensation and sensation of dyspnea, as well as nausea, anorexia, and vomiting
- The resulting volume depletion further exacerbates elevations in glucagon, cortisol, and epinephrine, worsening lipolysis and ketogenesis
- Additionally, decreased hepatic gluconeogenesis or increased glucosuria contribute to EDKA
Signs and symptoms
- Metabolic acidosis (pH < 7.3, serum bicarbonate < 18 mEq/L)
- Ketonomia or kenonuria
- Normal blood glucose levels < 250 mg/dL
- Malaise
- Dyspnea
- Nausea
- Vomiting
- Confusion
- Excessive thirst/urination
- Kussmaul respiration (deep, rapid)
Etiology
- Starvation resulting in ketosis while maintaining normoglycemia
- Anorexia
- Gastroparesis
- Fasting
- Use of a ketogenic diet
- Alcohol use
- Persistent vomiting
- Pregnancy
- Pancreatitis
- Glycogen storage disorders
- Surgery
- Infection
- Cocaine toxicity
- Cirrhosis
- Insulin pump use
- Dehydration
- Sodium-glucose cotransporter 2 (SGLT2) inhibitors:
- SGLT2 inhibition in the proximal renal tubules promotes glycosuria
- Resulting in diminished insulin production and elevated plasma glucagon concentrations
Complications
- Dehydration
- Vomiting
- Hypoglycemia
- Hypovolemic shock
- Respiratory failure
- Cerebral edema
- Coma
- Seizures
- Infection
- Thrombosis
- Myocardial infarction
Diagnosis
- Blood or urine ketone testing
- Laboratory evaluation:
- Electrolytes
- Glucose
- Calcium
- Magnesium
- Creatinine
- BUN
- Serum and urine ketones
- Beta-hydroxybutyric acid
- Arterial or venous blood gas analysis
- Lactic acid
- Chest X-ray
- ECG
- Serum osmolality
- Alcohol
Management
Suggested reading
- Nasa P, Chaudhary S, Shrivastava PK, Singh A. Euglycemic diabetic ketoacidosis: A missed diagnosis. World J Diabetes. 2021;12(5):514-523.
- Thiruvenkatarajan, V., Meyer, E.J., Nanjappa, N., Van Wijk, R.M., Jesudason, D., 2019. Perioperative diabetic ketoacidosis associated with sodium-glucose co-transporter-2 inhibitors: a systematic review. British Journal of Anaesthesia 123, 27–36.
- Rawla, P., Vellipuram, A.R., Bandaru, S.S., Pradeep Raj, J., 2017. Euglycemic diabetic ketoacidosis: a diagnostic and therapeutic dilemma. Endocrinology, Diabetes & Metabolism Case Reports 2017.
- Modi A, Agrawal A, Morgan F. Euglycemic Diabetic Ketoacidosis: A Review. Curr Diabetes Rev. 2017;13(3):315-321.
Clinical updates
Ruste et al. (BJA, 2024) report that euglycemic ketoacidosis can occur perioperatively in patients without diabetes treated with SGLT2 inhibitors, particularly when combined with prolonged fasting and surgical stress. Their case series shows that normoglycemia and even normal arterial pH may mask significant ketonaemia due to compensatory hyperventilation, delaying diagnosis.
Tinsley et al. (BJA, 2025) highlight that SGLT-2 inhibitors are a major perioperative trigger of euglycemic diabetic ketoacidosis, often presenting with normal blood glucose during fasting or acute illness. The review recommends withholding SGLT-2 inhibitors at least 48 hours before surgery, routine ketone monitoring, and delaying drug reinitiation until normal oral intake and ketone clearance are confirmed.