Learning objectives
- Describe bronchopulmonary dysplasia
- Understand the pathophysiology of bronchopulmonary dysplasia
- Recognize the risk factors for developing bronchopulmonary dysplasia
- Anesthetic management of a pediatric patient with bronchopulmonary dysplasia
Definition and mechanisms
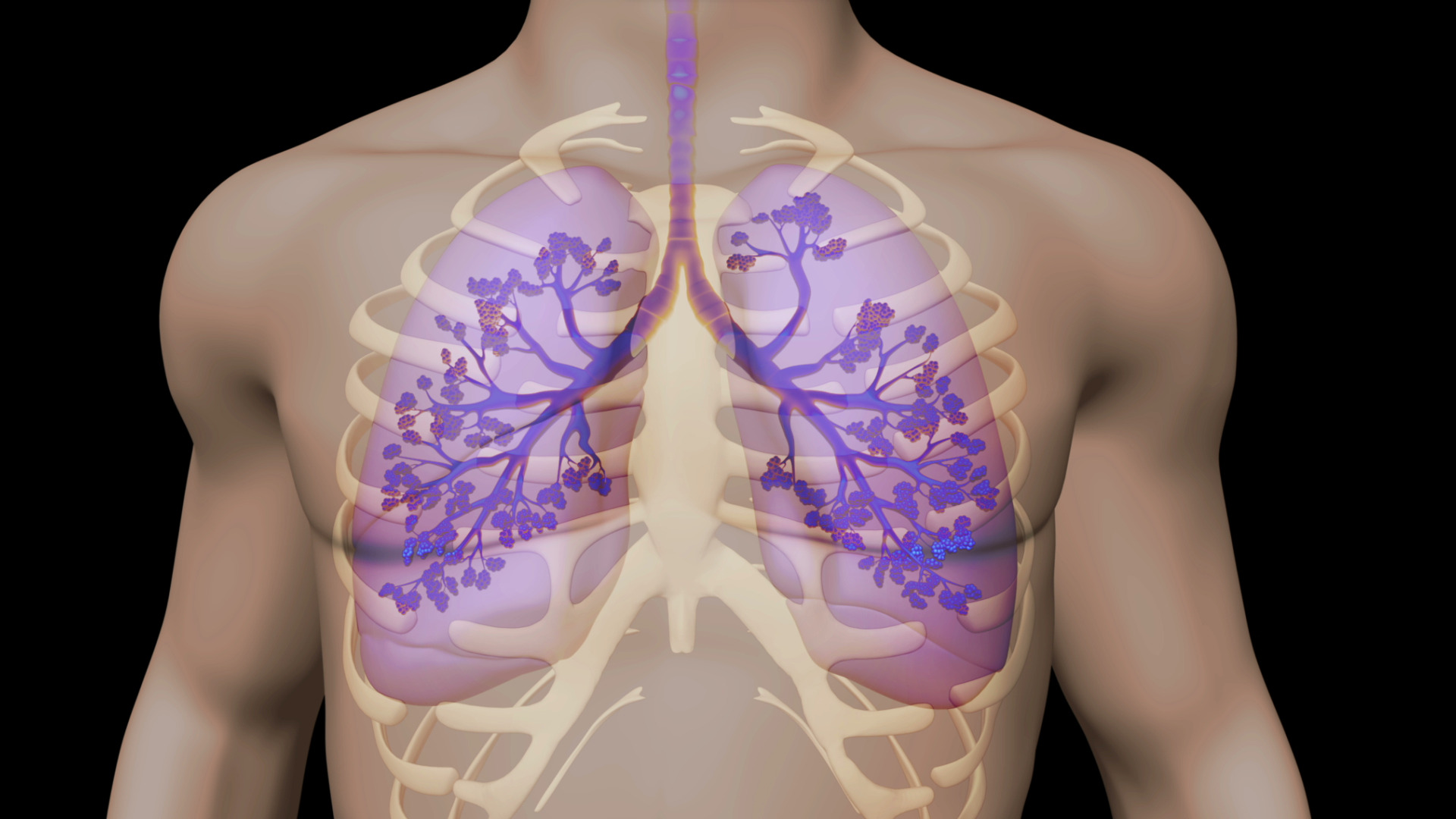
- Bronchopulmonary dysplasia (BPD) is a chronic lung disease in which premature infants require long-term oxygen because the alveoli that are present, are not mature enough to function properly
- Babies are not born with BPD, the condition results from damage to the lungs, usually caused by mechanical ventilation and long-term use of oxygen
- BPD is more common in infants with a low birth weight and those who receive prolonged mechanical ventilation to treat respiratory distress syndrome
- BPD develops most commonly in the first 4 weeks after birth
| Criteria for BPD diagnosis | |
|---|---|
| Infants requiring supplemental oxygen at 28 days are diagnosed, via an assessment at 36 weeks postmenstrual age, as having: | |
| Mild BPD | Infant breathing room air |
| Moderate BPD | Infant requiring <30% FiO2 |
| Severe BPD | Infant requiring >30% FiO2 or positive pressure ventilation |
Signs and symptoms
- Hypoxemia
- Hypercapnia
- Crackles, wheezing, and decreased breath sounds
- Increased bronchial secretions
- Hyperinflation
- Feeding problems due to prolonged intubation (oral-tactile hypersensitivity/oral aversion)
- Need for continued oxygen therapy after the gestational age of 36 weeks
- Repeated lower respiratory infections that may require hospitalization
- Delayed growth and development
Causes
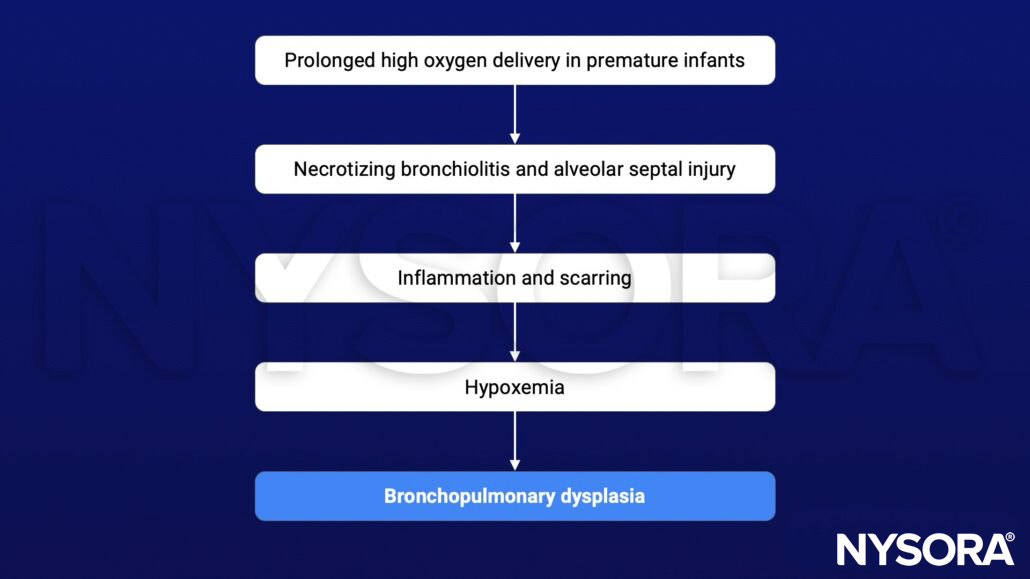
Risk factors
- Antenatal factors
- Prematurity
- Postnatal factors
- Mechanical ventilation
- Sepsis
- Oxygen toxicity
- Patent ductus arteriosus
Complications
- Airway disease and respiratory morbidity due to prolonged tracheal intubation and mechanical ventilation
- Development of tracheomalacia and bronchomalacia
- BPD spells: Acute cyanotic events caused by increases in central airway compliance
- Subglottic stenosis
- Airway granulomas
- Pseudopolyps
- Persistent airway obstruction and hyperreactivity
- Pulmonary hypertension
- Cor pulmonale
Pathophysiology
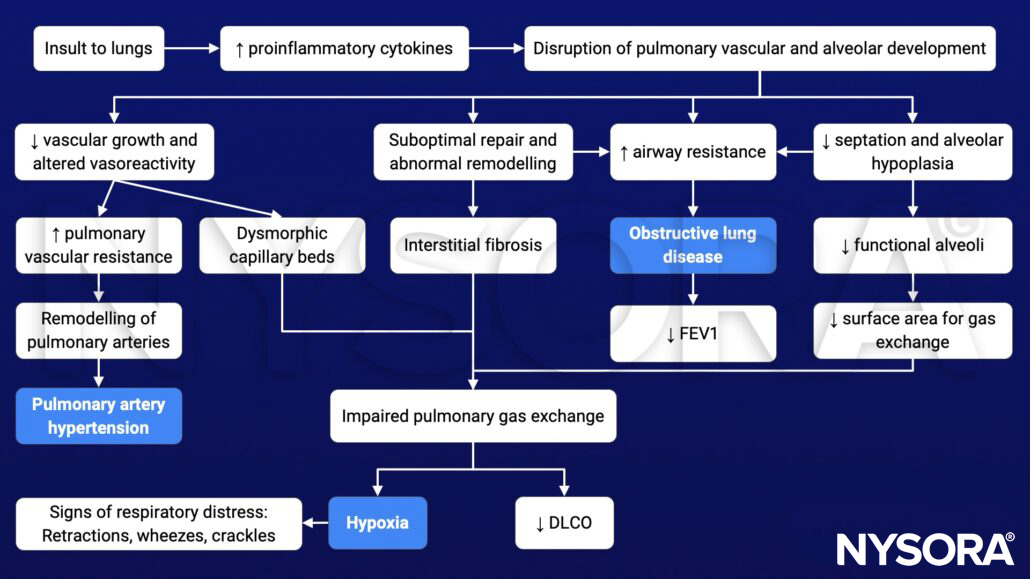
Treatment
- There is no cure for BPD, treatment focuses on minimizing further lung damage and providing support for the infant’s lungs
- Oxygen therapy
- Nasal continuous positive airway pressure (NCPAP)
- Bilevel positive airway pressure (BiPAP)
- Medications
- Diuretics: Decrease fluid in and around the alveoli
- Bronchodilators: Relax the muscles around the air passages, widening the airway openings and making breathing easier
- Corticosteroids: Reduce and/or prevent inflammation within the lungs, reduce swelling in the trachea, and decrease the mucus production
- Viral immunization: Prevent infection (i.e., respiratory syncytial virus)
Management


Prevention
- Antenatal steroid administration
- Surfactant therapy
- Improved ventilator strategies to minimize lung injury
Keep in mind
- BPD is one of the most common pulmonary disorders encountered by pediatric anesthesiologists
- BPD, a common sequala of preterm birth, is associated with persistent airway disease and pulmonary hypertension
- Anesthetic effects might have life-threatening consequences in BPD patients (limited respiratory reserve)
- Intraoperative bronchospasms or airway collapse → hypoxemia, acute pulmonary hypertension, right-sided heart failure, arrhythmias, and death
- Effects on myocardial contractility can impair right ventricular function → reduction in cardiac output and cardiovascular compromise → cor pulmonale
- Respiratory infections (i.e., pneumonia) can further complicate the perioperative course
Suggested reading
- Lauer R, Vadi M, Mason L. Anaesthetic management of the child with co-existing pulmonary disease. BJA. 2012;109(1):i47-i59.
Clinical updates
Recent reviews of neonatal and infant respiratory disease (Current Opinion in Anesthesiology, 2024) emphasize that modern bronchopulmonary dysplasia is driven by disrupted alveolar and pulmonary vascular development, with inflammation and pulmonary hypertension as key determinants of morbidity. The article highlights the importance of lung-protective ventilation, careful oxygen titration, and early recognition of pulmonary hypertension, all of which are critical for perioperative and anesthetic management of infants with BPD.