Etiology
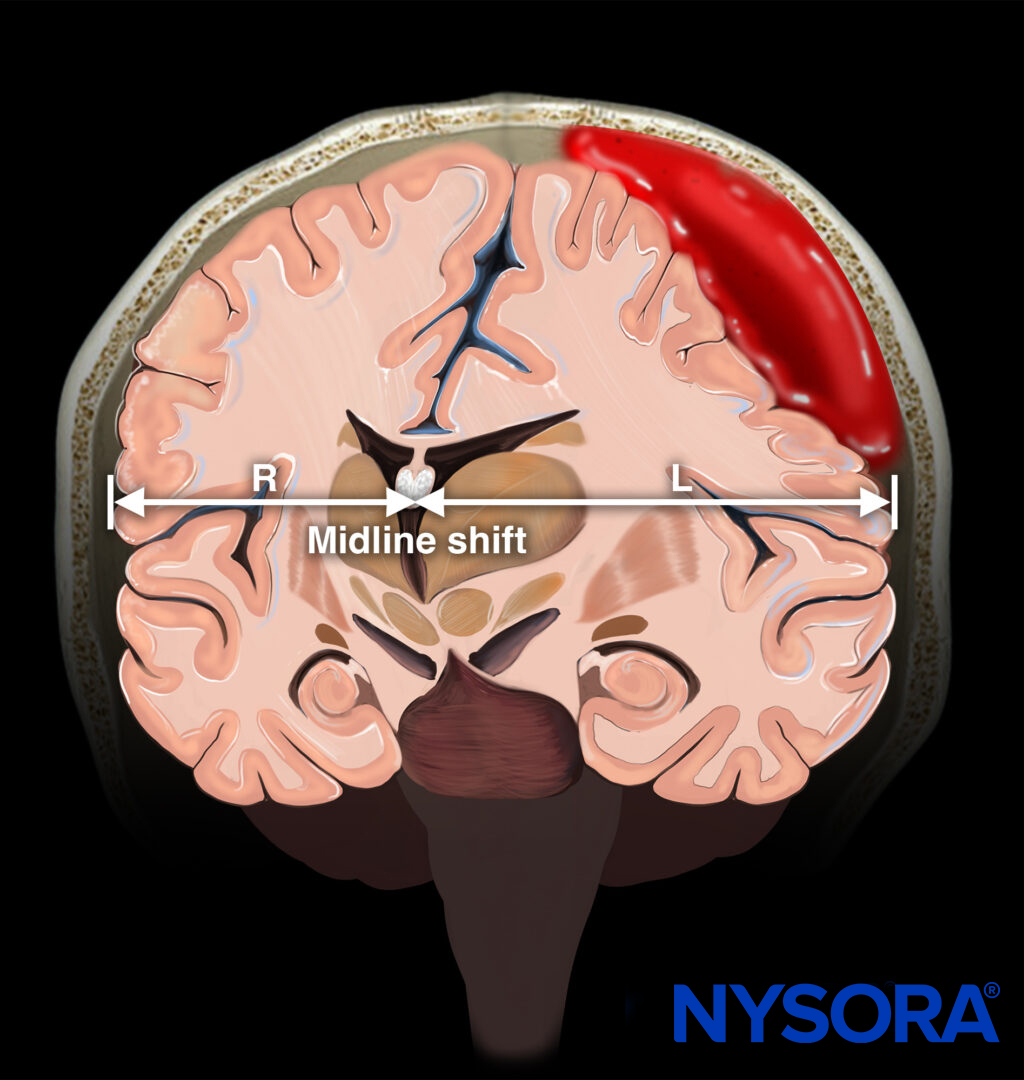
Midline shift results from mass effect and increased intracranial pressure.
All conditions that lead to mass effects can cause midline shifts. Examples are traumatic brain injury, hematoma, stroke, etc.
View

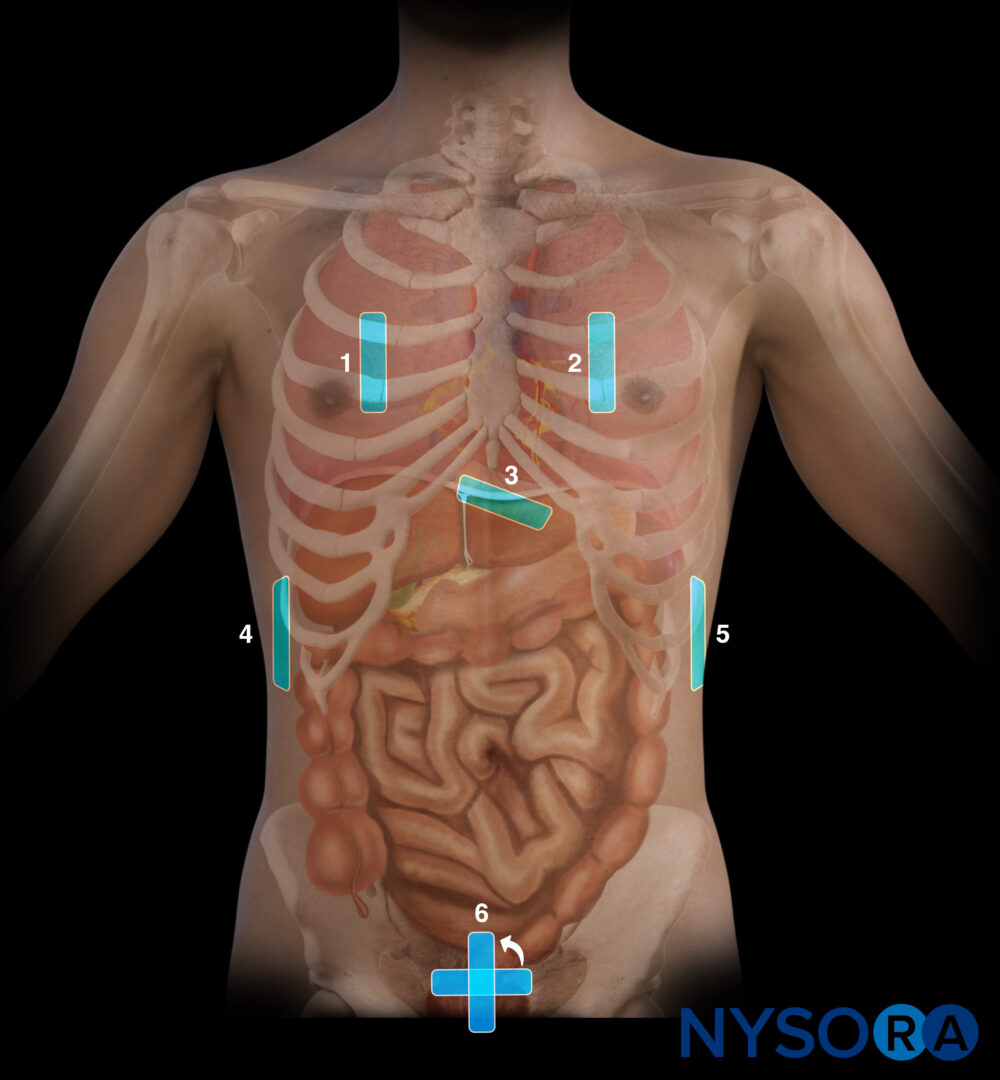
Transducer position for transcranial Doppler examination of midline shift.
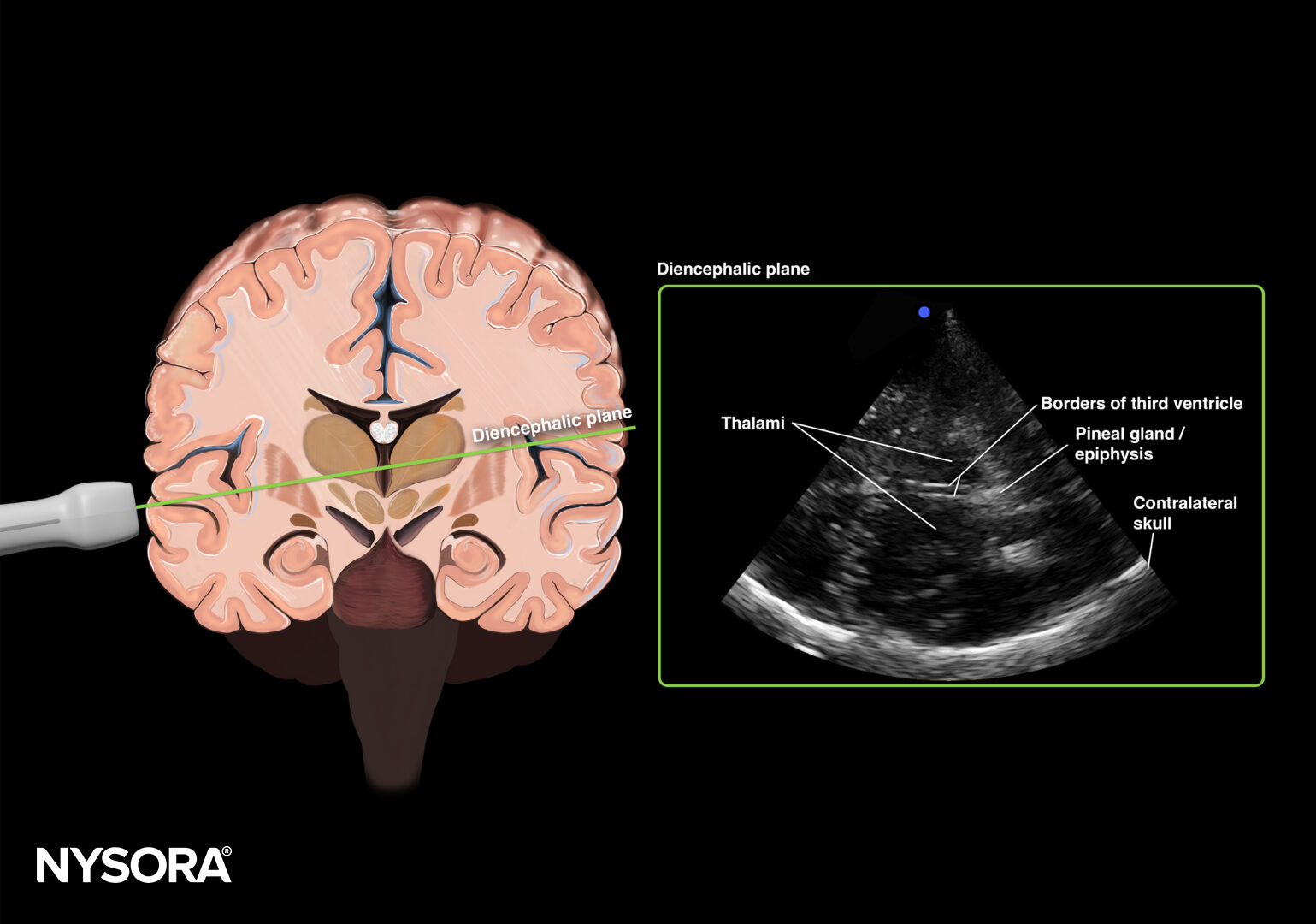
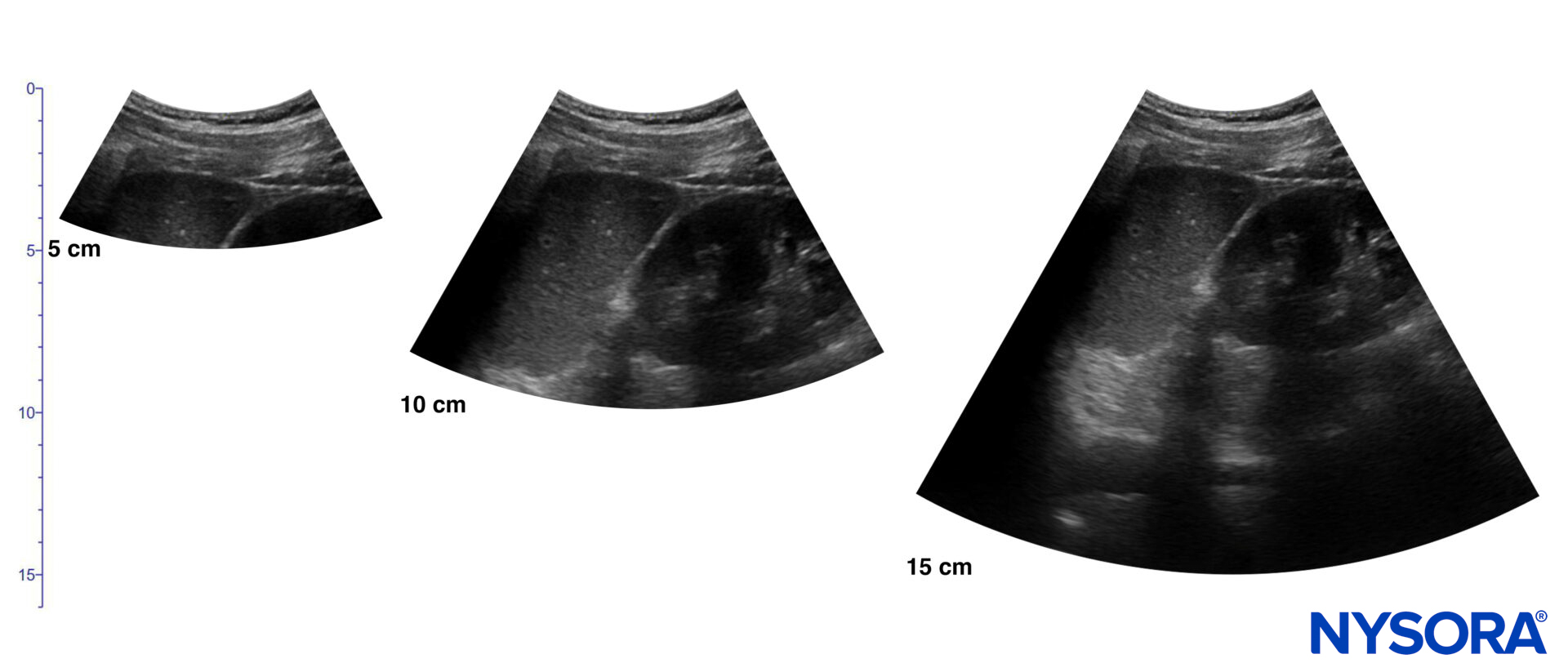
Diencephalic plane.
Assessment
Measure the distance from the transducer to the middle of the third ventricle from both sides (R and L).
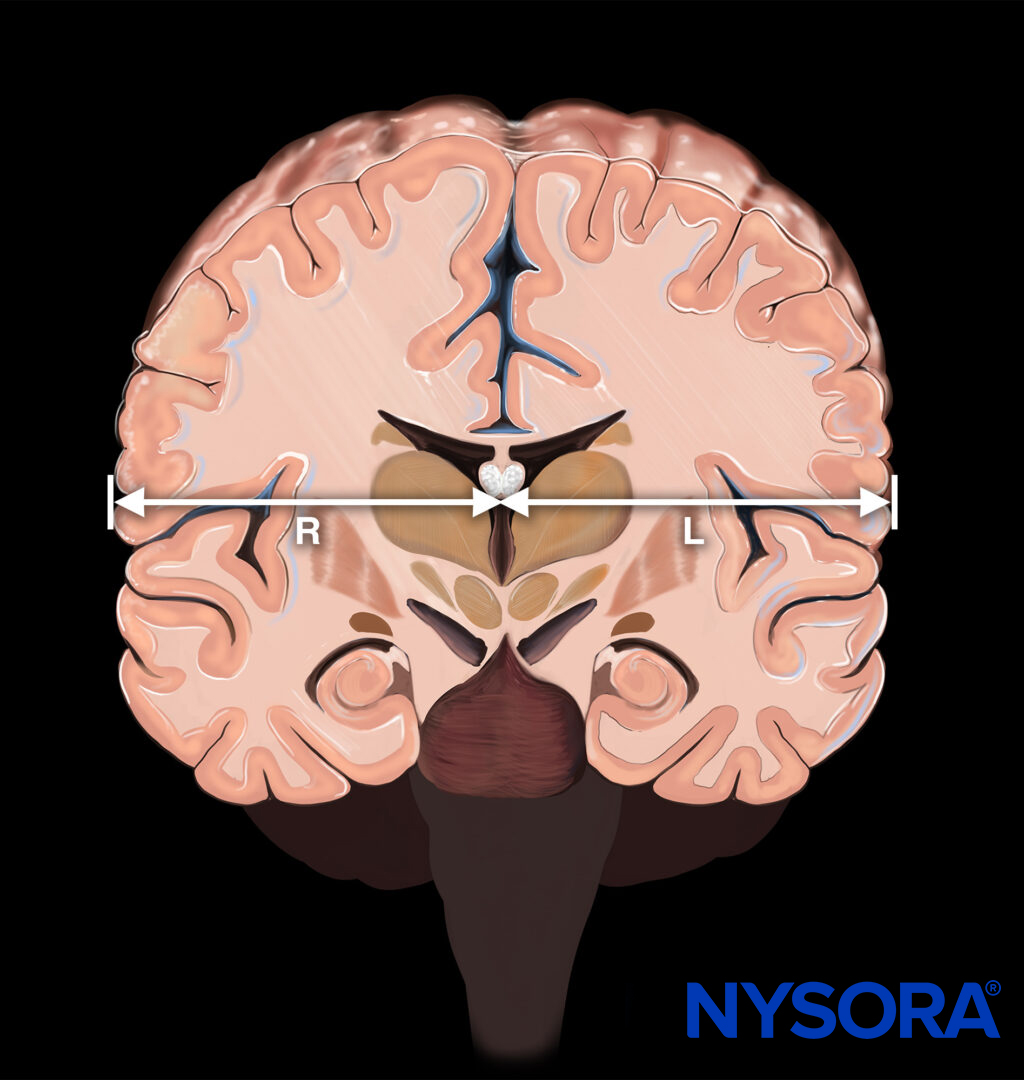
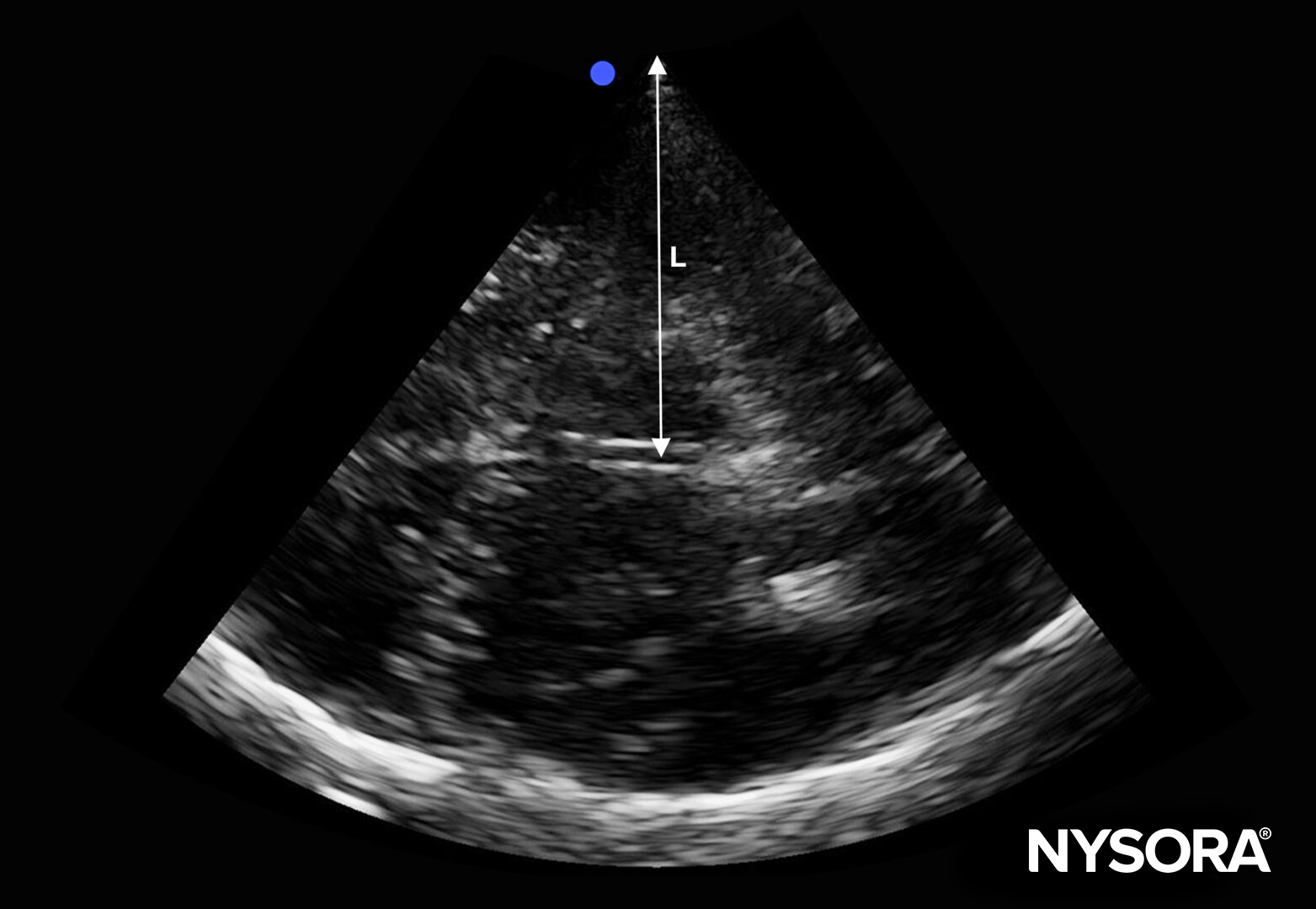
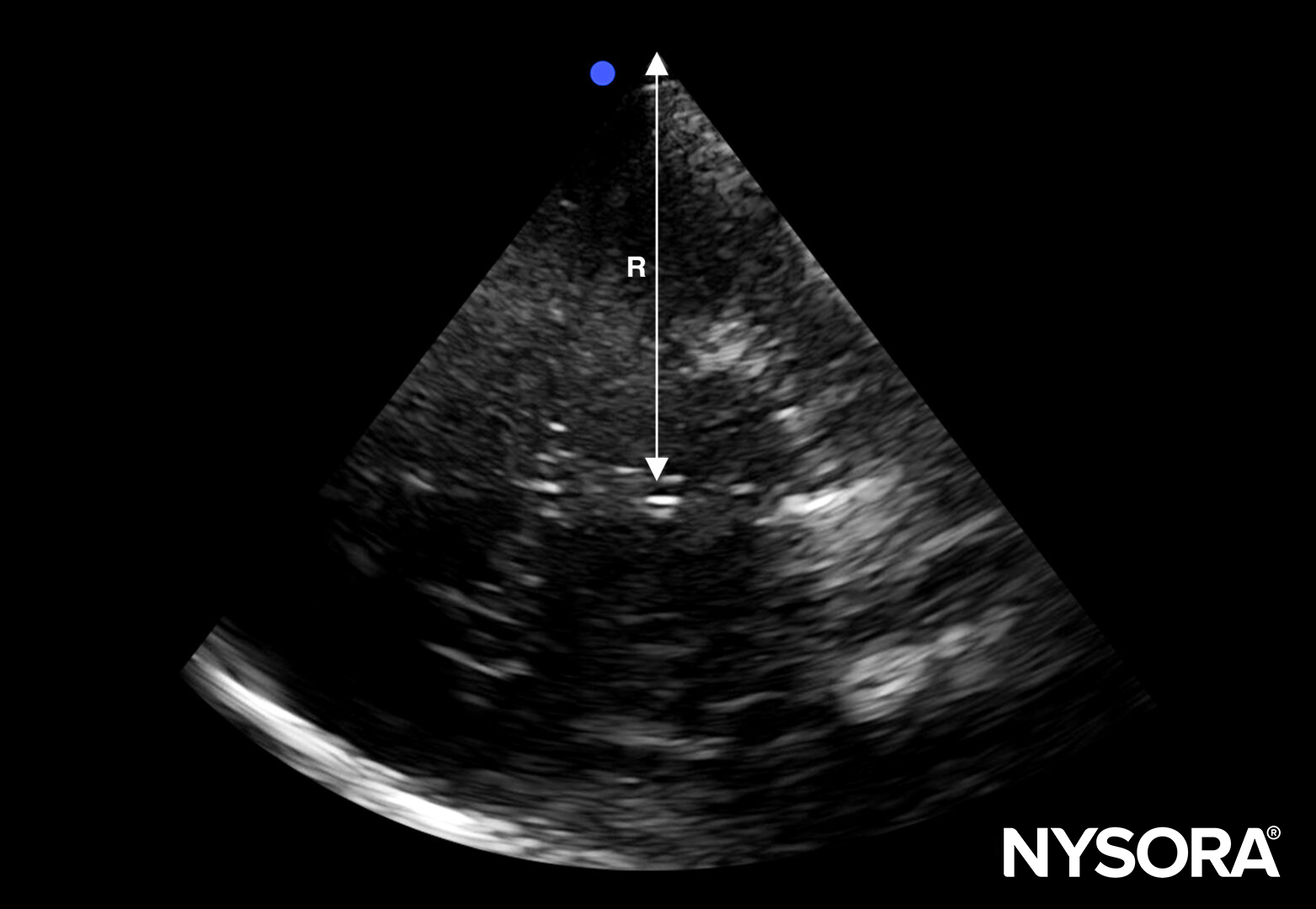
Measure the distance from the transducer to the middle of the third ventricle from both sides. R, distance between the transducer and third ventricle on the right side; L, distance between the transducer and third ventricle on the left side.
Midline shift = (distance R – distance L)/2
Midline shifts of 5 mm or more are considered significant.
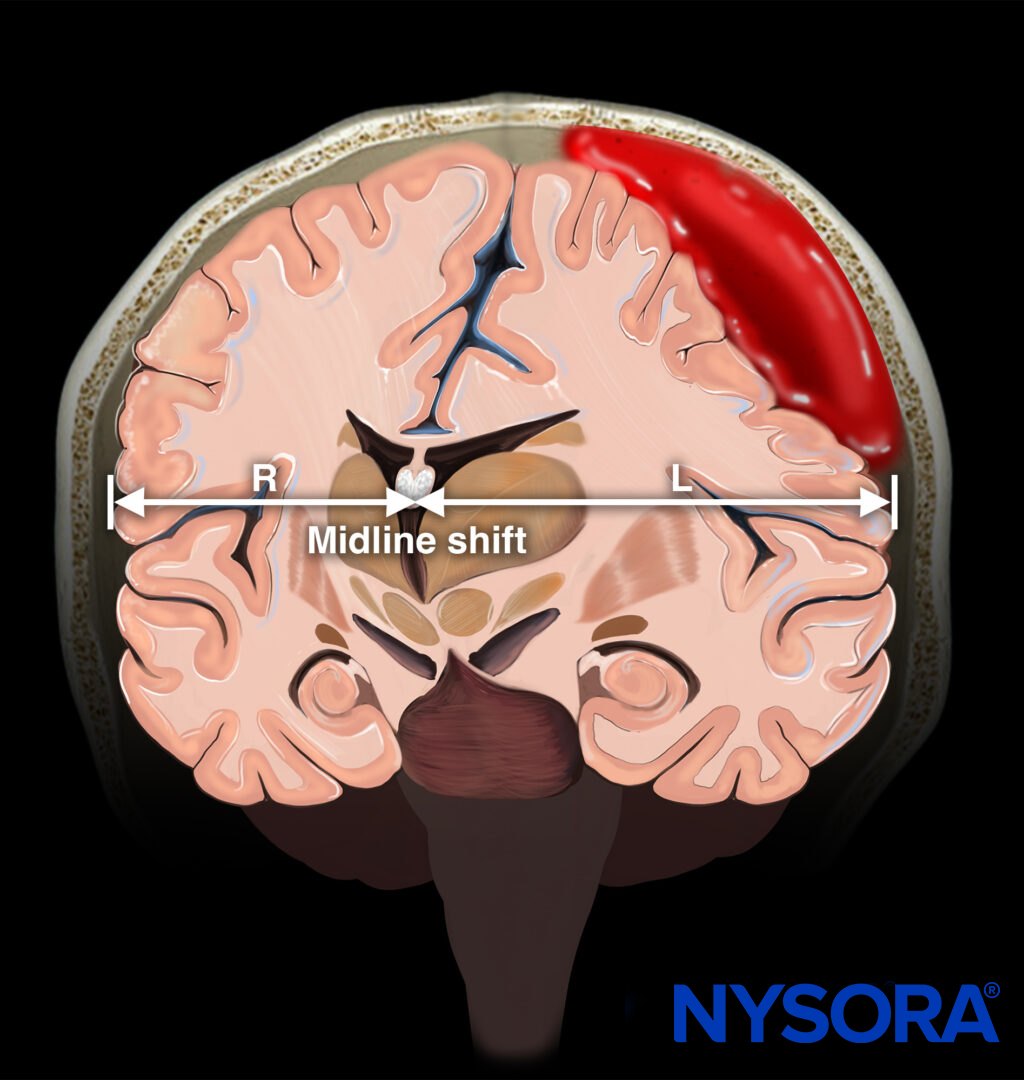
Illustration of a midline shift due to hemorrhage.
Overview
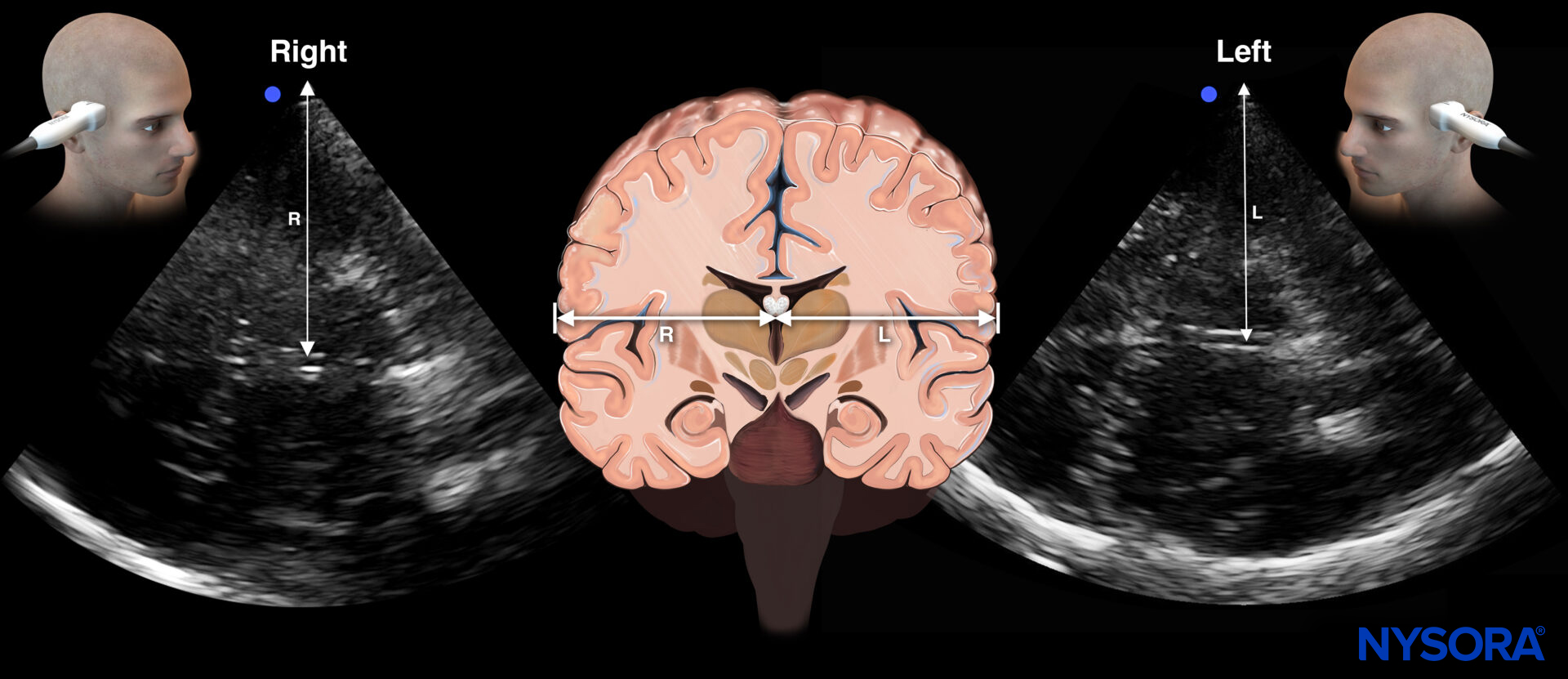
Overview of midline shift assessment using transcranial Doppler.
Exclusion criteria:
- Gross cranial deformities/asymmetries
- Status post decompressive craniectomy
- Cranial fractures
Note
TCD should not replace a CT scan to detect midline shift. It can, however, provide additional information on trends, augment the clinical exam, and trigger further imaging.
Clinical updates
- McKeown et al. (Neurocritical Care, 2022) analyzed 1,977 ischemic stroke patients from multiple trials and registries and found that any midline shift (MLS) independently predicted poor 3-month outcome (adjusted OR 2.33), even after controlling for age, NIHSS, stroke volume, and reperfusion therapy. Importantly, they identified >3 mm MLS as the minimal clinically significant threshold, with MLS >3–4 mm associated with poor outcome (aOR 3.20), whereas 2–3 mm MLS was not significant, supporting 3 mm as a critical cutoff for clinically meaningful edema-related mass effect.
- McKeown ME, Prasad A, Kobsa J, et al. Midline Shift Greater than 3 mm Independently Predicts Outcome After Ischemic Stroke. Neurocrit Care. 2022;36(1):46-51