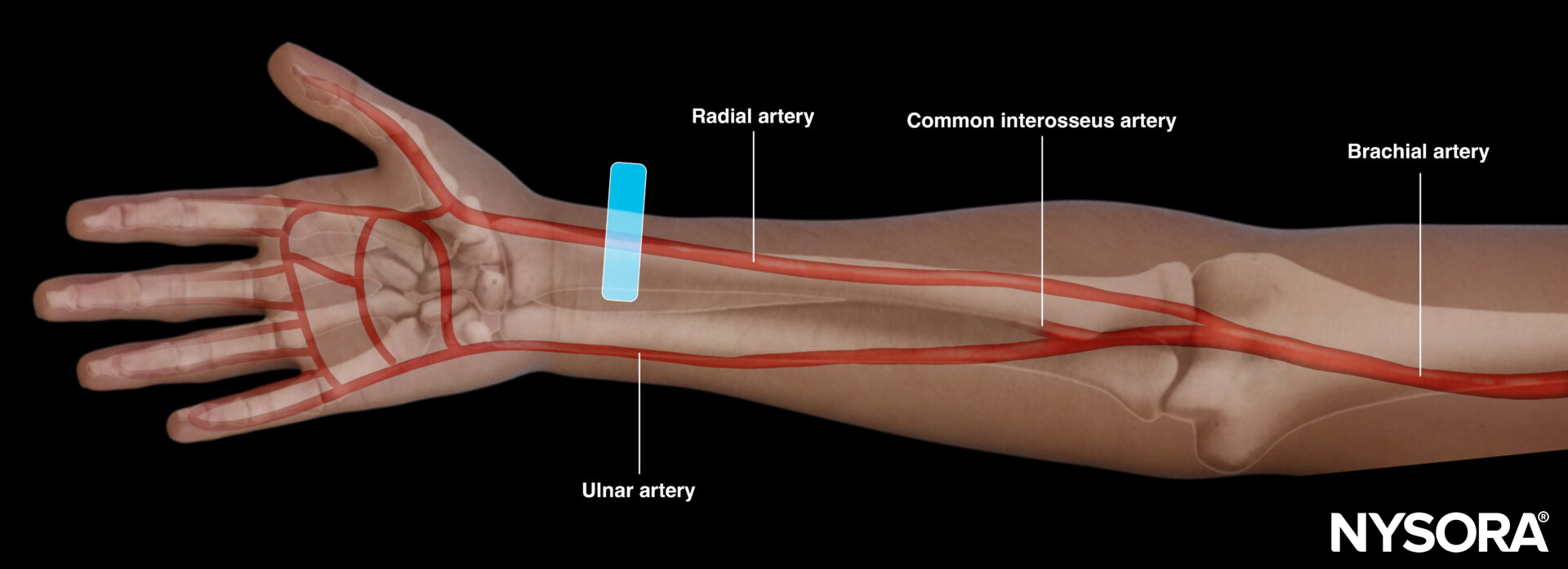
Indications
The FALLS (Fluid Administration Limited by Lung Sonography) protocol is a suggested approach for acute circulatory failure or undifferentiated shock (obstructive, cardiogenic, hypovolemic, distributive). Next to a simple cardiac ultrasound to rule out pericardial tamponade or pulmonary embolism (right ventricle dilatation), it uses the BLUE protocol as well as fluid therapy to guide the type of shock.
The FALLS protocol
The FALLS protocol consists of three steps:
1. Cardiac ultrasound should be used to diagnose obstructive shock by checking for tamponade or right ventricle dilatation.
- The subcostal four-chamber view is excellent to rule out tamponade. In the presence of a tamponade, the heart is surrounded by an anechoic layer. More info on tamponade can be found in the cardiac category.
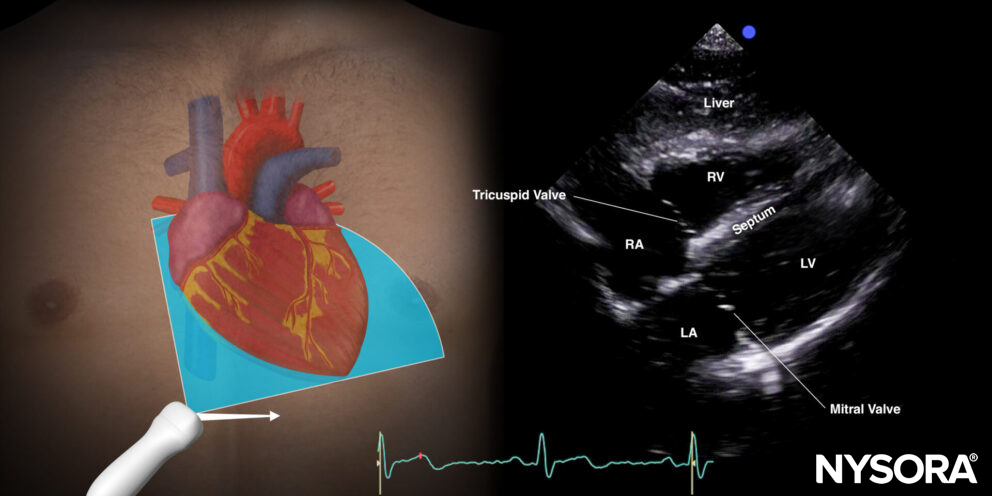
Subcostal four-chamber view.
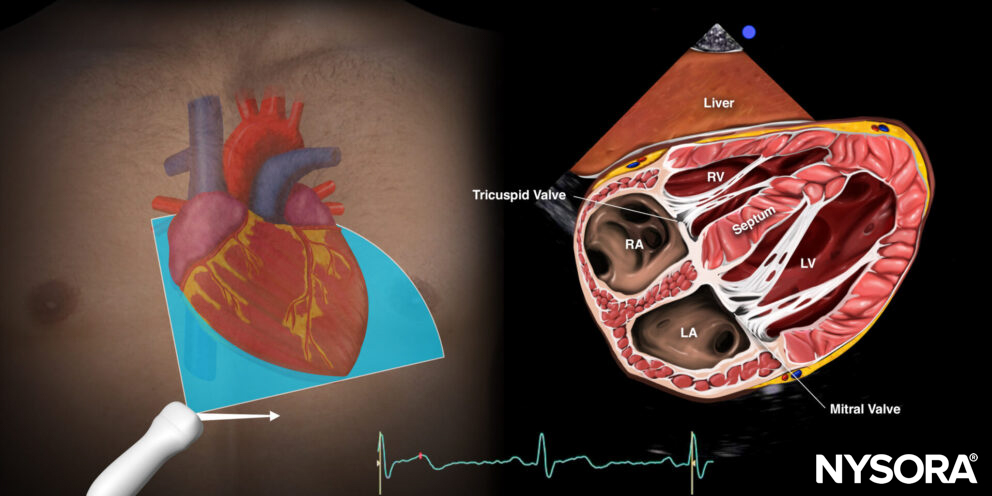
Reverse Ultrasound Anatomy of the subcostal four-chamber view.
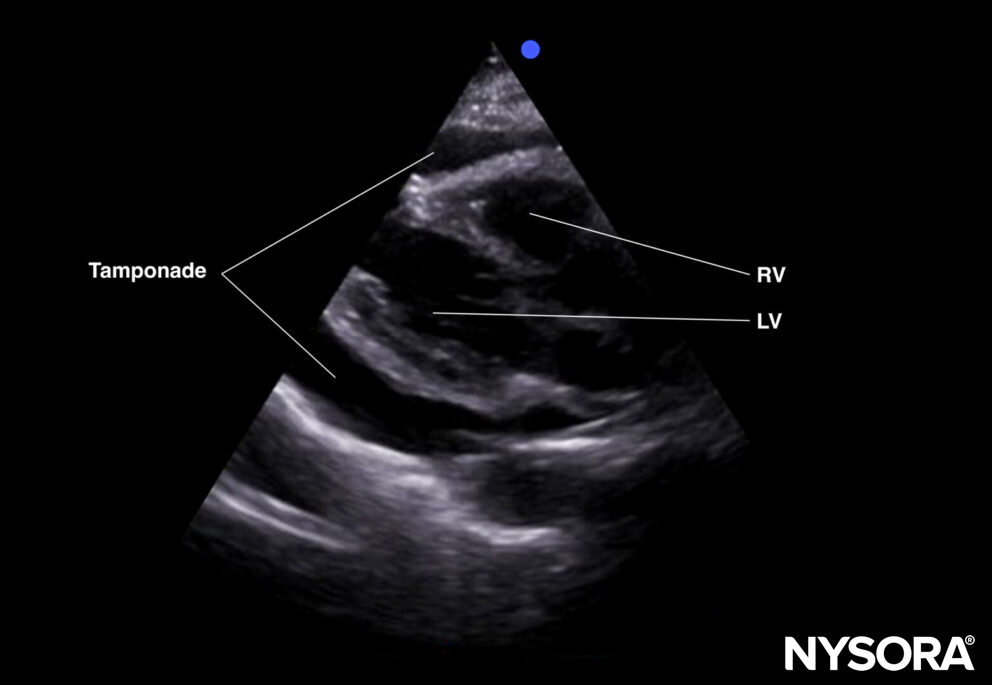
Subcostal four-chamber view of a tamponade.
- To rule out right ventricle dilatation, it is best to use the parasternal short-axis view. The right ventricle should have a crescent shape. High right ventricular pressures will cause the septum to bulge into the left ventricle. This is also called left ventricular D-shaping.
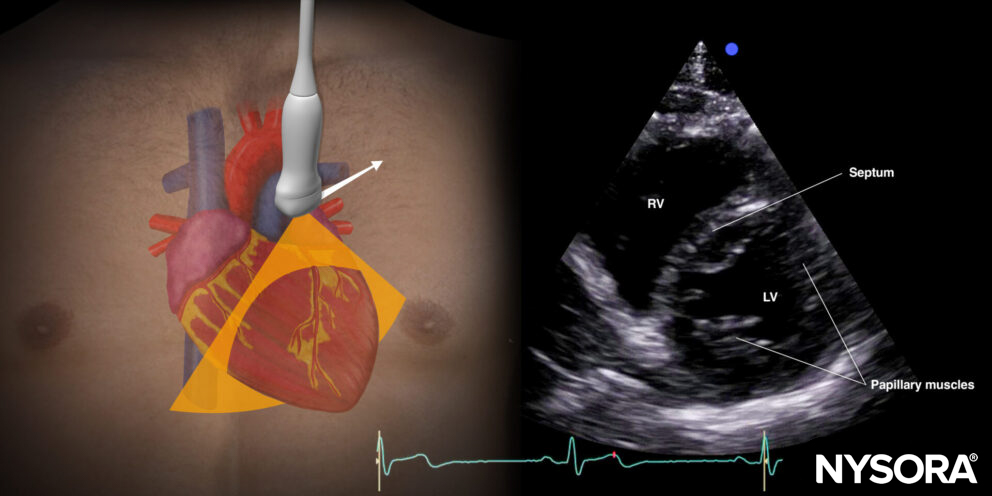
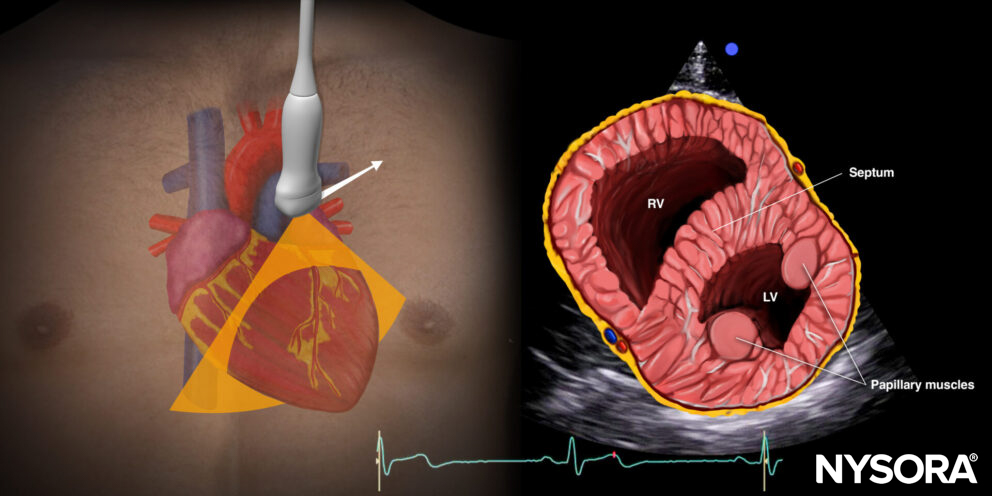
Ultrasound and Reverse Ultrasound Anatomy of the parasternal short-axis view
2. If the cardiac exam is normal, use the BLUE protocol to further differentiate the type of shock. In the presence of acute circulatory failure and an A’-profile (tension pneumothorax), you are dealing with obstructive shock. A B-profile (pulmonary edema) will be present in cardiogenic shock.
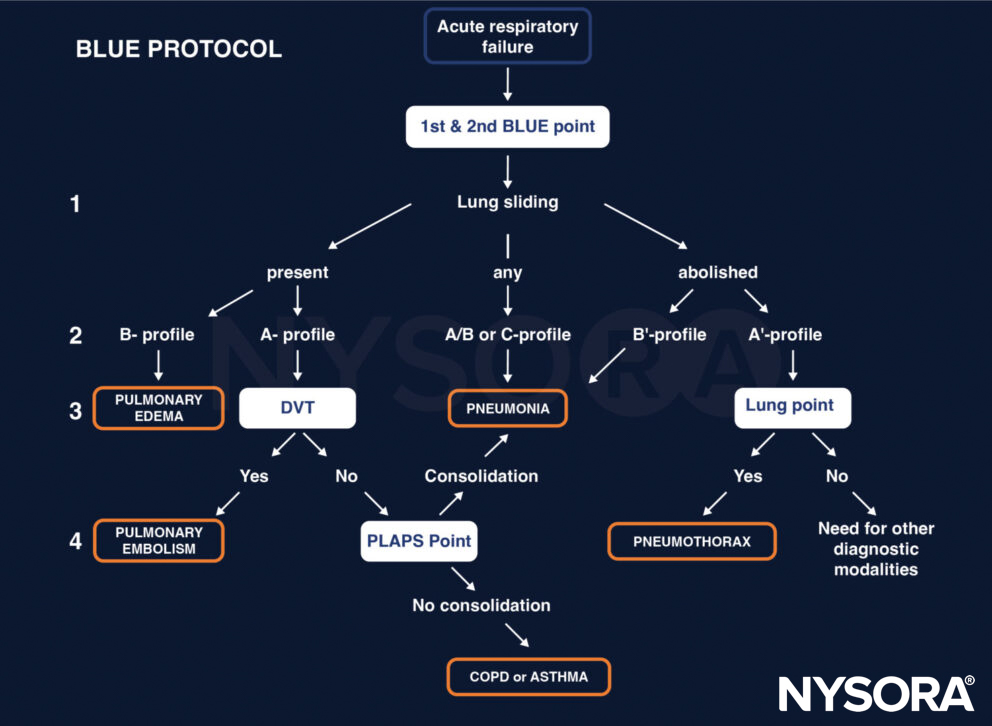
The BLUE protocol. Adapted from D. Lichtenstein.
3. The final step requires an A-profile and the start of fluid therapy. If there is clinical improvement, you are dealing with hypovolemic shock. If there is no clinical improvement, repeat the BLUE protocol. If a B-profile is now present, you are dealing with distributive shock.
Summary
This overview illustrates how the FALLS protocol can be used to differentiate between the different types of shock in the setting of acute circulatory failure.
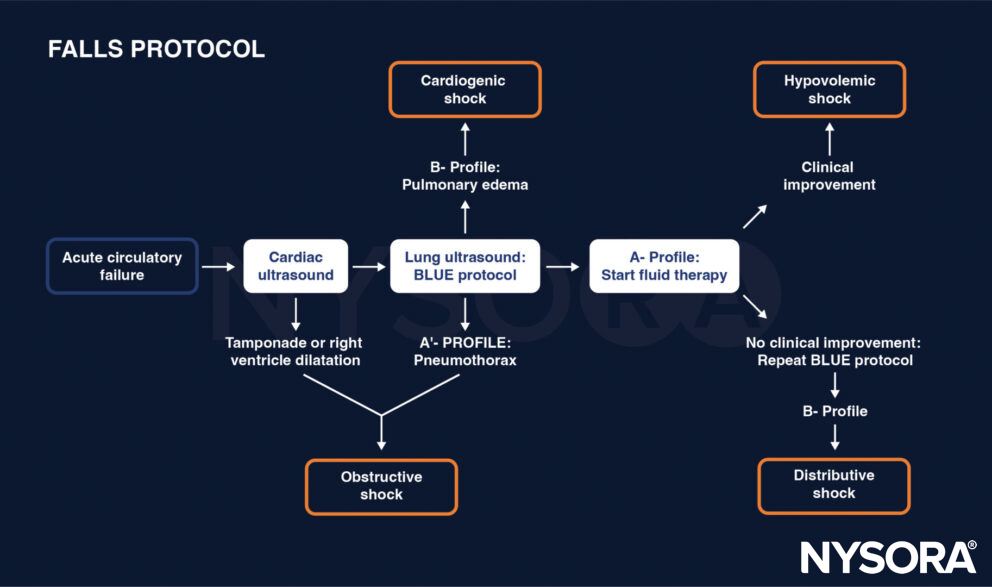
The FALLS protocol. Adapted from D. Lichtenstein.
Note
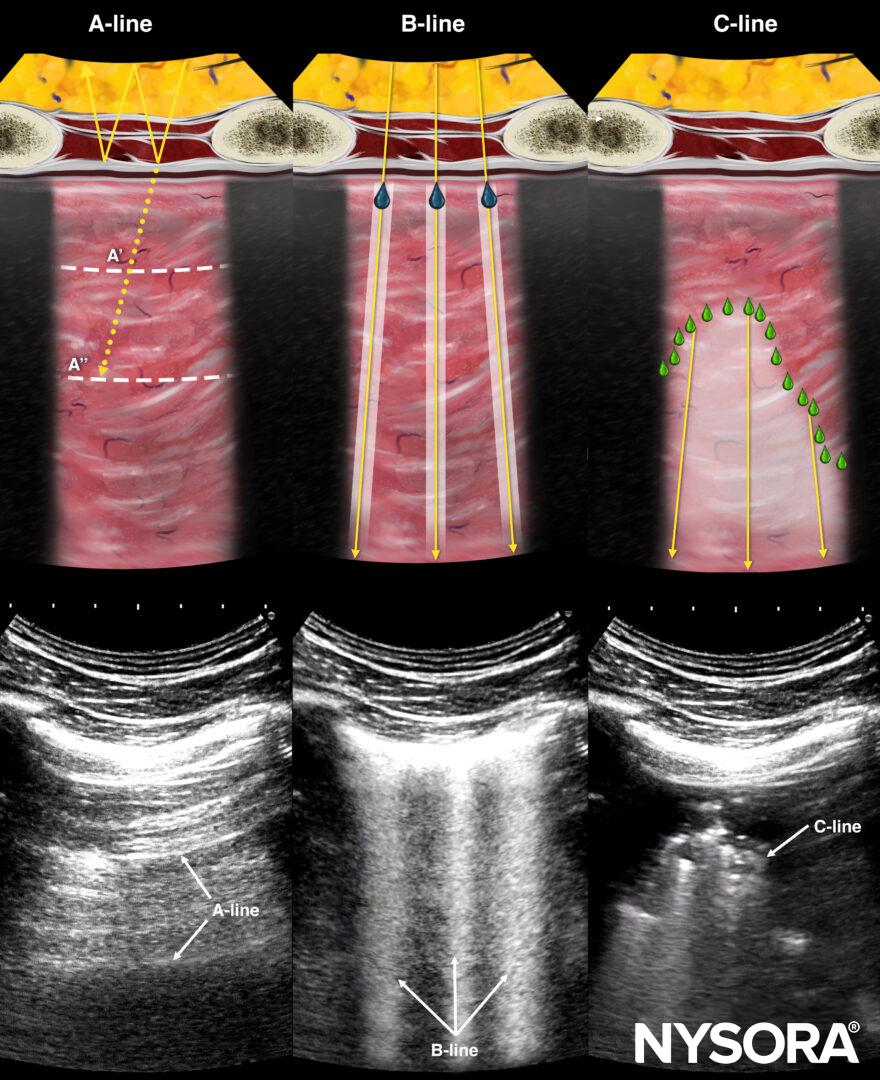
The fluid administration within the FALLS protocol is based on the fact that A-lines transform into B-lines at pulmonary artery occlusion pressures of 18 mmHg. This allows the use of lung ultrasound to directly assess lung water in critically ill patients.
Tips
- Patients presenting with B-lines on admission may show no transformation from A-lines to B-lines. This is one of the main limitations of the FALLS protocol.
- The correlation between an A-profile and a pulmonary artery occlusion pressure of 18 mmHg or less has 93% specificity and 97% positive predictive value.
- It is important to remember that the FALLS protocol is a direct product of the BLUE protocol. It is important to understand that it indicates a high likelihood of the type of shock, which is not 100%.
Clinical updates
Yoshida et al. (Critical Care, 2023) performed a systematic review and meta-analysis of 12 studies (n=1132) evaluating POCUS for undifferentiated shock and found high diagnostic accuracy across shock types, with pooled sensitivity/specificity of 0.82/0.98 for obstructive, 0.78/0.96 for cardiogenic, 0.90/0.92 for hypovolemic, and 0.79/0.96 for distributive shock; AUCs were ~0.95 and positive likelihood ratios exceeded 10 for all types, reaching 40 for obstructive shock . Specificity and LR+ were particularly strong for obstructive shock, supporting a protocol prioritizing early identification of obstructive causes (e.g., tamponade, PE, pneumothorax) during initial POCUS assessment.
- Yoshida T, Yoshida T, Noma H, Nomura T, Suzuki A, Mihara T. Diagnostic accuracy of point-of-care ultrasound for shock: a systematic review and meta-analysis. Crit Care. 2023;27(1):200.