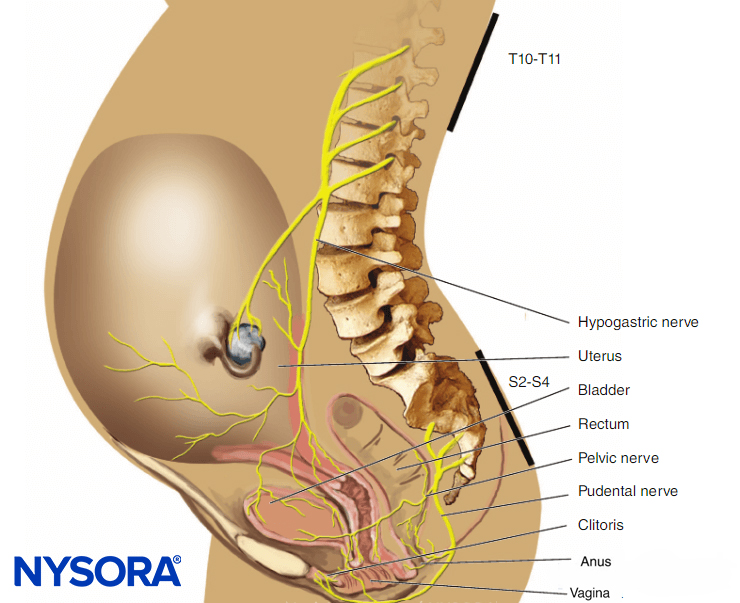
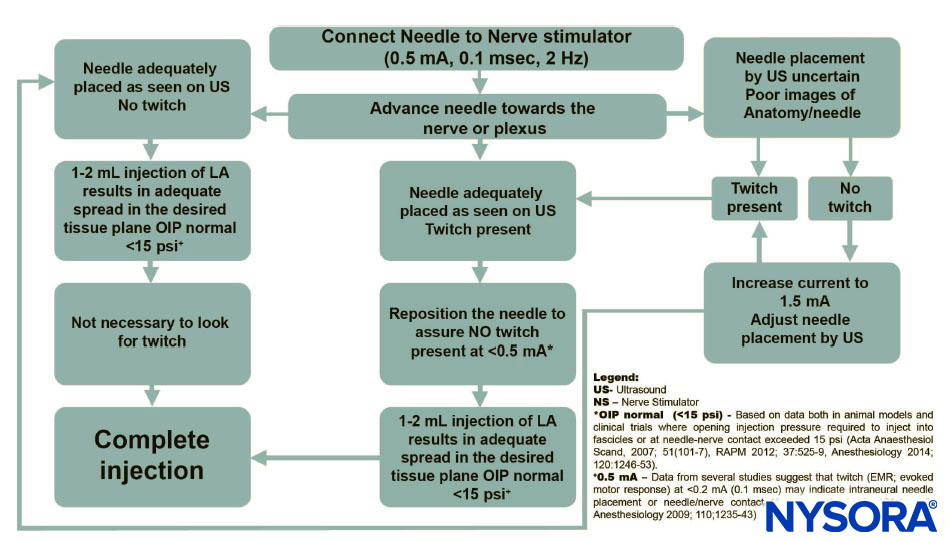
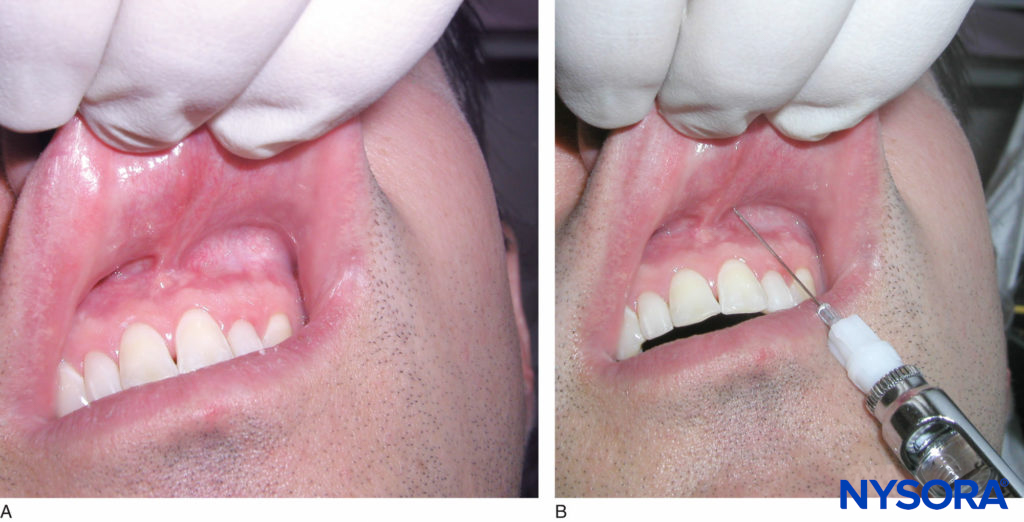
INTRODUCTION
Infectious complications related to regional anesthesia are rare. Because most of the information is available in case reports and retrospective surveys, it is likely that these complications are underreported. It is hoped that recent surveillance and prospective registry projects using standardized surveillance definitions and the integration of such in national quality assurance projects (American Society of Regional Anesthesia [ASRA] Acute-POP/AQI) will generate more comprehensive data for risk assessment and evaluation of infection control recommendations in the future. Integration of a structured surveillance tool into the electronic medical record and a hospital’s quality management system will ease the workload for clinicians and facilitate surveillance compliance (Table 1).
While we have to work on reducing infectious complications associated with regional anesthesia because of the potential severe individual consequences, some studies demonstrate a reduction of surgical site infections with the use of local anesthesia—opening the research arena regarding whether the avoidance of general anesthesia, intrinsic properties of local anesthetics, or a combination of both is responsible for this observation.
The objective of this chapter is to summarize information from the literature on infections complications associated with regional anesthesia, as well as to discuss the mechanism and suggest strategies to prevent these complications.
PATHOGENESIS OF INFECTIONS ASSOCIATED WITH CENTRAL NEURAXIAL block
Microorganisms from exogenous or endogenous sources may gain access to the subarachnoid, epidural, or tissue space surrounding peripheral nerves in several ways. Microorganisms from the patient’s or anesthesia practitioner’s flora can be inoculated directly when a catheter or needle is inserted into those spaces. Several reports in the literature suggested that infections are on occasion caused by the anesthesia practitioner’s flora. For example, Trautmann and colleagues reported a case of meningitis caused by a Staphylococcus aureus strain that was identical by pulsed-field gel electrophoresis to the S. aureus isolated from the anesthesiologist’s nose. Rubin et al could trace to a single anesthesiologist Streptococcus salivarius as the responsible agent for six cases of meningitis following spinal anesthesia, and the Centers for Disease Control and Prevention (CDC) reported five cases in Ohio and one case in New York between 2008 and 2009 with the same organisms.
Microorganisms can also enter the epidural space by hematogenous spread from other body sites, such as infected skin, or by migrating along the catheter tract. Several case reports suggested that infection was caused by spread of bacteria from infected sites through the bloodstream to the epidural space. Others maintained that infections at distal sites are not contraindications to epidural anesthesia. For example, Newman concluded that distal infections did not increase the risk of epidural infection because traumatic injuries are often infected, and no epidural catheter-related infections were identified among over 3000 patients who had epidural neural blocks for postoperative or posttraumatic analgesia. Gritsenko and coworkers analyzed the charts of 474 patients who underwent removal of an infected hip or knee prosthesis under neuraxial anesthesia and found in 0.6% of the cases clinical signs of central neuraxial infections (meningitis or epidural abscess) and three other anesthesia-related complications, including a psoas abscess beside an epidural hematoma and back pain.
TABLE 1. Regional anesthesia surveillance system complication denitions.
| A: Essential Criteria | B: Contributory Criteria | |
|---|---|---|
| Epidural infection | ||
| EI1: Superficial soft tissue infection 2 A and B criteria needed | Swelling Local tenderness | Fever (>38.0°C) Drainage Positive culture from the area Leukocytosis (>12/nL or CRP > 20 mg/L) Local erythema |
| EI2: Epidural abscess 1 A and 3 B criteria needed | Radiological evidence of a mass in the epidural space consistent with an epidural abscess within 30 days after epidural/spinal needle/catheter placement/catheter removal or attempted epidural/spinal placement | Fever (>38.0°C) Drainage Positive culture from surgical exploration or puncture Leukocytosis (12/nL or CRP > 20 mg/L) Local erythema Local tenderness Focal back pain Neurologic deficita |
| EI2Na | Same as above: Classified as EI 2 N if neurologic deficit is present as a contributory criterion | |
| EI3: Epidural infection with sepsis 1 A and 4 B criteria needed | Diagnostic criteria of EI1 or EI2 or EI2Na puncture site or abscess | Positive blood culture with the same organism isolated from Fever > 38.0°C or hypothermia < 36°C Leukocytosis > 12 nL or leukopenia < 4 nL BP systolic < 90 mm Hg Tachycardia > 90 bpm Respiratory failure (AF > 20, paCO2 < 32 mm Hg, PaO2 < 70 mm Hg breathing spontaneously or PaO2 /FiO2 < 175 on mechanical ventilation) |
| EI3N | Same as above: Classified as EI3N if EI2Na criteria are present | |
| Peripheral nerve block–associated other infection | ||
| OI1: Superficial soft tissue infection | Swelling along the catheter or needle placement track Local tenderness along the catheter or needle placement track | Fever (>38.0°C) Drainage Positive culture from the area Leukocytosis (>12/nL or CRP > 20 mg/L) Local erythema |
| OI2: Abscess or deep tissue infection | Evidence of an abscess or fluid collection consistent with an infectious process by imaging or surgical exploration within 30 days after peripheral nerve block needle placement/catheter removal or attempted placement | Fever (>38.0°C) Drainage Positive culture from surgical exploration or puncture Leukocytosis (>12/nL or CRP > 20 mg/L) Local erythema Local tenderness Focal back pain Neurologic deficita |
| OI2Na | Same as above: Classified as OI2N if neurologic deficit is present as contributory criterion | Positive blood culture with the same organism isolated from puncture site or abscess Fever > 38.0°C or hypothermia < 36°C Leukocytosis > 12 nL or leukopenia < 4 nL BP systolic < 90 mm Hg Tachycardia > 90 bpm Respiratory failure (AF > 20, PaCO2 < 32 mm Hg, PaO2 < 70 mm Hg breathing spontaneously or PaO2/FiO2 < 175 on mechanical ventilation) |
| OI3: Infection with sepsis 1 A and 4 B criteria needed | Diagnostic criteria of OI1 or OI2 or OI2Na | Positive blood culture with the same organism isolated from puncture site or abscess Fever > 38.0°C or hypothermia < 36°C Leukocytosis > 12 nL or leukopenia < 4 nL BP systolic < 90 mm Hg Tachycardia > 90 bpm Respiratory failure (AF > 20, PaCO2 < 32 mm Hg, PaO2 < 70 mm Hg breathing spontaneously or PaO2/FiO2 < 175 on mechanical ventilation) |
| OI3N | Same as above: Classified as OI3N if OI2Na criteria are present | New onset of central neurologic symptoms Headache Stiff neck Fever > 38.0°C Positive CSF culture Meningitis-specific antibiotic therapy started Spinal or epidural block (catheter insertion/ removal) in the past 72 h |
| Neurologic deficit | ||
| ND1: Neurologic deficit | Residual sensory and/or motor and/or autonomic block 72 h after last injection of local anesthetic without other identifiable etiology New onset of sensory and/or motor and/or autonomic deficit 24 h after resolution of the original block without other identifiable etiology If regional anesthetic-/analgesia-related infection is present classify, as EIXN/OIXNa | Electrophysiological evidence of new nerve damage (MEP, SEP, nerve conduction study, electromyography) |
| 2 A and 1 B criteria needed | New loss of deep tendon reflexes New loss of vibration sensation New onset of neuropathic pain in affected nerve distribution area Paresthesia in affected nerve distribution area Sensory and/or motor and/or autonomic deficit consistent with dermatomes or nerve distribution area |
|
NYSORA Tips
- Streptococcal species, S. aureus, and Pseudomonas aeruginosa are the most common causative agents but multiresistant species also emerge as causative pathogens as their endemic impact grows within health-care systems.
- Microorganisms from the patient’s or anesthesia practitioner’s flora can be inoculated directly when a catheter or needle is inserted into the epidural or subarachnoid space.
- Because it is easy to contaminate the needle or the catheters, aseptic measures.
The anesthetic agents injected into the subarachnoid or epidural space are another possible source of infection. Infections from contaminated multidose vials are likely rare because most anesthetic drugs are weak bases dissolved in acidic solutions that inhibit growth of bacteria and fungi. Besides most multidose local anesthetic solutions contain a bacteriostatic agent. Nevertheless, the case report by North and Brophy suggested that contaminated multidose vials still can be a source of infection. These authors reported an infection in which S. aureus with matching phage types were Isolated from an abscess and a multidose lidocaine vial.
A report by Wong et al described, besides other infection control violations, the use of single-dose medications for multiple patients as the culprit in an outbreak of Klebsiella pneumoniae and Enterobacter aerogenes bacteremia in a pain clinic. Breaches in aseptic technique for medication preparation can be detrimental, especially if a compound pharmacy is involved: In 2012, more than 200 patients suffered fungal infections with Exserohilum rostratum after use of contaminated methypred-nisolone injections for interventional pain procedures in multiple institutions in the United States.
To assess whether contamination of the anesthetic agent or the equipment (needles, syringes, tubing) is related to subsequent infections, investigators have cultured these items after they have been used with patients or during simulations. In four studies, 0%–29% of used catheters were contaminated, and James and coworkers found that 5 of 101 syringes used to inject anesthetic agents were contaminated. Ross and coworkers drew up 0.25% bupivacaine into control syringes and into syringes used to induce continuous lumbar epidural neural block (test syringe) in 18 obstetric patients. After each dose from the test syringe, the investigators cultured the contents of both the test and the control syringes. Six of 18 test syringes were contaminated with bacteria, compared with only 1 of 18 control syringes. Raedler and associates cultured 114 spinal and 20 epidural needles after use for single lumbar injections. Twenty-four cultures (17.9%) grew microorganisms: 15.7% coagulase-negative staphylococci; 1.5% yeasts; and 0.8% each enterococci, pneumococci, and micrococci. The authors concluded that it is easy to contaminate the needle, and that anesthesiologists need to improve their hygienic measures. Despite finding contaminated equipment or anesthetic solutions, no infected patient was identified; thus, none of the authors was able to correlate contamination with infection. However, Loftus and coworkers examined the contamination of intravenous stopcocks during general anesthesia and showed, for the first time, postoperative infections with the same organism. It is therefore conceivable that contamination during the placement of a regional block, and, even more likely, during handling of continuous catheter systems, can cause infections. Although the risk for such infections would be less likely than that of manipulating intravenous lines.
INFECTIONS ASSOCIATED WITH EPIDURAL block
The numerous case reports in the literature of infections occurring after epidural neuraxial block, attest to the fact that such complications do occur and can be severe (Table 2). Of 57 patients in these case reports, 41 acquired epidural or intraspinal abscesses, 1 developed a subcutaneous abscess, 2 had meningitis without epidural abscess formation, and 1 developed sepsis. Four patients had injections only, 1 patient had injections and several catheters, and the remaining patients had catheters. Among the 38 patients who had catheters and for whom the duration of catheterization was specified, the median duration of catheteriza-tion was 3 days (range 50 minutes to 6 weeks). The median time to onset of the first signs or symptoms of infection was 4 days (range 1 day to 4.8 months) after catheter placement. Staphylococcus aureus caused 27 of 43 infections from which bacterial pathogens were isolated. Pseudomonas aeruginosa caused five infections and Streptococcus spp. caused five. Methicillin-resistant S. aureus (MRSA) was isolated in one case; three patients died.
NYSORA Tips
- Epidural catheters inserted for long-term pain control become infected more frequently than those used for short periods of time.
- Malignancy and reduced immunocompetence might be additional risk factors for catheter infection.
- Case reports of infections occurring after epidural neuraxial block point out that complications from infection can be severe and often lead to epidural or intraspinal abscesses.
It should be kept in mind that the number of reported cases does not allow us to assess the true frequency of infections after epidural neural block. However, several investigators have performed studies to assess this risk. When reviewing 350 reports in the literature, Dawkins in 1969 found no reports of infection after thoracic or lumbar epidural block but identified 8 (0.2%) reports of infection after 3767 sacral epidural blocks used for operative procedures and for obstetrics. More recently, Dawson reviewed the literature and found rates of deep infection ranging from 0% to 0.7% and rates of superficial infection ranging from 1.8% to 12%.
TABLE 2. Infections associated with epidural neural block.
| Author (Reference) | Year | Indication | Epidural Site | Filter Used | Catheter Duration | Type of Infection | Time From Insertion to Symptoms | Signs and Symptoms | Microorganism | Outcome |
|---|---|---|---|---|---|---|---|---|---|---|
| Edwards and Hingson31 | 1943 | Vaginal delivery | Caudal | NS | NS | Epidural abscess, bacteremia | NS | NS | Staphylococcus aureus | Died 31 days after delivery |
| Ferguson and Kirsch32a | 1974 | Postoperative analgesia | Thoracic | NS | 2 days | Epidural empyema | 4 days 10 days 14 days | Fever, headache, meningism Urinary retention Paraparesis | Staphylococcus epidermidis | Sensory impairment, spastic weakness, walks with crutches |
| Saady33a | 1976 | Postoperative analgesia | Thoracic | Yes | 1.7 days | Epidural abscess | 4 days 8 days 9 days 10 days 14 days | Fever Chills, abdominal pain right upper quadrant Headache, stiff neck Urinary retention Lower extremity paraparesis, no anal tone | S. aureus | Sensory impairment, walks with minimal assistance |
| North and Brophy7 | 1979 | 1. Priapism | Lumbar | No | 3 days | Epidural abscess | 1 day | Fever Stiff neck, dysphagia, back pain, absent ankle jerks | S. aureus | Full recovery |
| 2. Fractured ribs, chest injury | Thoracic | Yes | 4 days | Epidural abscess | 10 days | Fever Stiff neck, sensory loss T2 to T6 | S. aureus | Sensory impairment | ||
| Wenningsted Torgard et al45b | 1982 | Lower back pain | Lumbar | NS | 6 days | Skin abscess, spondylitis, bacteremia | 10 days | Fever | S. aureus | Wedge formation of two vertebral bodies |
| McDonogh and Cranney35 | 1984 | Fractured ribs | Thoracic | Yes | 3.3 days | Epidural abscess | 2.5 days 19 days | Fever Paralysis left leg, weakness, right leg, urinary retention, sensory deficit T7 to 8 | S. aureus | Residual left-side weakness, uses walking frame, urinary retention |
| Konig et al36 | 1985 | Knee surgery | Lumbar | NS | 4 days | Paravertebral and epidural abscesses, osteomyelitis, phlegmonous duritis, myelitis | 2 weeks | Pain, lower extremity paraparesis | S. epidermidis | Nearly complete recovery |
| Sollmann et al37 | 1987 | Phantom limb pain | NS | NS | 6 weeks | Large encapsulated “spinal” abscess compressing dura at L4–L5 | 6 weeks, 5 months | Severe back pain Severe sciatica | Pseudomonas aeruginosa | Persistent pain |
| Fine et al38 | 1988 | Neuralgic pain syndrome | Thoracic | Yes | 3 days | Site infection, epidural abscess | 9 days | Fever, chills, urinary retention | No culture obtained | Sensory impairment |
| Ready and Helfer39 | 1989 | 1. Vaginal delivery | Lumbar | NS | 50 min | Meningitis | 1 day | Headache, stiff neck, fever, back pain, nuchal rigidity | Streptococcus uberis | Full recovery |
| 2. Cesarean section | NS | NS | 3 days | Cellulitis meningitis | 3.5 days 5.5 days | Fever Headache, nuchal rigidity, photophobia, hyperacusis | Enterococcus faecalis | Full recovery | ||
| Berga and Trierweiler40 | 1989 | Vaginal delivery | Lumbar | NS | NS | Meningitis | 1 day | Headache | Streptococcus sanguis | Full recovery |
| Goucke and Graziotti41 | 1990 | Back pain | Lumbar | NS | 3 epidural injections | Bacteremia, epidural abscess | 3.3 weeks after last injection | Back pain, fever, urinary retention | S. aureus | Died 7 weeks after laminectomy |
| Lynch and Zech42 | 1990 | Intra- and postoperative analgesia | Lumbar | Yes | 3 days | Spondylitis | 3 days | Fever, chills, headache, back pain | P. aeruginosa | 9-month recovery, wears lumbar brace, some lumbar pain |
| Strong43 | 1991 | 1. Herpes zosterb | Thoracic | Yes | 2.5 days 3 daysc | Epidural abscess | 4.4 weeks | Pain, headache, stiff neck, fever, right flank pain | S. aureus | Full recovery |
| 2. Reflex sympathetic dystrophy | Cervical | Yes | 5 days 5 daysc | Cellulitis Epidural abscess | 16 days 7 weeks | Cellulitis Neck pain radiating to left arm | Culture negative | Full recovery | ||
| Klygis and Reisberg44 | 1991 | Vaginal delivery | NS | NS | NS | Epidural abscess | 1.5 days | Back pain, paresthesias medial thigh and plantar surface of feet, fever | Group G streptococci | Full recovery |
| Dawson et al45 | 1991 | Postoperative analgesia | Thoracic | Yes | 4 days | Epidural abscess | 12 days 18 days | Numbness and weakness in leg, urinary incontinence Paraplegia | S. aureus | Loss of motor function, requires indwelling urinary catheter, able to take few steps with help |
| Waldmann142 | 1991 | Cervical radiculopathy | C6 | NS | NS | Epidural abscess | 72 h | Stiff neck and chills | S. aureus | Quadraparetic with partial function of upper extremities and able to walk |
| Ferguson46 | 1992 | Intra- and postoperative analgesia | Lumbar | Yes | 4 days | Cellulitis, epidural infection | 7 days | Fever, back pain | S. aureus | Not specified |
| NganKee and Jones47 | 1992 | Cesarean section | Lumbar | Yes | 50 h | Epidural abscess | 5 days | Fever, back pain, rigors, bacteremia, paresthesias, weakness of both legs | S. aureus | Full recovery after 8 weeks |
| Sowter et al48 | 1992 | Intra- and postoperative analgesia | Thoracic | Yes | 5 days | Epidural abscess | 3.6 weeks | Back pain, urinary retention, paresthesias and weakness both legs | S. aureus | Paraplegic with indwelling urethral catheter |
| Shintani et al49 | 1992 | Herpes zoster | Lumbar | NS | 3 days | Meningitis, epidural abscess | 3 days | Headache, nausea, vomiting, fever, somnolence, back pain | Methicillinresistant S. aureus | Full recovery |
| Nordstrom and Sandin50 | 1993 | Fractured ribs | Thoracic | Yes | 6 days | Epidural abscess | 19 days | Back pain, numbness both legs, fever, paresis urethral sphincter | S. aureus | Incomplete recovery of motor function 4 months after laminectomy |
| Mamourian et al70 | 1993 | PVD | L3–L4 | NS | 48 h | Epidural abscess | 72 h | Lower extremity radicular pain and weakness, urinary retention | S. aureus | Full recovery |
| Low back pain | NS | NS | Single shot | Epidural abscess | 2 weeks | Worsening pain, leg weakness, urinary retention | S. aureus | Died from ventricular tachycardia | ||
| PVD | NS | NS | Single shot | Epidural abscess | 24 h, 4 days | Fever, leg spasm | S. aureus | No neurologic deficit | ||
| Davis et al51 | 1993 | Vaginal delivery | Lumbar | NS | Less than 1 day | Meningitis | 1.7 days | Headache, vomiting, confusion, delirium, fever | Group β-hemolytic streptococci | Full recovery |
| Ania52b | 1994 | Lumbar pain | NS | NS | 8 days | Meningitis | 1 day, 3 days | Headache, chills, vomiting | S. aureus | Full recovery |
| Tabo et al71 | 1994 | Herpes zoster | L3–L4 | NS | 3 days | Epidural abscess | 4 days | Fever, fatigue, pain | S. aureus | Full recovery |
| Borum et al53 | 1995 | Vaginal delivery | Lumbar | Yes | 1 days | Epidural abscess | 4 days | Low back pain, tingling both lower extremities | S. aureus | Full recovery |
| Liu and Pope54 | 1996 | Extracorporeal shockwave lithotripsy | NS | NS | NS | Meningitis | 6 days | Weakness both lower extremities | Streptococcus pneumoniae | Full recovery |
| Dunn et al<55 | 1996 | Intra- and postoperative analgesia | NS | NS | 1 day | Epidural abscess, osteomyelitis | 1 day | Neck and back pain | S. aureus | Mild hip and loin pain 5 months after the operation |
| 14 days | Back pain, nausea, vomiting, fever | |||||||||
| Cooper and Sharpe56b | 1996 | Chronic back pain | Not specified | NS | Injection | Meningitis, cauda equina syndrome | 3 days | Increased back pain, chills, profuse sweating | S. aureus | Incontinent of stool |
| 13 days | Leg weakness, incontinent of stool | |||||||||
| Barontini et al57 | 1996 | Transurethral resection of prostate | Lumbar | NS | NS | Epidural abscess | 2 days | Fever, leg weakness | No culture obtained | Paraplegia |
| 4 days | Chills, pain, flaccid paraparesis of leg | |||||||||
| Pinczower and Gyorke15 | 1996 | Postoperative analgesia | Lumbar | NS | 4 days | L1 vertebral osteomyelitis | 3 weeks | Low back pain | P. aeruginosa | Full recovery |
| Wang et al72 | 1996 | RSD | L2–L3 and L3–L4 (total of 4 catheters during 4 weeks) | NS | 4 weeks | Small epidural abscess with meningeal irritation | ? | Nuchal rigidity, back pain, nausea, photophobia, severe headache | Not identified | Full recovery |
| Bengtsson et al17 | 1997 | 1. Analgesia after a traumatic amputation | L3–L4, T12–L1 | Yes | 1 day,c 4 days | Meningitis | 4 days | Fever, pain and erythema at 2nd insertion site, stiff neck | P. aeruginosa | Full recovery |
| 2. Analgesia for phantom pains after an amputation | Lumbar | Yes | 3 days | Soft tissue and interspinal abscess | 3 days | Fever, severe headache, erythema, S. aureus and swelling at insertion site, back pain radiating to right thigh | No culture obtained | Radicular pain in lower back | ||
| 3. Analgesia for painful foot ulcers | Lumbar tunneled catheter | Yes | 16 days | Psoas abscess at L2 to L5 tracking to L3–L4 intraspinal level | 11 days, 14 days | Fever, pain radiating from back | S. aureus | Full recovery | ||
| Sarrubbi and Vasquez58 | 1997 | 1. Analgesia for reflex sympathetic dystrophy | L1–L2 | NS | 3 days | Epidural abscess | 3 days | High fever, cloudy drainage at catheter exit site | S. aureus | Recovered to her baseline |
| 2. Surgical anesthesia and postoperative analgesia | NS | NS | 2 days | Epidural abscess and meningitis | 2 days | Bilateral leg weakness and double vision | S. aureus | Ambulated with a walker at 3 months | ||
| 5 days | Flaccid paralysis, double vision from 3rd-nerve palsy, meningism, sensory level L1 | |||||||||
| Iseki et al59 | 1998 | Analgesia for herpes zoster | 11 epidural injections then catheters at T6–T7, T8–T9, T7–T8 | NS | 4 days,c 1 day, 6 days | Epidural abscess at T6–T7 and inflammation of the perivertebral muscles at T5 to T7 | 6 days after the final catheterization | Fever, elevated white blood count and C-reactive protein | Methicillinresistant S. aureus | Full recovery |
| O’Brien and Rawluk60 | 1999 | Analgesia for low back pain | 1 epidural injection | NS | Not applicable | Epidural abscess | 3 months | Back pain, bilateral lower extremity pain | Mycobacterium fortuitum | Full recovery |
| Halkic et al61 | 2001 | Postoperative analgesia | T11–T12 | NS | 4 days | Spondylodiscitis at L5–S1 | 4 days | Lumbar pain radiating to the groin | Propionibacterium acnes | Full recovery |
| Phillips et al62 | 2002 | 1. Postoperative analgesia | Thoracic | NS | 3 days | Epidural abscess | 4 days | Fever | S. aureus | Full recovery |
| 5 days | Low backache, headache, tenderness at insertion site | |||||||||
| 2. Postoperative analgesia | Thoracic | NS | 3 days | Epidural abscess | 3 weeks | Pain at insertion site, weakness in lower extremities, urinary retention | Methicillinresistant S. aureus | Died of a pulmonary embolus and cardiac arrest | ||
| Royakkers et al63 | 2002 | 1. Postoperative analgesia | L2–L3 | Yes | 4 days | Epidural abscess | 3 days | Fever | S. aureus | Full recovery |
| 4 days | Elevated ESR, WBC, C-reactive protein | |||||||||
| 5 days | Erythema at exit site | |||||||||
| 7 days | Pus at insertion site | |||||||||
| 2. Postoperative analgesia | T7–T8 | NS | 5 days | Epidural abscess | 6 days | Erythema and pus at insertion site | S. aureus | Full recovery | ||
| 3. Postoperative analgesia | T10–T11 | NS | 3 days | Epidural abscess | 7 days | Signs of local infection, back pain, fever to 39°C | S. aureus | Full recovery | ||
| Hagiwara et al64 | 2003 | Postoperative analgesia | Low thoracic | NS | NS | Epidural abscess | 4.8 months | Fever, back pain, neck stiffness, coma, and quadriplegia | Methicillinresistant S. aureus | Nearly full recovery |
| Evans and Misra65 | 2003 | Labor analgesia | Lumbar | Yes | NS | Epidural abscess | 7 days | Back and leg pain | NS | Incomplete recovery |
| 9 days | Hot and cold flushes, flu-like illness, pain from back down both legs | |||||||||
| 11 days | Fever, dehydration, tachycardia | |||||||||
| 12 days | Unable to bear weight or pass urine, sensation decreased below knees | |||||||||
| Yue and Tan66 | 2003 | Low back pain | Caudal | NS in abstract | NS in abstract | Diskitis | 4 weeks | Low back pain, elevated serum acute-phase reactants, radiographic evidence of L4–L5 diskitis | P. aeruginosa | Full recovery |
| Hagiwara et al69 | 2003 | Colectomy | Lumbar | NS | NS | Epidural abscess | 144 days | Fever, severe back pain | Methicillinresistant S. aureus | Slight gait disturbance |
| Volk et al179 | 2005 | Hip replacement | Lumbar | Yes | 3 days | Subdural empyema and paraspinal abscess | 16 days | Fever, back pain, mild headache | NS | Full recovery |
| Aiba et al67 | 2009 | NS | NS | NS | NS | Wide epidural abscess | NS | NS | NS | NS |
| Radif and Dalsgaard68 | 2009 | NS | NS | NS | 2 days | Subcutaneous abscess and meningitis | 2 days | Pain, later fever and neck rigidity | NS | Full recovery |
| Pitkänen et al113 | 2013 | Abdominal surgery | Thoracic | NS | 9 days | Epidural abscess | NS | NS | Full recovery | |
| Herniated disk | NS | NS | Several injections | Epidural abscess | NS | NS | Full recovery | |||
| Multiple trauma | Thoracic | NS | 14 days | Epidural abscess | NS | NS | Full recovery | |||
| Chronic pain | NS | NS | NS | Meningitis | NS | NS | Full recovery | |||
| Chronic pain | NS | NS | 14 days | Sepsis | NS | NS | Full recovery |
Scott and Hibbard surveyed all obstetric units in the United Kingdom and identified one epidural abscess in approximately 506,000 epidural neural blocks. In contrast, Palot and colleagues identified three cases of meningitis in 300,000 patients who had undergone epidural blocks. Three smaller series of obstetric epidural neural blocks (some 12,000 patients) did not identify any infections. Similarly, in a recent study by the French SOS group on complications of regional anesthesia, Auroy and coworkers did not identify any infections in 29,732 epidural neural blocks given for obstetrical procedures. Together, the results of these five studies suggest that four or five serious infectious complications (ie, epidural abscesses or meningitis) occur per 1 million obstetric epidural neural blocks.
A number of studies have assessed infections associated with epidural neural blocks performed for operative procedures or for short-term pain relief. However, these studies reported fewer patients than the studies of epidural neural block for obstetric procedures. Findings from 10 studies are summarized in Table 3. Brooks and collaborators found four infections among 4832 (0.08%) patients undergoing epidural neuraxial block for surgical procedures or for labor and delivery. All four infections occurred in healthy young women who underwent cesarean sections; two infections were superficial (0.04%), and two involved the epidural space (0.04%). In contrast, Holt and colleagues reported 53 (1.8%) local infec-tions and 11 (0.4%) central nervous system infections related to approximately 3000 epidural catheters.The median duration of catheterization was 8 days for patients with local infections and 15 days for those with generalized symptoms (p = .01). Catheters removed from patients with clinical symptoms were more heavily colonized than those removed from asymptomatic patients. However, 59 of 78 catheters with positive cultures were removed because patients were symptomatic, suggesting that this observation may have been affected by ascertainment bias.
Given that the incidence of infections identified in all studies has been low, the results reported by investigators who calculated the upper boundaries of the infection risk associated with epidural neural block are particularly important because they provide a better estimate of the true risk than do studies that reported only the number of infections and the number of procedures. For example, Strafford and coworkers did not identify skin infections or epidural abscesses among 1458 pediatric patients who had epidural analgesia to control perioperative pain. These investigators calculated the incidence of clinical infection to be 0 with a 95% confidence interval from 0% to 0.03%, or three infections per 10,000 procedures. Auroy and colleagues, as noted previously, did not identify any infections among 29,732 procedures done for deliveries. They calculated 95% confidence intervals of 0/10,000 to 1/10,000 procedures. Darchy and associates evaluated 75 patients, 9 (12%; incidence density rate of 2.7/100 catheter-days) of whom acquired local infections. None of the patients acquired deep infections. Based on these data, Darchy and associates estimated the upper risk of spinal space infections to be 4.8% for catheters that remained in place for 4 days. Of note, these estimates are considerably higher than those of Strafford and coworkers and higher even than the rates found by Du Pen and collaborators among patients with epidural catheters for long-term pain control.
TABLE 3. Infections after epidural neural blocks done for surgical procedures or short-term pain relief.
| Author (Reference) | Year Published | Number of Patients | Number of Infections |
|---|---|---|---|
| Hunt et al28 | 1977 | 102 | 1 cellulitis |
| Sethna et al82 | 1992 | 1200 children | 0 |
| Darchy et al83 | 1996 | 75 | 9 local infections, 4 of which were associated with catheter infections |
| McNeeley et al84 | 1997 | 91 | 0 |
| Abel et al85 | 1998 | 4392 | 0 |
| Grass et al86 | 1998 | 5193 | 1 exit site infection |
| Kost-Byerly et al87 | 1998 | 210 children | 21/170 (12.3%) of caudal catheters, 1/40 (2.5%) lumbar catheters were associated with cellulitis |
| Phillips et al62 | 2002 | 2401 | 3 epidural infections |
| Auroy et al81 | 2002 | 5561 | 1 meningitis |
| Volk et al140 | 2009 | 5057 | 136 exit site infections |
In general, epidural catheters inserted for long-term pain control become infected more frequently than those used for short periods of time. Du Pen and associates identified 30 superficial (9.3/10,000 catheter-days), 8 deep catheter track (2.5/10,000 catheter-days), and 15 epidural space (4.6/10,000 catheter-days) infections among 350 patients who had long-term epidural catheters. Similarly, Zenz and colleagues identified two cases of meningitis among 139 patients (1.4%, or 2.1/10,000 catheter-days) treated for pain due to malignancy. Coombs reported that 10 of 92 (10.9%) cancer patients acquired local infections, and 2 (2.2%) acquired meningitis. Malignancy and reduced immunocompetence might be additional risk factors in the population with long-term catheters.
Whether newly developed transparent dressings with integrated chlorhexidine patches might be beneficial for this vulnerable population remains to be seen.
INFECTIONS ASSOCIATED WITH SUBARACHNOID block
Case reports in the literature indicated that serious infections can occur as complications of subarachnoid neural block (Table 4). Of the 471 infections reported in these case reports, 272 were meningitis, 4 were epidural abscesses, 2 were soft tissue abscesses, 2 were infections of a disk or of a disk space, 1 developed cerebral and spinal abscesses, and 1 was a case of severe necrotizing fasciitis. In the last case mentioned, the authors speculated about a contaminated reused multiuse vial of local anesthetic as the cause. The median time to onset of signs or symptoms of infection was 1 day (range 1 hour to 2 months) for all infections and 18 hours (range 1 hour to 10 days for meningitis). Streptococcal species caused 24 of the 37 infections from which bacterial pathogens were identified; S. aureus caused 2 infections; Pseudomonas spp. caused 4; and an extended spectrum betalactamase Serratia marcescens caused 1. Compared with infections after epidural neural block, infections associated with subarachnoid neural block were more likely to be caused by streptococci, and patients were more likely to recover fully. Table 5 reviews data from 10 studies or reviews that, if taken together, suggest that the rate of infection was approximately 3.5 per 100,000 sub-arachnoid neural blocks.
INFECTIONS ASSOCIATED WITH COMBINED EPIDURAL AND SUBARACHNOID block
At present, there are few reports in the literature about infectious complications as a result of using combined epidural-subarachnoid (CSE) neural block. In 11 case reports of infections with a total number of 12 patients after combined procedures (Table 6), the median time to onset of signs or symptoms of infection was 21 hours (range 8 hours to 9 days) for all infections and 18 hours (range 8 hours to 3 days) for meningitis. Signs or symptoms of epidural abscesses were first noted 1–9 days after the procedures. Streptococcal species caused three of six cases of meningitis, and S. aureus caused all three epidural abscesses. Ten of twelve patients recovered fully. Cascio and Heath assessed rates of infection associated with combined procedures and identified one case of meningitis after about 700 (≈0.1%) CSE neural blocks.
INFECTIONS ASSOCIATED WITH PERIPHERAL NERVE BLOCKS
Continuous regional anesthetic techniques utilizing peripheral nerve blocks have become more popular in recent years for postoperative pain management, especially for orthopedic procedures. Only a few studies have addressed infectious complications related to these procedures. The study by Auroy and coworkers of French anesthesiologists did not identify any infections after 43,946 peripheral blocks. Bergman and colleagues identified 1 patient among 368 patients (405 axillary catheters) who had a local S. aureus skin infection in the axilla after 48 hours of axillary analgesia. The patient recovered fully with antibiotic treatment. Meier and colleagues reported eight superficial skin infections among 91 patients who had continuous interscalene catheters for an average of 5 days. Nseir described a case of fatal streptococcal necrotizing fasciitis following axillary brachial plexus block. Adam reported a psoas abscess complicating a femoral nerve block catheter.
Cuvillion and coworkers obtained cultures of 208 femoral catheters when they were removed after 48 hours. Of the catheters, 54% were colonized with potentially pathogenic bacteria (71% Staphylococcus epidermidis, 10% Enterococcus spp., and 4% Klebsiella spp.). These investigators also reported three episodes of transient bacteremia, but they did not identify any abscesses or episodes of clinical sepsis. None of the groups provided information about the aseptic techniques used for catheter insertion.
Compère reported a single infection in 400 continuous popliteal sciatic nerve blocks (0.25%), while Volk and coworkers from the German regional anesthesia network reported in 2009 a 1.3% incidence of infectious complications for peripheral blocks in 3724 procedures compared to a higher rate for neuraxial techniques (2.7% in 5057 procedures).
Between 2002 and 2009, Reisig and coworkers collected data on 10,549 peripheral catheter procedures in an observations study that included the implementation of a comprehensive infection control bundle. While the definitions of inflammation and infection used in this study remain somewhat vague, they could show a rate of 4.2% for inflammation and 3.2% for infections in 3491 procedures before the intervention and a reduction to 2.6% for inflammation and 0.9% for infections in 7053 procedures after the interventions.
Other reports included cases of osteomyelitis following digital blocks and hematoma block for fracture repair, as well as orbital cellulites from sub-Tenon anesthesia,mediastinitis following continuous interscalene block, Aspergillus caldi-oustus infection after unspecified lower back nerve block, and two cases with sepsis after femoral nerve catheters.
All these reports emphasize the importance of maintaining strict asepsis when performing continuing peripheral nerve blocks.
TABLE 4. Infections associated with subarachnoid neural block.
| Author (Reference) | Year Indication | Indication | Type of Infection | Incubation Period | Signs and Symptoms | Microorganism | Outcome | Comments |
|---|---|---|---|---|---|---|---|---|
| Corbett and Rosenstein96 | 1971 | 1. Vaginal delivery | Meningitis | 36 h | Fever, headache, stiff neck | Pseudomonas aeruginosa | Full recovery | Three patients infected when a physician rinsed the spinal needle stylet in saline used for consecutive deliveries |
| 2. Vaginal delivery | Meningitis | 3 days | Fever, headache, stiff neck, neck pain, nuchal rigidity | P. aeruginosa | Full recovery | |||
| 3. Vaginal delivery | Meningitis | 4 days | Fever, headache, nausea | P. aeruginosa | Full recovery | |||
| Siegel et al97 | 1974 | Vaginal delivery | Left subgluteal abscess | 4 h | Buttock pain radiating to thigh | Mimeae | Full recovery | |
| 14 days | Severe pain sacroiliac joint | |||||||
| Loarie and Fairley | 1978 | Debride necrotic heel ulcers | Epidural abscess | 2 days | Fever, back pain, urinary retention | Staphylococcus epidermidis, Bacteroides | Full recovery | Insulin-dependent diabetic |
| 15 days | Bilateral lower extremity weakness, absent anal sphincter tone | |||||||
| Berman and Eisele14 | 1978 | Transurethral evacuation of clot from bladder | Meningitis | 1 h | Shaking chill, fever, back pain, headache, confusion | Enterococcus | Not specified | |
| Beaudoin and Klein98 | 1984 | Debride and drain infected foot | Epidural abscess | 4 days after last subarachnoid neural block | Back pain, pain radiating to upper thighs | Pseudomonas spp. | Full recovery | 35-year-old insulindependent diabetic, received 5 subarachnoid neural blocks in 10 days |
| Abdel-Magid and Kotb99 | 1990 | Hemorrhoidectomy | Epidural abscess | 15 days | Back pain, leg weakness, urinary retention, fever, bilateral absent ankle reflexes | Proteus spp. | Full recovery | |
| Roberts and Petts100 | 1990 | Remove retained placenta | Meningitis | 18 h | Headache, photophobia, fever, chills, positive Kernig sign, quadriceps weakness | Culture negative | Full recovery | Antibiotics started before the lumbar puncture |
| Lee and Parry101 | 1991 | Cesarean section | Meningitis | 16 h | Severe headache | |||
| 22 h | Nausea, photophobia, decreasing mental status, fever, nuchal rigidity, positive Kernig sign | |||||||
| Blackmore et al102 | 1993 | Herniorrhaphy | Meningitis and bacteremia | 16 h | Fever, vomiting, obtundation | Streptococcus mitis | Full recovery | |
| Ezri et al103 | 1994 | Hemorrhoidectomy | Meningitis | 10 days | Fever | Escherichia coli | ||
| 25 days | Malaise, headache, photophobia, dizziness, fever | Full recovery | ||||||
| Mahendru et al104 | 1994 | Foot amputation | Epidural abscess | 3 weeks | Back pain, bilateral lower extremity paresis and weakness | No culture obtained | Died from esophageal carcinoma | Insulin-dependent diabetic |
| Gebhard and Brugman105 | 1994 | Knee arthroscopy | Diskitis | 2 months | Back and thigh pain, elevated sedimentation rate | Propionibacterium acnes | Full recovery | |
| Newton et al106 | 1994 | Vaginal delivery | Meningitis | 12 h | Headache, photophobia, declining mental status, fever | Streptococcus salivarius | Full recovery | |
| Schneeberger et al9 | 1996 | 1. Knee arthroscopy | Meningitis | 12 h | Fever, meningeal signs | Streptococcus sanguis | Full recovery | |
| 2. Knee arthroscopy | Meningitis | 12 h | Headache | S. mitis | Full recovery | |||
| 2 days | Fever, meningeal signs | |||||||
| 3. Varicose vein stripping | Meningitis | 24 h | Headache, fever, impaired consciousness, meningeal signs | S. salivarius | Full recovery | |||
| 4. Varicose vein stripping | Meningitis | 12 h | Headache, fever | Streptococcus cremoris | Communicating hydrocephalus | Hydrocephalus may have been preexisting | ||
| Horlocker et al109 | 1997 | 1. Urologic procedure | Disk space infection | 1 day | Low back pain | Staphylococcus aureus | Full recovery | |
| 4 months | Incapacitating low back pain | |||||||
| 2. Examination under anesthesia | Paraspinal abscess | 1 day | Low back pain | S. aureus | Full recovery | |||
| 11 days | Fever | |||||||
| Kaiser et al107 | 1997 | Hysterectomy | Meningitis | 12 h | High fever, severe headache, lumbar pain, lethargy, Glasgow score of 12, nuchal rigidity, positive Kernig and Brudzinski signs | S. salivarius | Full recovery | |
| Laurila et al73 | 1998 | Arthroscopy | Meningitis | 16 h | Headache, nausea, vomiting | S. salivarius | Full recovery | Anesthesiologist wore mask and gloves and used chlorhexidinealcohol solution for skin preparation |
| Fernandez et al108 | 1999 | Arthroscopic meniscectomy | Meningitis | 18 h | Severe headache, nausea, vomiting, high fever, nuchal rigidity | S. mitis | Full recovery | |
| Yaniv and Potasman95 | 2000 | Extracorporeal shock wave lithotripsy for ureterolithiasis | Meningitis | 12 h | Fever, severe headache, meningeal signs, elevated white blood cell count | S. salivarius | Minor sequelae, mild paresthesia of right thigh | Anesthesiologist wore gown, sterile gloves, face mask |
| Trautmann et al8 | 2002 | Arthroscopic knee repair | Meningitis | 1 day | Fever, nausea, stiff neck | S. salivarius | Full recovery | Both patients underwent their operations the same day |
| Arthroscopic knee repair | Meningitis | 1 day | Headache, nausea, stiff neck | S. salivarius | Full recovery | |||
| Rubin et al10 | 2007 | 6 surgical cases | Meningitis | NS | Fever, stiff neck | S. salivarius | Full recovery | Single anesthesiologist with possible violation of aseptic technique |
| Cervero111 | 2009 | Surgery | Meningitis | NS | NS | S. salivarius | NS | |
| CDC11 | 2010 | Intrapartum (6 cases) | Meningitis | NS | NS | S. salivarius | Full recovery | Not wearing a mask in 5 cases |
| Hadzic et al110 | 2012 | Orthopedic surgery | Meningitis | 1 day | Headache, fever | ESBL Serratia marcescens | Full recovery | Multiresistant organisms need to be considered for empiric treatment depending on local endemic situation |
| Kundra et al112 | 2012 | Cesarean delivery | Necrotizing fasciitis | 5 days | Skin necrosis from puncture site to the gluteal region | NS | Full recovery | Reused contaminated multidose vial as likely cause |
| Pitkänen et al113 | 2013 | Knee arthroscopy | Cerebral and spinal abscesses | 2 months | Headache, stiff neck | NS | Death | |
| Knee surgery | Meningitis | NS | NS | NS | Full recovery | |||
| Phimosis | Meningitis | NS | NS | NS | Full recovery | |||
| Knee arthroscopy | Meningitis | NS | NS | NS | Full recovery | |||
| Prostate hyperplasia | Meningitis | NS | NS | NS | Full recovery | |||
| Knee arthroscopy | Meningitis | NS | NS | NS | Full recovery |
TABLE 5. Frequency of meningitis after subarachnoid neural block.
| Author (Reference) | Year | Number of Patients | Number of Infections | Rate of Meningitis |
|---|---|---|---|---|
| Evans116 | 1945 | 2500 | 0 | 0 |
| Scarborough117 | 1958 | 5000 | 0 | 0 |
| Dripps and Vandam118 | 1954 | 8460 | 0 | 0 |
| Moore and Bridenbaugh119 | 1966 | 11,574 | 0 | 0 |
| Lund and Cwik120 | 1968 | >21,000 | 0 | 0 |
| Sadove et al121 | 1961 | >20,000 | 3 | ≈15/100,000 |
| Arner122 | 1952 | 21,230 | 1 | 4.7/100,000 |
| Horlocker et al109 | 1997 | 4217 | 0 | 0 |
| Auroy et al81 | 2002 | 5640 obstetrical | 0 | 0 |
| Auroy et al81 | 2002 | 35,439 nonobstetrical | 1 | 2.8/100,000 |
| Pugely et al123 | 2013 | 6030 Total knee replacements | ? | 0 |
| Total | >141,090 | 5 | ≈3.5/100,000 | |
PREVENTION OF INFECTIONS ASSOCIATED WITH REGIONAL ANESTHESIA
Anesthesiologists disagree about the necessity of certain infection control precautions. For example, several surveys indicated that only 50%–66% of anesthesia staff wore masks when performing epidural and subarachnoid neural blocks.
NYSORA Tips
- Wearing a mask during insertion of indwelling neuraxial or peripheral nerve catheters is suggested.
- Sterile gown should be warn during insertion of epidural or nerve block catheters.
- Sterile ultrasound transducer cover should be routinely used with ultrasound-guided procedures.
- Surveillance for catheter site infections is one of the most effective methods for reducing the incidence and consequence of indwelling catheter–related infections.
The review of studies on infections associated with epidural anesthesia indicated that there is no consensus regarding patient risk factors for infectious complications of epidural neural block. Few studies assess risk factors for infection associated with epidural or subarachnoid neural blocks, possibly in part because these infections are uncommon. In fact, only one case-control study was performed to evaluate risk factors for infections associated with epidural neural block. Dawson and colleagues evaluated epidural neural blocks performed for postoperative pain relief and found that procedures done between April and August had a sixfold higher risk than those done during other months (95% CI 1.28–28.12, p = .009). The risk of infection was lower if a bag rather than a syringe was used to administer the anesthetic agent (odds ratio 0.17, 95% CI 0.02–1.34, p = .05). Of the two risk factors identified by this study, only the latter, use of syringes, could be addressed by practice changes.
Assuming that the respiratory tract of anesthesia personnel could be a source of infection, Philips and associates conducted a simulation to assess the efficacy of masks. They seated anesthesia staff with and without masks in a room with controlled environment and asked them to speak in front of blood agar plates placed 30 cm away. The number of bacteria on the plates was significantly lower when masks were worn. However, the clinical significance of this finding is unknown.
Chlorhexidine has been shown to reduce the risk of catheter-associated bloodstream infections significantly compared with povidone-iodine. Several investigators have tried to determine whether a particular disinfectant provides more effective skin antisepsis before epidural neural blocks than do other agents. However, none of the studies was large enough to assess rates of infection; instead, the outcomes evaluated were catheter or skin colonization.
Kasuda and colleagues randomly assigned 70 patients to have their skin prepared with either a 0.5% alcoholic solution of chlorhexidine or 10% povidone-iodine. After a median of 49 ± 7 hours, the investigators removed the catheters and obtained cultures of the insertion sites and catheter tips. There was no difference in rates of positive cultures.
Kinirons and associates (the only investigators who reported a power calculation) obtained cultures from catheters removed from 96 children who had epidural catheters longer than 24 hours. The colonization rate was lower for catheters removed from children whose skin was prepared with a 0.5% alcoholic solution of chlorhexidine (1/52 catheters, 0.9/100 catheter-days) than for those removed from children whose skin was prepared with povidone-iodine (5/44 catheters, 5.6/100 catheter-days) (relative risk 0.2, 95% CI 0.1–1.0).
TABLE 6. Infections associated with combined subarachnoid and epidural neural block.
| Author (Reference) | Year | Indication | Type of Infection | Time of Symptom Onset | Signs and Symptoms | Microorganism | Outcome | Comments |
|---|---|---|---|---|---|---|---|---|
| Cascio and Heath124 | 1995 | Vaginal delivery | Meningitis | 16 h after delivery, ≈ 20 h after insertion | Fever, headache, chills, photophobia, mild nuchal rigidity | Streptococcus salivarius | Full recovery | Anesthesiologist wore mask, cap, and sterile gloves and used povidone-iodine spray for skin antisepsis |
| Harding et al125 | 1994 | 1. Vaginal delivery | Aseptic meningitis | 21 h after the injection | Severe headache, faint feeling, shortness of breath, urinary retention, aphasia, tingling right side of face, neck stiffness, positive Kernig sign, low-grade temperature | No growth | Full recovery | Anesthesiologist scrubbed, wore sterile gown and gloves, and used alcoholic chlorhexidine for skin antisepsis |
| 2. Vaginal delivery converted to emergency cesarean section | Meningitis | 3 days after the operation | Headache, fever, vomiting, severe stiff neck, elevated white blood cell count, hypotension, bradycardia | Staphylococcus epidermidis | Full recovery | Alcoholic chlorhexidine used for skin antisepsis | ||
| Stallard and Barry126 | 1994 | Analgesia during labor, subsequent cesarean section | Meningitis | 18 h after the operation | Acute confusion, fever, aphasia, ignored left side, elevated white blood cell count | No growth | Full recovery | Did three procedures to achieve adequate analgesia; anesthesiologist used alcoholic chlorhexidine for skin antisepsis and wore mask, gown, and gloves |
| Aldebert and Sleth127 | 1996 | Vaginal delivery | Meningitis | 8 h after puncture | Headache, nausea, fever, agitation, nuchal rigidity, positive Babinski sign | Nonhemolytic streptococcus | Full recovery | Anesthesiologist wore mask, gown, cap, and sterile gloves |
| Dysart and Balakrishnan128 | 1997 | Cesarean section | Epidural abscess | 9 days after the operation | Backache, fever, foot drop, weakness of ankle eversion and inversion, absent ankle jerk reflex, decreased pinprick sensation from L5 to perianal region, elevated erythrocyte sedimentation rate | Staphylococcus aureus | Nearly full recovery; patient had residual numbness in L5 distribution | Anesthesiologist wore a mask, gown, and gloves and used chlorhexidine for skin antisepsis |
| Schroter et al129 | 1997 | Anesthesia for vascular surgery | Epidural abscess | 1 day after procedure | Back pain, fever, slight nuchal rigidity, erythema and induration at puncture site and purulent drainage from puncture site, elevated white blood cell count | S. aureus | Full recovery | Anesthesiologist wore a mask, surgical hood, sterile gloves, and gown and used povidone-iodine for skin antisepsis |
| Bouhemad et al130 | 1998 | Cesarean section | Epidural abscess | 14 h after delivery | Fever, severe headache, photophobia, drowsiness, stiff neck, | S. salivarius | Full recovery | Anesthesiologist wore gown, gloves, face mask, and cap and used tincture of iodine for skin antisepsis |
| Rathmell et al114 | 2000 | Labor analgesia in patient with multiple trauma | Epidural abscess | 7 days after catheter placement | Back pain, purulent discharge from insertion site | S. aureus | Full recovery | |
| Phillips et al62 | 2002 | Surgical anesthesia and postoperative analgesia | Epidural abscess Ll–L2 | Day 6 | Discomfort at the epidural site and severe radicular pain in L2 dermatome, erythema and swelling at site, decreased strength, light touch, and pinprick, and loss of ankle jerk reflex | S. aureus | Discharged from hospital 3 months after first operation | Anesthesiologist wore a cap, gown, and sterile gloves and used 10% povidone-iodine for skin antisepsis |
| Sandkovsky et al131 | 2009 | Delivery | Meningitis | NS | NS | Streptococcus spp. | NS | |
| Pitkänen et al113 | 2013 | Total hip arthroplasty | Epidural abscess | NS | NS | NS | Full recovery |
Sato and coworkers enrolled 60 patients who were undergoing back operations under general anesthesia. After preparing the site with either 0.5% alcoholic chlorhexidine or 10% povidone-iodine, the investigators obtained skin biopsies. Cultures from skin prepared with the alcoholic chlorhexidine were less likely to be positive (5.7%) than were cultures from skin prepared with povidone–iodine (32.4%; p < .01). However, microscopy was as likely to identify bacteria in the hair follicles of skin prepared with the alcoholic solution of chlorhexidine (14.3%) as skin prepared with povidone-iodine (11.8%).
This has led to the recommendation to use alcoholic chlorhexidine for skin preparation despite some concerns about potential neurotoxicity. The latter might be the reason American Society of Anesthesiologists (ASA) members were equivocal on the issue during the consensus process, while external experts were in favor of the recommendation.
Sviggum et al published the experiences from the Mayo Clinic analyzing almost 12,000 spinal anesthetics between 2006 and 2010 that used alcoholic chlorhexidine. They did not observe any change in neurological complications, considering the practice to be safe. Unfortunately, no data about infectious complications were reported.
The safety of alcoholic chlorhexidine was underlined in an experimental study by Doan and coworkers. They found damage to neuronal cell cultures with chlorhexidine as well as with 10% iodine they could also show that a relevant toxic concentration of skin disinfectants cannot be reached if the puncture is performed through dry skin. Therefore, allowing the skin to completely dry once disinfected before performing the block is more important than the choice of the solution in order to prevent any neurotoxic effect.
Malhotra et al demonstrated in a study of 309 healthy volunteers that single application of 0.5% chlorhexidine gluconate in 70% ethanol was as effective as two applications.The fact that infections rarely complicate neuraxial blocks suggests that the infection control practices used for these procedures are usually adequate. Given the very low rates of infection associated with epidural and subarachnoid neural block, it will be difficult to prove that additional infection control practices such as wearing masks and using full barrier precautions (ie, the anesthesiologist wears a cap, mask, sterile gloves, and sterile gown and uses a large drape to cover the patient) reduce the risk of infection. However, bacteria that colonize the skin, respiratory tract, or water caused most reported infections after epidural and subarachnoid neural blocks. Masks have been shown to decrease spread of organisms when anesthesiologists are talking. Thus, a mask would allow the anesthesiologist to talk to the patient while doing the procedure and could decrease the risk of contaminating the insertion site with oral or respiratory flora. This has also been incorporated in the ASA “Practice Advisory for the Prevention, Diagnosis, and Management of Infectious Complications Asso-ciated With Neuraxial Techniques.”
Furthermore, epidural and subarachnoid neural blocks are at least as invasive as placing central venous catheters, and the consequences of subsequent infections are at least as bad as those for catheter-associated bloodstream infections. Because the use of full barrier precautions reduces the incidence of catheter-related bloodstream infections, aseptic measures similar to those used for placing central venous catheters should be used during the placement of catheters that will remain in place for several days or longer. While the ASA practice advisory still uses the term hand washing before putting on sterile gown and gloves, hand disinfection with an alcoholic hand rub (with 70% alcohol) is the internationally preferred standard.
Anesthesia personnel should observe their patients closely for signs and symptoms of infection so that infections can be diagnosed and treated immediately. Pegues and coworkers reviewed medical records from 1980 to 1992 of patients who had short-term epidural catheters to identify those who acquired infections. They followed patients prospectively from January 1993 until June 1993.170 In 1990, they introduced a standardized procedure for inspecting temporary epidural catheters. During the entire 12.5-year period, the investigators identified seven infections, all of which occurred after catheters were inspected routinely. The increased incidence of infection could have resulted from ascer-tainment or misclassification bias associated with the retrospective review or from increased use of epidural catheters for pain management during the later time period. On the other hand, it could indicate that infections were not diagnosed when catheters were not inspected routinely for signs of infection.
Because it may be difficult to draw up opioids in a sterile manner from ampoules, some have suggested that these drugs be drawn through a filter into a syringe, which is then double wrapped and sterilized in ethylene oxide. However, the benefit of such extreme precautions is highly hypothetical.Brooks and coworkers were among the first to implement and report on structured infection control measures for continuous neuraxial blocks in their hospital. In 2008, we reviewed the literature and compared the infection control recommendations of the ASRA and the German Society of Anesthesiology and Intensive Care (DGAI) and noticed some discrepancies, especially regarding the use of masks and gowns or filters. In 2010, new guidelines by the ASA were developed in a consensus process among ASA members and external experts to clarify some of the issues. However, the evidence supporting many of the recommendations remains sparse, and extrapolation from other areas of practical implementation of infection control is needed.
The ASA “Practice Advisory for the Prevention, Diagnosis, and Management of Infectious Complications Associated With Neuraxial Techniques” has published the following guide-lines for the placement of neuraxial blocks:
- Before performing neuraxial techniques, a history and physical examination relevant to the procedure and review of relevant laboratory studies should be conducted to identify patients who may be at risk of infectious complications. Consider alternatives to neuraxial techniques for patients at high risk.
- When neuraxial techniques are indicated in a known or suspected bacteremic patient, consider administering preprocedure antibiotic therapy.
- Selection of neuraxial technique should be determined on a case-by-case basis, including consideration of the evolving medical status of the patient.
- Lumbar puncture should be avoided in the patient with a known epidural abscess.
- Aseptic techniques should always be used during the preparation of equipment (eg, ultrasound) and the placement of neuraxial needles and catheters, including the following:
- Removal of jewelry (eg, rings and watches); hand washing; and wearing of caps, masks (covering both mouth and nose and consider changing before each new case), and sterile gloves
- Use of individual packets of antiseptics for skin preparation
- Use of chlorhexidine (preferably with alcohol) for skin preparation, allowing for adequate drying time
- Sterile draping of the patient.
- Use of sterile occlusive dressings at the catheter insertion site.
- Bacterial filters may be considered during extended continuous epidural infusion.
- Limit the disconnection and reconnection of neuraxial delivery systems to minimize the risk of infectious complications.
- Consider removing unwitnessed accidentally disconnected catheters.Catheters should not remain in situ longer than clinically necessary.The following recommendations are given for the diagnosis and management of infectious complications after neuraxial block:
- Daily evaluation of patients with indwelling catheters for early signs and symptoms (eg, fever, backache, headache, erythema, and tenderness at the insertion site) of infectious complications should be performed throughout the patients’ stay in the facility.
- To minimize the impact of an infectious complication, promptly attend to signs or symptoms.
- If an infection is suspected:
- Remove an in situ catheter and consider culturing the catheter tip.
- Order appropriate blood tests.
- Obtain appropriate cultures.
- If an abscess is suspected or neurologic dysfunction is present, imaging studies should be performed, and consultation with other appropriate specialties should be promptly obtained.
- Appropriate antibiotic therapy should always be administered at the earliest sign or symptom of a serious neuraxial infection.
- Consultation with a physician with expertise in the diagnosis and treatment of infectious diseases should be considered.
TABLE 7. Summary of recommendations for infection control practice.
| SingleShot PNB | Continuous Catheter PNB | Single-Shot Neuraxial Block | Continuous Neuraxial Catheter | Long-Term Implanted Device/ Catheter (eg, Intrathecal Pump) |
|
|---|---|---|---|---|---|
| 2% chlorhexidine in 70% alcohol skin prepa | + | + | + | + | + |
| Small sterile drape | (+) | + | |||
| Large sterile drape | + | + | + | + | |
| Sterile gloves | + | + | + | + | + |
| Sterile gown | + (especially for stimulating catheters) | (+) | + | ||
| Mask | + | + | + | + | |
| Hair cover | + | + | + | + | |
| Prophylactic antibiotics | - | - | - | - | + single perioperative dose |
| Filter on injection/infusion system | - | (+) | - | (+) | NA |
| OR or special procedure room | + | ||||
| Tunneling of catheter | + (to prevent dislocation) | + if used for more than 3 days | |||
| Preparation of injection/ infusion solution under sterile conditions (pharmacy) | (+) for continuous infusion | (+) for continuous infusion |
aAlternatively, 10% povidone-iodine or 80% alcohol or a mixture of 70%–80% alcohol with povidone-iodine for at least 3 minutes. Choice of agent also depends on type of block (eg, eye blocks, etc.).
However, guidelines and standard operating procedures alone are not enough to ensure proper aseptic technique. Friedman and coworkers showed in a videotape analysis of 35 epidural placements by second-year residents a significant increase in manual skills with growing experience, but there was no increase in aseptic technique. This highlights the need for a special focus on aseptic technique in residency and during infection control audits of anesthesia providers.
PERIPHERAL BLOCKS AND PERIPHERAL CONTINUOUS CATHETERS
Recent studies indicated that infection control protocols similar to the recommendations for neuraxial block can reduce the incidence of infectious complications associated with placement of continuous peripheral nerve catheters. Unfortunately, the effectiveness of each step is hard to assess, a problem familiar from all the other recommended approaches in infection con-trol, such as the ones for prevention of central line–associated bloodstream infections or ventilator-associated pneumonia.
With the increasing use of real-time ultrasound, the correct handling of the ultrasound probe becomes an additional concern. To maintain the aseptic field, the cable and the probe should be covered with a sterile sheath to avoid contamination in the case of needle contact. Sterile contact gel or sterile saline should be used within the sheath. Puncture aids fixating the needle to the probe must be sterile. After the procedure, ultrasound probes need to be cleaned removing any residual gel and disinfected with an appropriate disinfectant that cannot damage the probe. Alternative techniques using ultraviolet light to disinfect ultrasound probes are under investigation.
SUMMARY
Although rare, infectious complications from regional anesthe-sia and analgesia do occur and can be serious. Recent guidelines offer practice recommendations especially for neuraxial blocks. Table 7 summarizes the key recommendations for decreas-ing the risk of infections related to regional anesthesia proce-dures. Surveillance systems should be implemented as part of national quality assurance programs to allow benchmarking and process optimization as well as providing data from large population databases, which would be beneficial in addressing some of the unanswered questions about infections after regional anesthesia procedures.
Clinical updates
Le Couteur et al. (Anesthesiology, 2025) systematically reviewed eight major SSI prevention guidelines (WHO, CDC, NICE, ACS/SIS, SHEA/IDSA/APIC, ACOG, APSIC, Spanish Association of Surgery) and found broad agreement that maintaining intraoperative homeostasis—glycemic control, oxygenation, normothermia, and normovolemia—is central to SSI reduction, but with substantial heterogeneity in specific targets and cited evidence. Glycemic targets ranged from ≤150 mg/dL (WHO, ACS/SIS) to <200 mg/dL (CDC/ACOG), and recommendations differed on insulin use in nondiabetics, underscoring inconsistent interpretation across 24 RCTs and highlighting the need for high-quality adaptive platform trials to determine optimal intraoperative targets.
- Read more about the study HERE.
Provenzano et al. (Regional Anesthesia & Pain Medicine, 2025) present ASRA Pain Medicine consensus infection-control guidelines for peripheral nerve blocks, neuraxial techniques, and implantable pain therapies, using a modified USPSTF grading framework and a Delphi consensus. They emphasize that Staphylococcus aureus is the leading pathogen in implantable device infections, that S. aureus colonization increases SSI risk, and that infections account for the most common damaging events in chronic pain implants—supporting graded recommendations for preoperative risk stratification, strict sterile technique, procedural setting considerations, and early recognition and management pathways.
Selvamani et al. (Regional Anesthesia & Pain Medicine, 2024) provide pooled contemporary risk estimates of infectious complications following regional anesthesia, reporting an overall infection rate of 9 per 100,000 after central neuraxial blocks (CNB) and CNS infections of 2 per 100,000 (1 per 100,000 after spinal anesthesia), with even lower rates in obstetric populations. In contrast, peripheral nerve block catheters had a substantially higher pooled infection rate of 1.8% (95% CI 1.2–2.5%), reinforcing that while neuraxial infections are exceedingly rare, catheter-based peripheral techniques warrant heightened infection surveillance and standardized reporting practices.
- Read more about the study HERE.
Clinical Update – Infections from Non-Sterile Ultrasound Gel (NYSORA/CDC, 2025):
A May 13, 2025 CDC nationwide health alert identified over 40 bloodstream infections caused by Paraburkholderia fungorum genetically linked to contaminated non-sterile, multi-use ultrasound gel (including MediChoice® and ClearImage® lots), used in percutaneous procedures such as ultrasound-guided nerve blocks and vascular access.
Key clinical implications:
- Use only single-use, sterile ultrasound gel labeled “sterile” for any procedure that breaches skin integrity (e.g., nerve blocks, IV/arterial access, biopsies). Gel labeled merely “bacteriostatic” or with preservatives should be considered non-sterile and not used for invasive procedures.
- Strict infection control practices are essential: sterile probe covers validated for percutaneous use should be applied, and transparent dressings (e.g., Tegaderm®) are not approved substitutes.
- Ongoing risk awareness: Prior outbreaks from non-sterile gel have been reported (e.g., Burkholderia cepacia complex infections), underscoring persistent infection risks when non-sterile gel contacts punctured skin.
Bottom line: Ultrasound-guided invasive procedures must incorporate sterile technique—including both sterile gel and appropriate probe barriers—to minimize healthcare-associated infection risk.
- Read more HERE.