Learning objectives
- Describe acromegaly
- Recognize signs and symptoms of acromegaly
- Anesthetic management of a patient with acromegaly
Definition and mechanisms
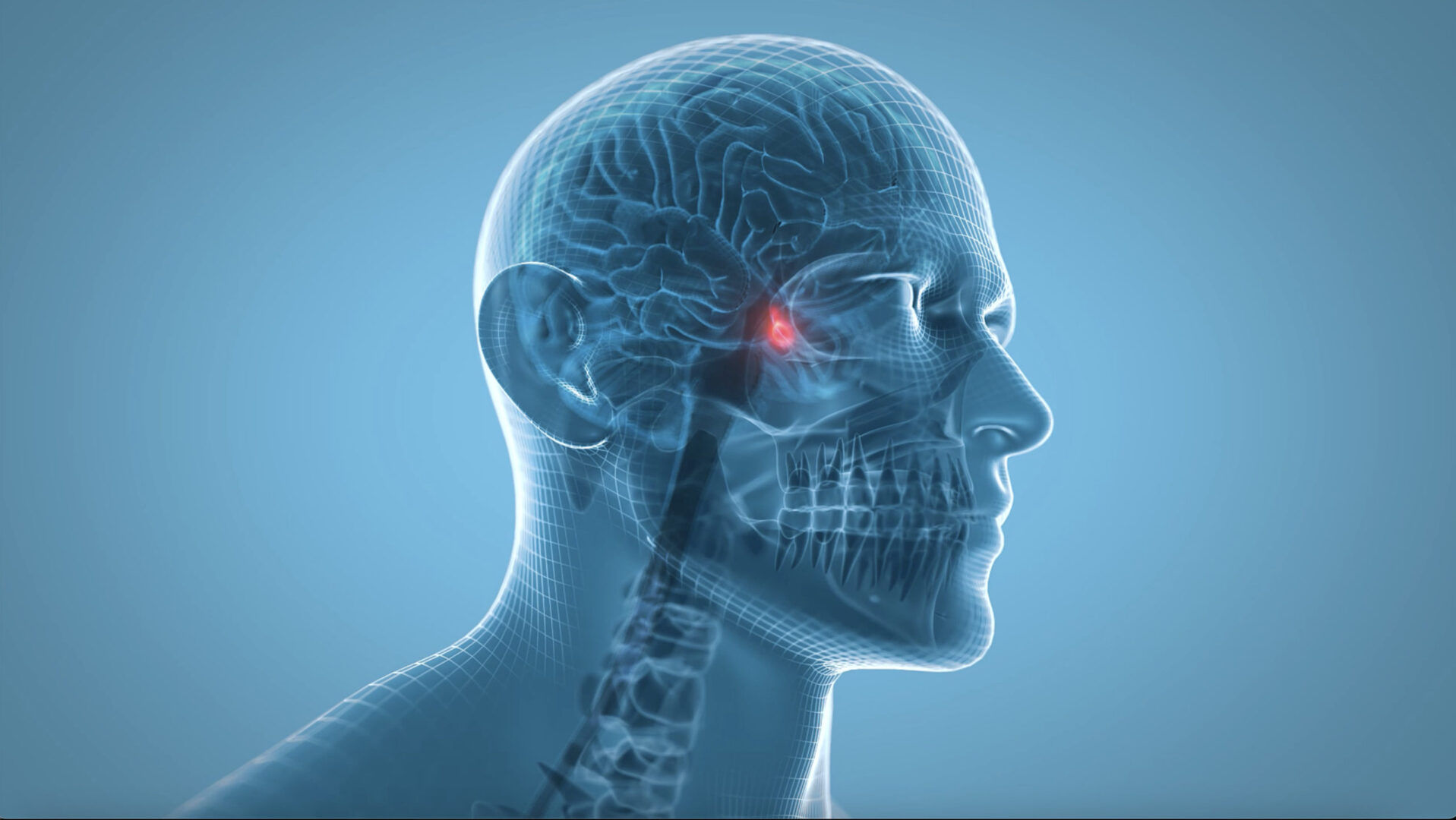
- Acromegaly is a chronic, progressive, hormone hypersecretion syndrome caused by an excess of growth hormone (GH) after the growth plates have closed (i.e., puberty)
- The hypersecretion of GH is the result of oversecretion of growth hormone-releasing hormone (GHRH) from the hypothalamus or oversecretion of the hormone itself from a pituitary adenoma
Signs and symptoms
| Affected area | Signs and symptoms |
|---|---|
| Face | Increase in size of skull and supraorbital ridges; enlarged lower jaw; increase in spacing between teeth/malocclusion |
| Hands and feet | Spade-shaped; carpal tunnel syndrome |
| Mouth/tongue | Macroglossia; thickened pharyngeal and laryngeal soft tissues; thickened vocal cords; reduction in the size of the laryngeal aperture; obstructive sleep apnea |
| Soft tissue | Thick skin; doughlike feel to palm |
| Skeleton | Vertebral enlargement; osteoporosis; kyphosis |
| Cardiovascular | Hypertension; cardiomegaly; impaired left ventricular function |
| Endocrine | Impaired glucose tolerance; diabetes |
| Other | Arthropathy; proximal myopathy |
Complications
- Diabetes mellitus type 2
- Hypertension
- Hypercholesterolemia
- Cardiomyopathy
- Pulmonary dysfunction
- Obstructive sleep apnea
- Osteoarthritis
- Goiter (enlargement of the thyroid gland)
- Colon polyps
Treatment
- Surgery: Preferred treatment; to remove the pituitary tumor
- Drugs:
- Somatostatin analogs: Drugs that reduce GH production
- Dopamine agonists: Drugs to lower hormone levels
- GH receptor antagonists: Drugs to block the action of GH
- Radiation therapy: Both used alone or in combination with surgery or drugs
Management
Four grades of airway involvement have been described in acromegaly:
| Grade | Airway involvement |
|---|---|
| 1 | No significant involvement |
| 2 | Nasal and pharyngeal mucosa hypertrophy but normal cords and glottis |
| 3 | Glottic involvement including glottic stenosis or vocal cord paresis |
| 4 | Combination of grades 2 and 3: Glottic and soft tissue abnormalities |
- Ventilation with a bag and mask is straightforward in acromegalic patients but an oral airway may be required
- Laryngoscopy and tracheal intubation prove more difficulty due to a combination of macrognathia, macroglossia, and expansion of the upper airway soft tissues
- Tracheostomy is recommended for grades 3 and 4, however, fiberoptic laryngoscopy is a safe alternative
- Tracheal intubation is feasible with standard techniques (i.e., external laryngeal pressure and the use of a gum elastic bougie or airway exchange catheter)
- Awake fiberoptic intubation is the technique of choice in case of anticipated difficult intubation in these patients
- Preoperative transthoracic echocardiography is useful to assess left ventricular size and performance, and to estimate pulmonary pressures due to associated cardiopulmonary complications
Keep in mind
- About one-quarter of acromegalic patients have an enlarged thyroid, which may compress the trachea
- Preoperative assessments help the anesthesiologist to understand the possibility of difficulties with airway management and tracheal intubation
- Difficult airway
- Macroglossia and enlarged epiglottis: Difficult bag-mask ventilation and direct laryngoscopy
- Recurrent laryngeal nerve palsy, narrow glottic opening, subglottic narrowing (stridor)
- Nasal turbinate enlargement: Caution with nasal intubation and consider a smaller endotracheal tube
Suggested reading
- Menon R, Murphy PG, Lindley AM. Anaesthesia and pituitary disease. Continuing Education in Anaesthesia Critical Care & Pain. 2011;11(4):133-137.
- Smith M, Hirsch NP. Pituitary disease and anaesthesia. Br J Anaesth. 2000;85(1):3-14.
- Seidman PA, Kofke WA, Policare R, Young M. Anaesthetic complications of acromegaly. Br J Anaesth. 2000;84(2):179-182.
Clinical updates
Giustina and Colao (New England Journal of Medicine, 2025) emphasize that diagnostic delay in acromegaly still averages >5 years and is directly associated with higher GH/IGF-I levels, vertebral fractures (≈30% at presentation), cardiovascular disease, and increased mortality, underscoring IGF-I measurement as the key screening test when clinical suspicion arises. They detail evolving multimodal management, highlighting improved surgical outcomes in expert centers, expanded roles for oral octreotide and the oral SSTR2 agonist paltusotine to maintain biochemical control after depot SRLs, selective use of pasireotide (with GLP-1 agonists to manage hyperglycemia), pegvisomant achieving IGF-I normalization in ~70–90%, and combination regimens to optimize tumor control and metabolic outcomes, while noting that persistent quality-of-life impairment and excess cardiovascular/oncologic mortality remain concerns.
Freda (Expert Review of Endocrinology & Metabolism, 2025) highlights that acromegaly remains underdiagnosed with a median ~5-year delay, and that early/mild cases are particularly challenging because IGF-1 may be only modestly elevated and GH can suppress to <1.0 µg/L after oral glucose. She emphasizes interpreting IGF-1 and GH together using assay-specific cutoffs, considering factors such as BMI, estrogen use, and comorbidities that alter results. She advocates an individualized treatment strategy, surgery as first-line, followed by tailored medical therapy (first-generation SRLs, pasireotide, pegvisomant, or cabergoline, alone or in combination) based on tumor characteristics, glucose status, and predictors of response, to optimize biochemical control, tumor stability, and comorbidity management.