Etiology
Cerebral vasospasm is usually caused by subarachnoid hemorrhage (SAH) due to the exposure of the vessels to blood. Occasionally, traumatic brain injury, vasculitis, or meningitis can also result in vasospasm.
Tips
- Daily TCDs are indicated from day 3-5 after SAH, but the highest incidence of vasospasm is usually 8 days after the initial bleed.
- Vasospasm may occur in up to 70% of patients presenting with SAH.
- Postoperative edema can make the diagnosis of vasospasm challenging.
View
Position 1: Transtemporal

Transducer position for a transtemporal Doppler examination of cerebral vasospasm.
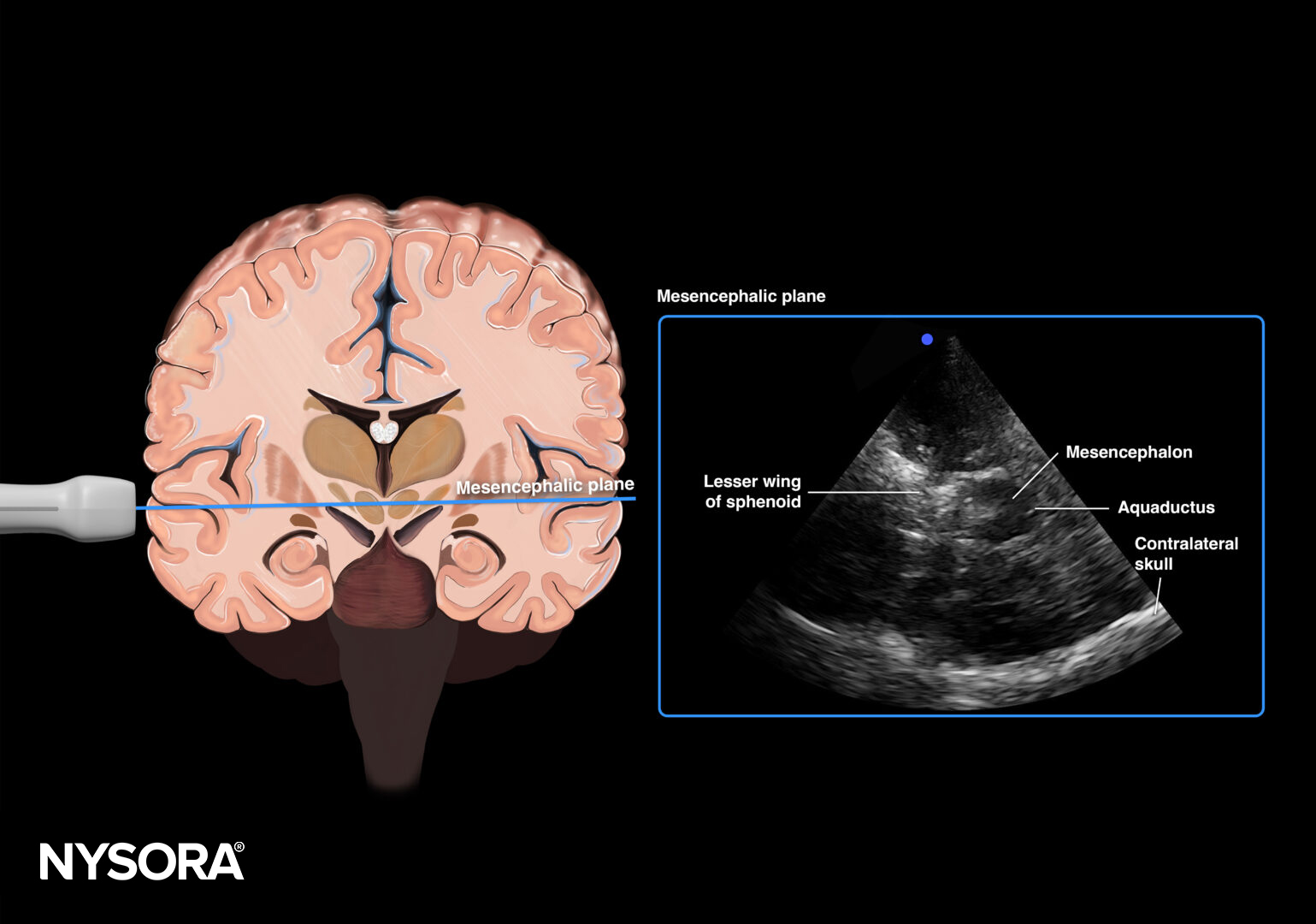
Mesencephalic plane.
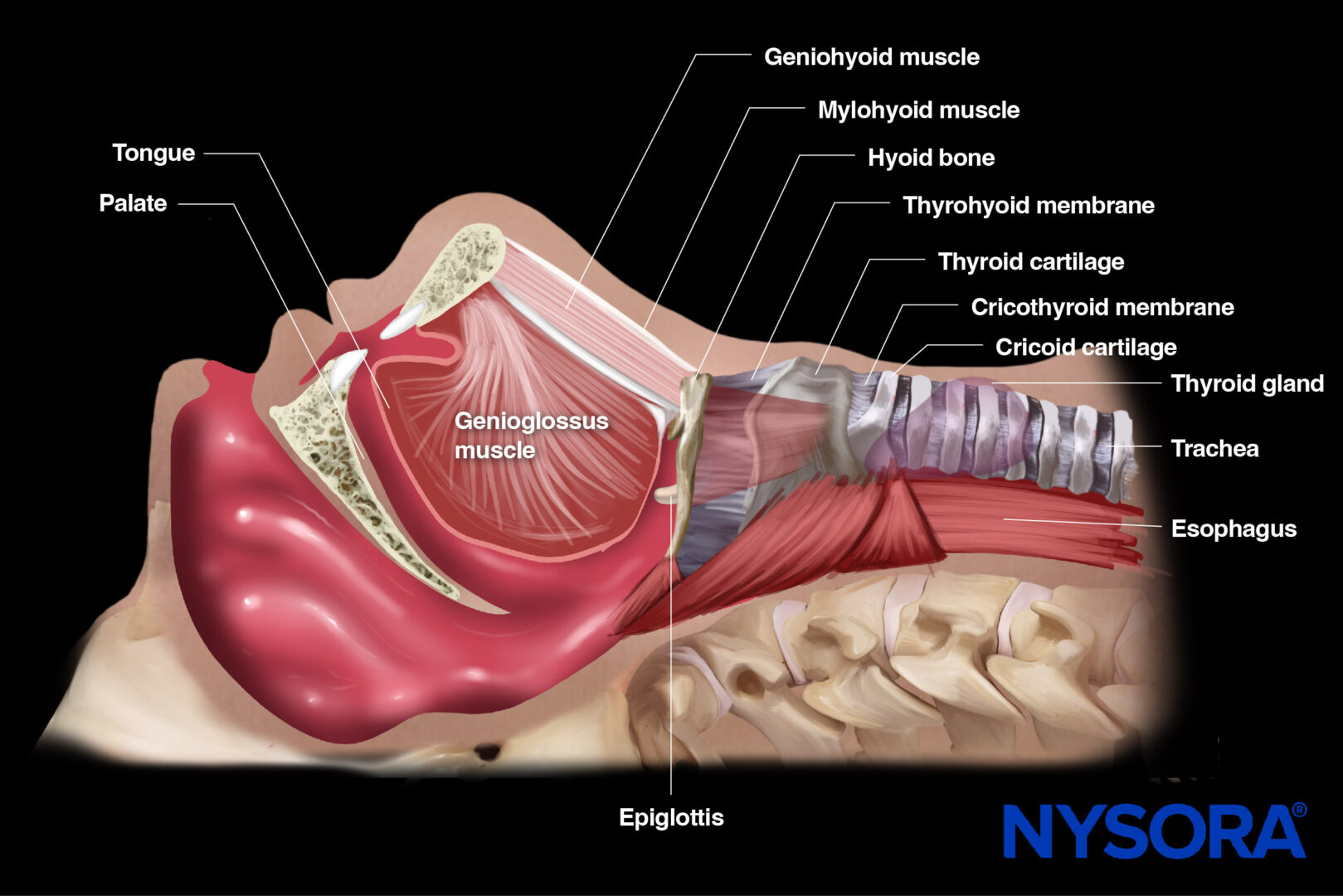
Position 2: Submandibular

Transducer position for a submandibular Doppler examination of cerebral vasospasm.
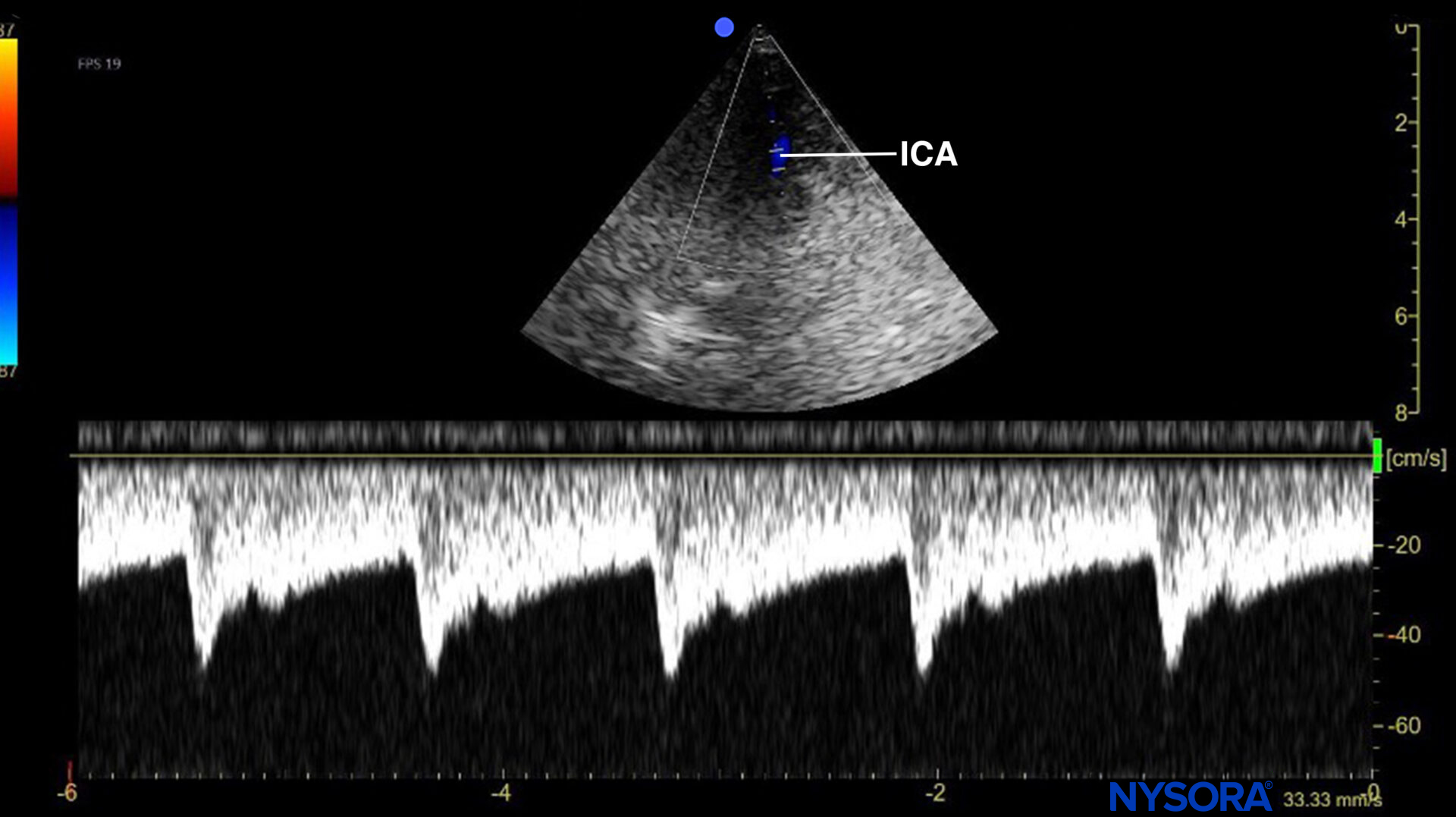
M-mode view of the internal carotid artery (ICA).
Assessment
Cerebral vasospasm assessment requires multiple steps:
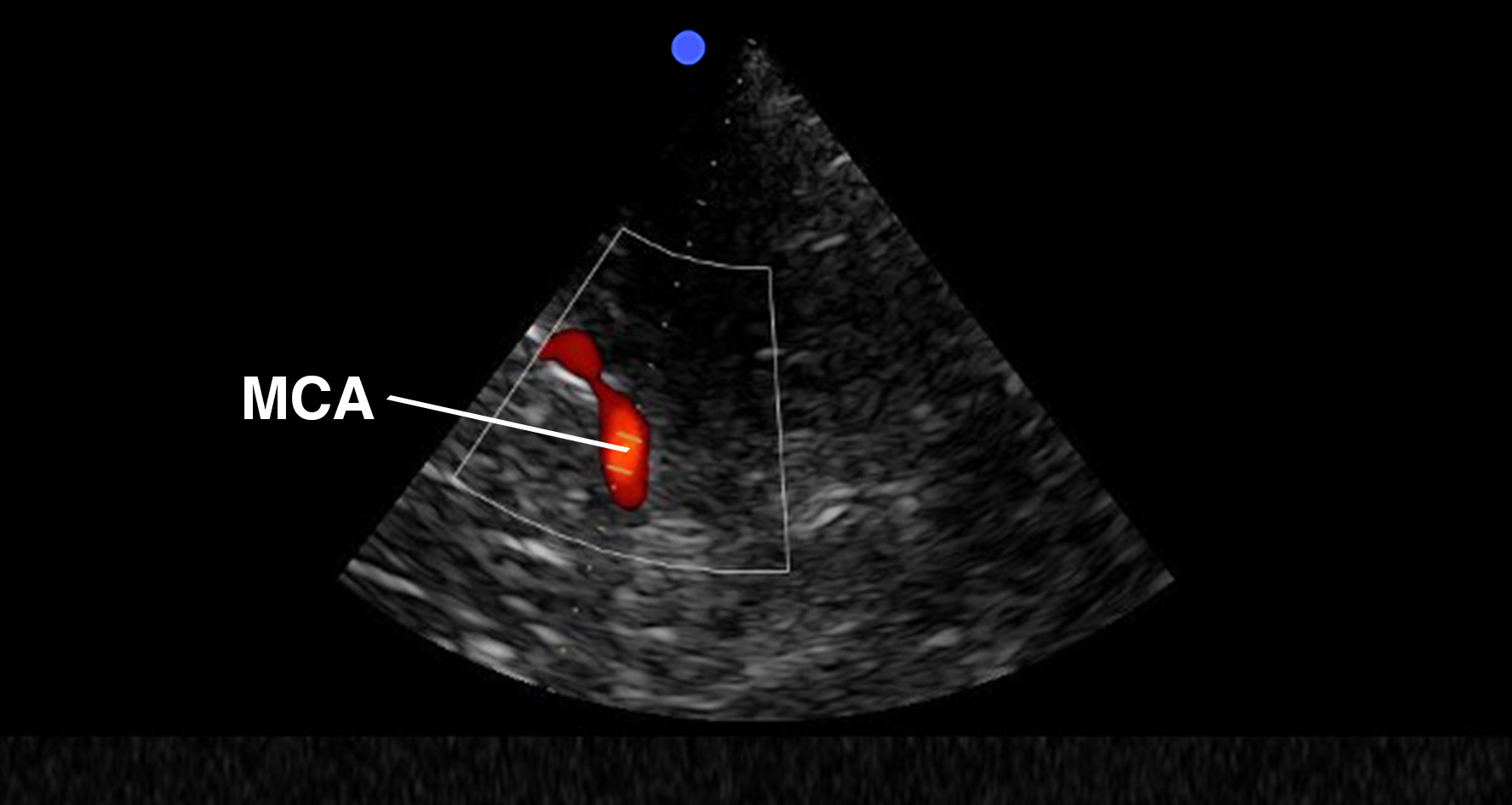
- Use the mesencephalic plane and activate pulsed wave Doppler. Position the Doppler gate on the middle cerebral artery (MCA) and trace the flow velocities.
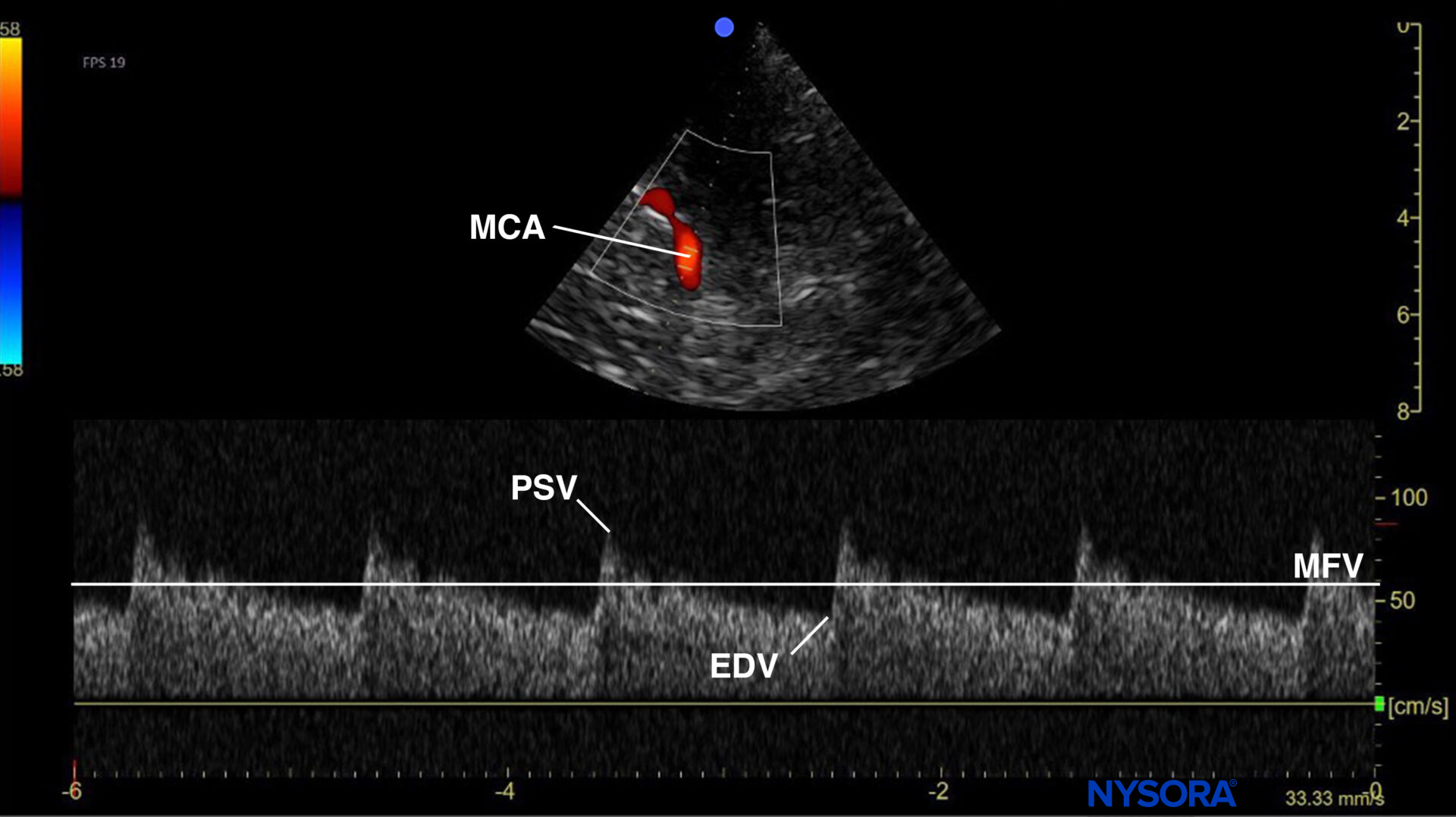
Mesencephalic plane pulsed wave Doppler with the Doppler gate on the middle cerebral artery (MCA). Evaluation of flow velocities in the MCA. PSV, peak systolic velocity; EDV, end-diastolic velocity; MFV, mean flow velocity.
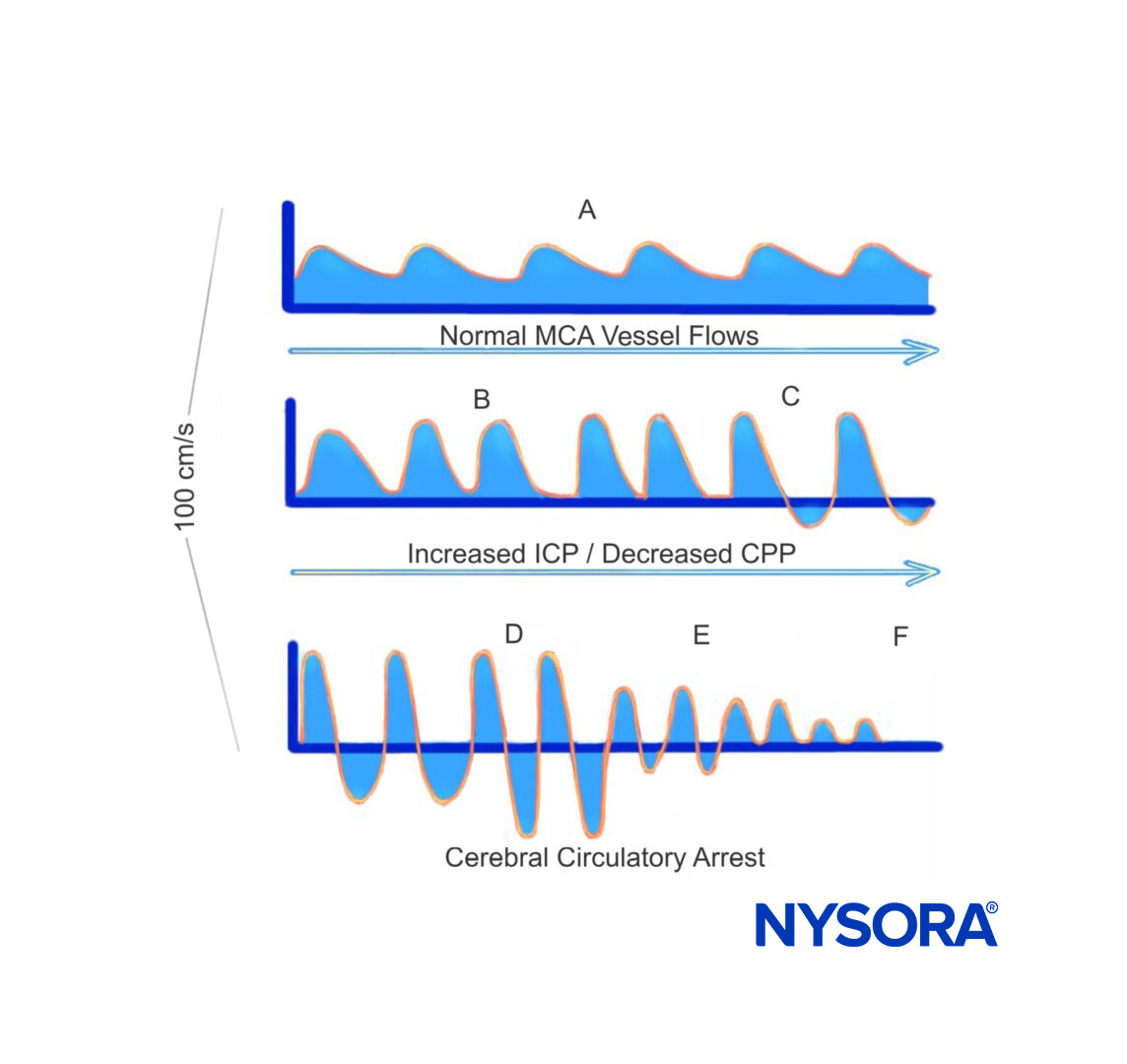
Normal findings include:
- Mean flow velocity < 80 cm/s
- Sharp upstroke (systole)
- Stepwise deceleration (diastole)
The following flow velocities are associated with vasospasm:

- Measure the flow velocities in the internal carotid artery (ICA).
Use the phased array transducer and position it high in the neck, pointing toward the vertex. Position the Doppler gate on the ICA to obtain the flow velocity, and trace it (usually 4-5 cm).
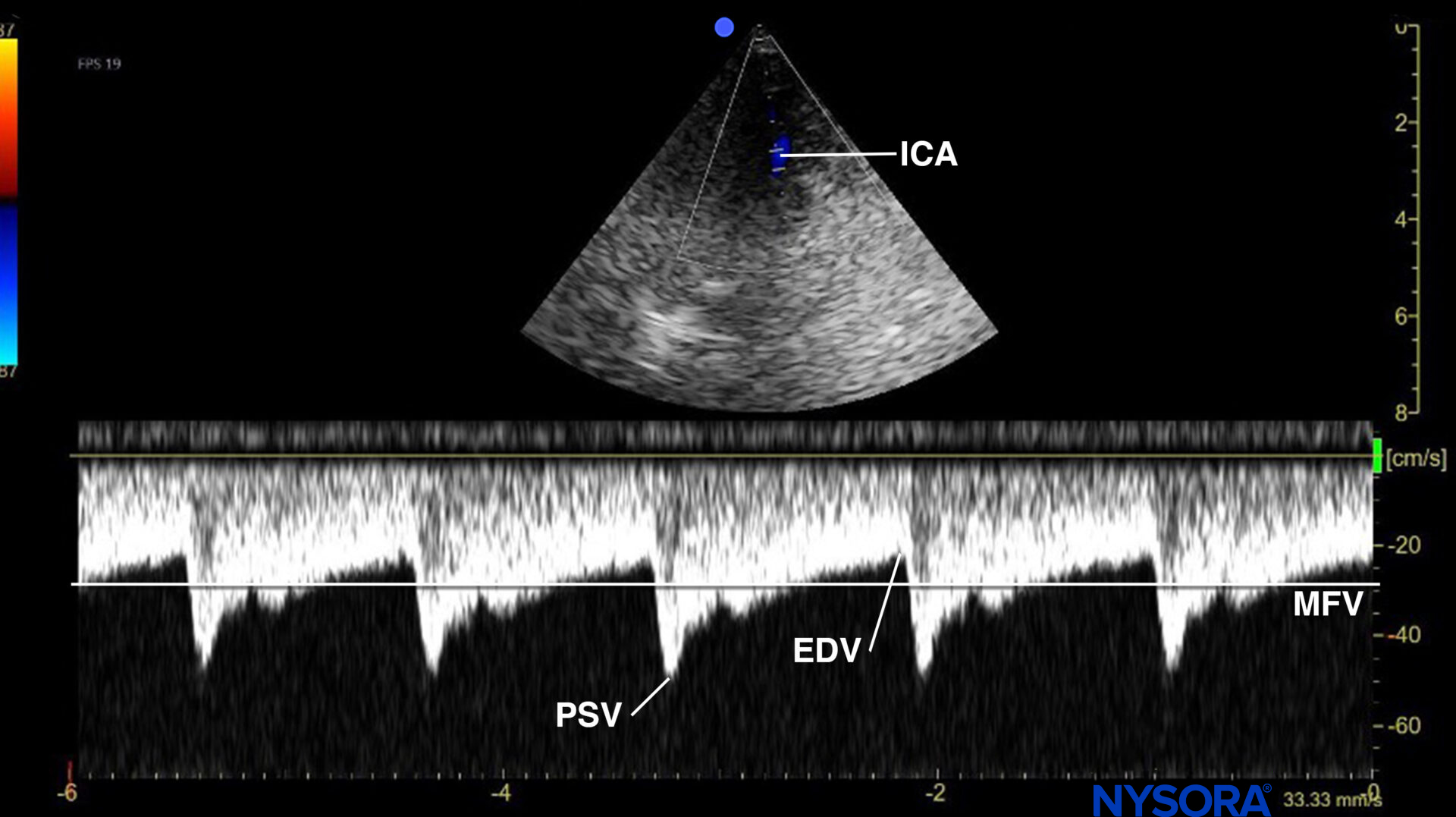
Pulsed wave Doppler of the flow in the (terminal extracranial) internal carotid artery (ICA). PSV, peak systolic velocity; EDV, end-diastolic velocity; MFV, mean flow velocity.
Note
Low diastolic flow velocities will be present for the external carotid artery. This requires you to redirect the transducer by tilting the transducer more medially. The spectral Doppler waveform of the ICA has the profile of a ‘low resistance’ circulation (gradual decline from PSV to EDV; prominent diastolic flow).
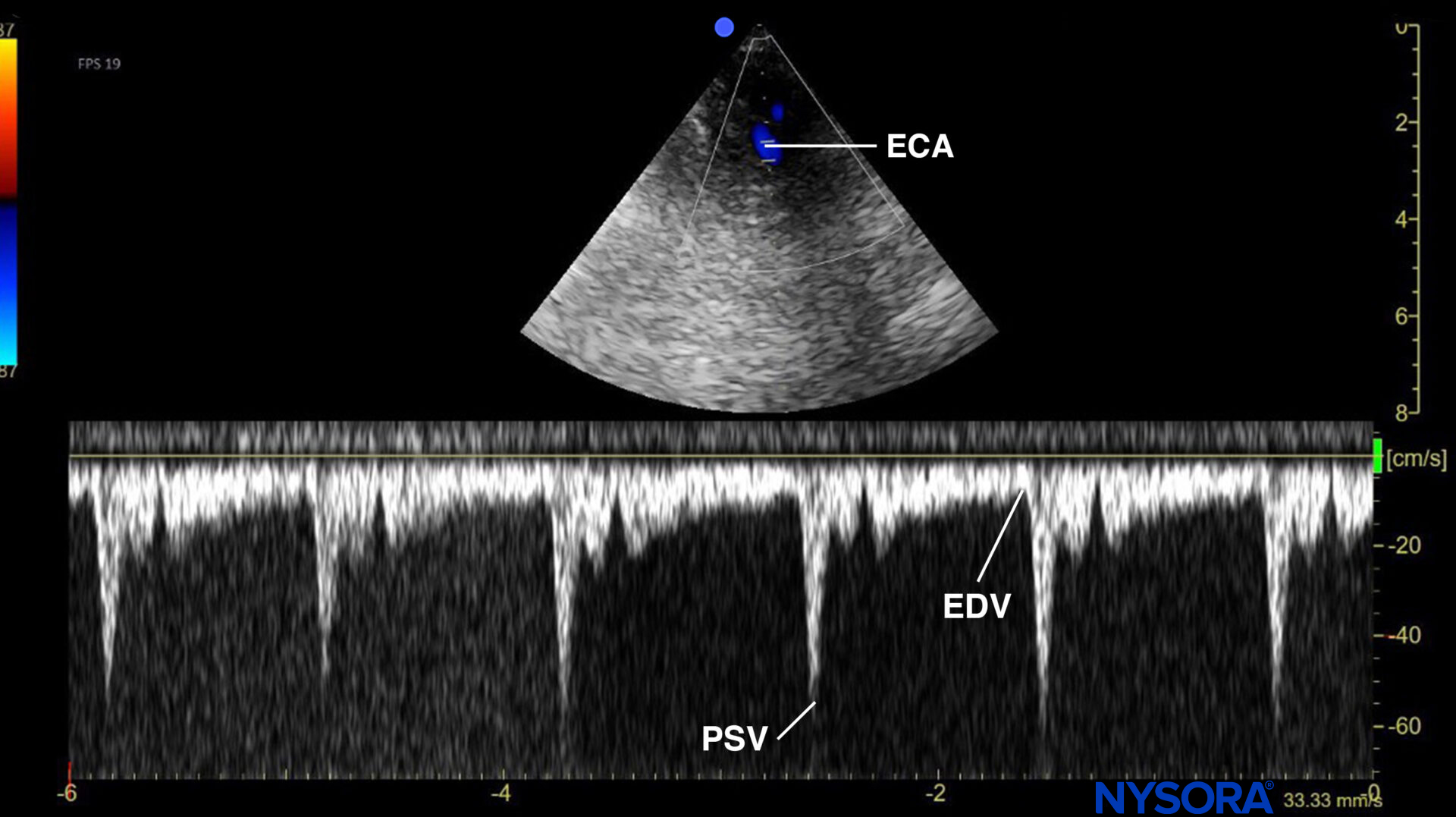
Pulsed wave Doppler of the flow in the external carotid artery (ECA) with the typical flow profile of a ‘high resistance’ circulation, with a steep decline after the systolic peak, and relatively low diastolic flow velocities. PSV, peak systolic velocity; EDV, end-diastolic velocity.
- Calculate the Lindegaard ratio to determine the severity of the vasospasm.
Lindegaard ratio = Mean flow velocity MCA / mean flow velocity ICA
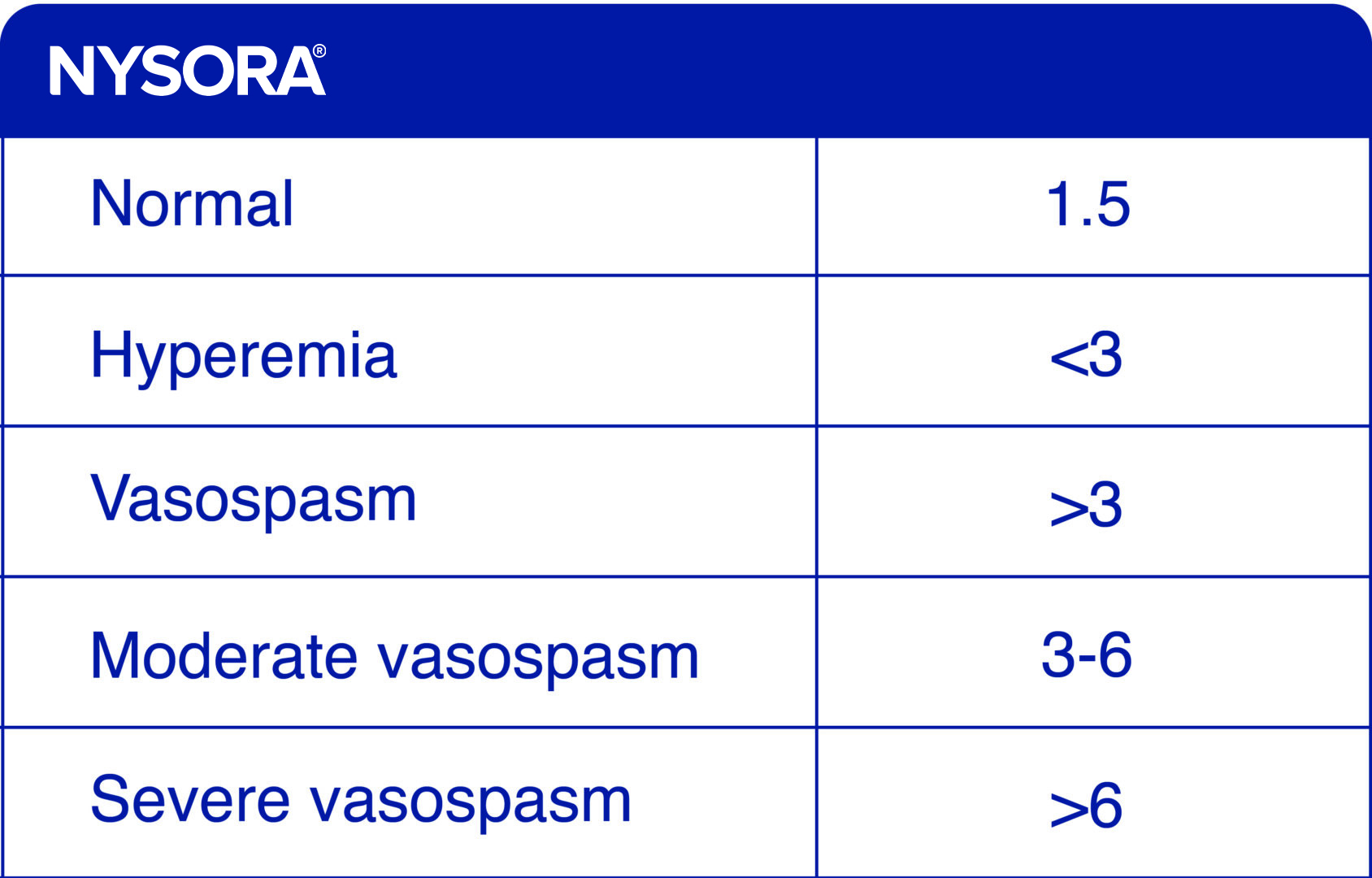

Degrees of vasospasm according to the Lindegaard ratio.
Tip
Daily follow-up allows for trend analysis of ratios in patients at risk for vasospasm.
Clinical updates
- Snider et al. (Neurocritical Care, 2022) conducted a retrospective cohort study of 262 patients with aneurysmal SAH and found that time-varying TCD-measured vasospasm severity was independently associated with delayed cerebral infarction (radiological DCI), with an adjusted hazard ratio of 1.7 per unit increase in spasm severity. Vasospasm within a specific vessel (e.g., right MCA) predicted infarction in that same vascular territory (aHR 2.0), supporting spatial specificity. Optimal discrimination occurred with mild vasospasm on days 4–5 or moderate vasospasm on days 6–9, yielding high negative predictive values (>90%) but low positive predictive values (~20%), reinforcing TCD’s role as an early screening tool to rule out high-risk patients rather than definitively predict infarction.
- Snider SB, Migdady I, LaRose SL, et al. Transcranial-Doppler-Measured Vasospasm Severity is Associated with Delayed Cerebral Infarction After Subarachnoid Hemorrhage. Neurocrit Care. 2022;36(3):815-821.