The BRUGANAES study, recently published in the European Journal of Anaesthesiology (2025), provides valuable insights into the anesthetic management of patients with Brugada syndrome (BrS), a rare but potentially lethal cardiac condition.
BrS poses unique perioperative challenges, especially given the long-standing concern that standard anesthetic drugs might trigger malignant arrhythmias. The BRUGANAES study challenges this assumption with data spanning 18 years and involving 189 anesthetic procedures.
What is Brugada syndrome?
Brugada syndrome is a genetic channelopathy associated with sudden cardiac death due to life-threatening ventricular tachyarrhythmias. It’s characterized by:
- Abnormal ECG findings (notably, type 1 coved ST elevation in right precordial leads)
- Mutations, particularly in the SCN5A gene, affecting cardiac sodium channels
- Symptoms such as syncope, seizures, or nocturnal agonal breathing
- Increased risk during fever, bradycardia, electrolyte imbalances, or under certain drugs (e.g., local anesthetics, propofol)
Study overview: BRUGANAES
Objective:
To assess the incidence of malignant arrhythmias during and up to 30 days post-anesthesia in BrS patients.
Design:
- Retrospective cohort (2006–2023)
- Conducted at Hospital Clínic of Barcelona
- Included 111 patients undergoing 189 procedures
Primary outcome:
- Occurrence of malignant ventricular arrhythmias or sudden cardiac death (SCD)
Secondary outcomes:
- Hospital complications
- 30-day readmissions
- 30-day mortality
Key findings
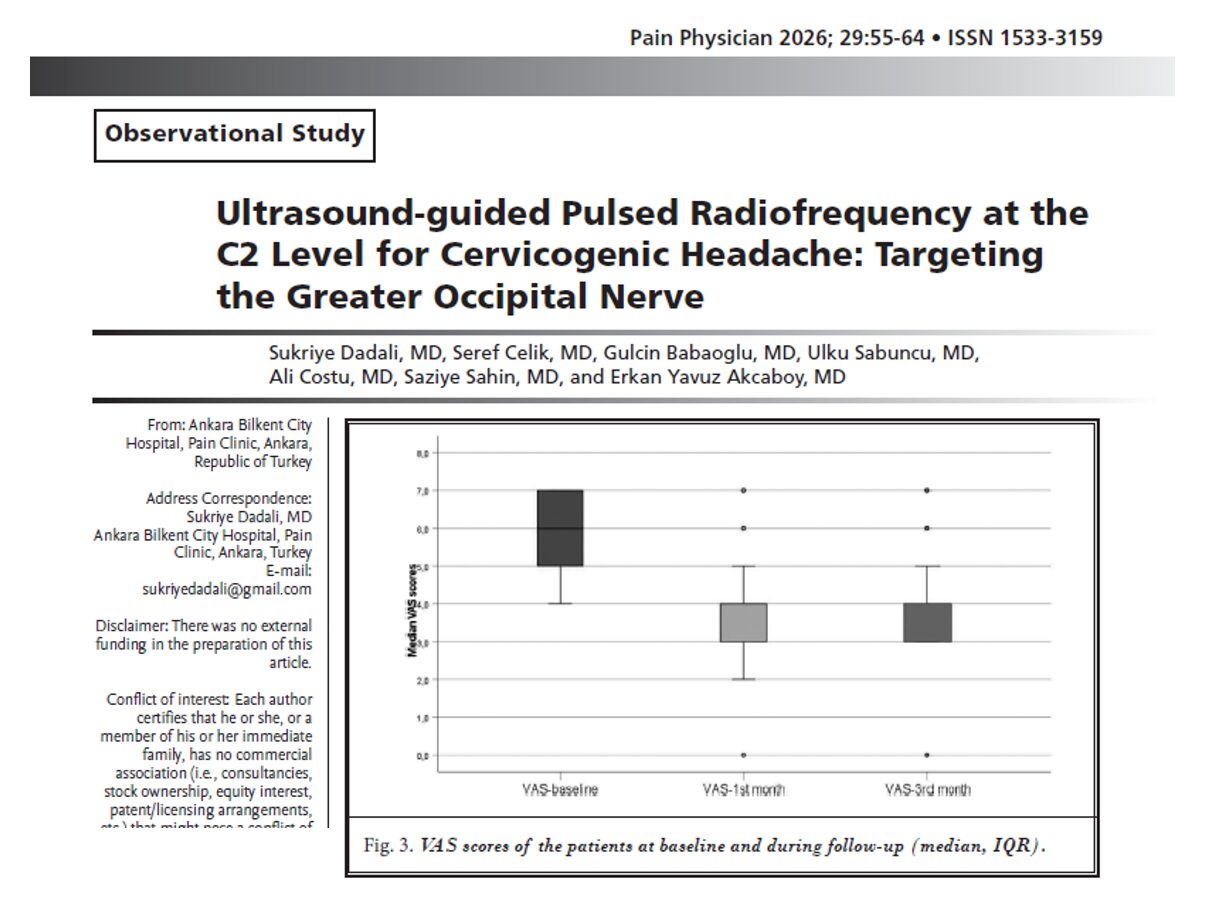
- Only 2 procedures (1%) led to intraoperative malignant arrhythmias
- No post-operative arrhythmias or deaths were reported within 30 days
- 129 (68.3%) procedures used non-recommended drugs like propofol, ketamine, or local anesthetics
- Propofol was used in 50.3% of all procedures
- No arrhythmias occurred in patients receiving neuraxial or peripheral blocks
Anesthetic approaches in BrS
Drug classifications
- Non-recommended drugs: Propofol, ketamine, tramadol, and local anesthetics
- Recommended drugs: Opioids, inhalational anesthetics, thiopental, etomidate
Types of anesthesia used:
- General anesthesia: 45.5%
- Procedural sedation: 31.2%
- Regional/neuraxial alone: 12.7%
- Mixed techniques: 10.6%
Regional anesthesia details:
- Drugs used:
- Bupivacaine (36.4%)
- Levobupivacaine (22.7%)
- Mepivacaine (20.9%)
- Ropivacaine (13.9%)
- Bupivacaine (36.4%)
- No associated malignant arrhythmias despite sodium channel-blocking properties
Case highlights
-
Bradycardia-induced ventricular fibrillation:
- Occurred during ICD replacement
- Patient received thiopental and sevoflurane
- Outcome: Death despite ECMO support
- Occurred during ICD replacement
-
Self-limited ventricular tachycardia:
- During ventricular lead extraction
- Used thiopental and sevoflurane
- Outcome: ICD re-implantation, full recovery
- During ventricular lead extraction
These events were more likely linked to surgical manipulation than the anesthetic drugs themselves.
How to manage BrS patients during anesthesia: 7 essential steps
- Pre-op assessment: Review ECG, risk stratify (ICD, syncope history, family history)
- Plan anesthesia regimen carefully: Prefer drugs with low sodium channel affinity when feasible
- Avoid triggers: Maintain normothermia, avoid bradycardia, and correct electrolytes
- Monitor ECG closely throughout perioperative period
- Use TCI pumps for precise propofol/remifentanil delivery if used
- Have defibrillation equipment available
- Post-op observation, especially in high-risk cases
Clinical implications and future directions
- The study challenges traditional caution surrounding common anesthetic agents in BrS
- It supports a more flexible and evidence-based approach
- Larger multicentre prospective studies are needed to further validate safety protocols
Conclusion
The BRUGANAES study provides the strongest evidence to date that common anesthetic drugs, including propofol and local anesthetics, are likely safe in Brugada syndrome patients when used appropriately. With informed planning and vigilant monitoring, anesthesiologists can provide safe perioperative care for this high-risk group.
Reference: Borrell-Vega J et al. Eighteen-year analysis of anaesthetic management in Brugada syndrome: The BRUGANAES study. Eur J Anaesthesiol. 2025;42:458-467.
Read more about this topic in the Anesthesia Updates section of the Anesthesia Assistant App.