Learning objectives
- Describe the different types of transfusion reactions
- Recognize the signs of the different types of transfusion reactions
- Take preventative measures against transfusion reactions
- Manage the occurrence of transfusion reactions
Definition & mechanisms
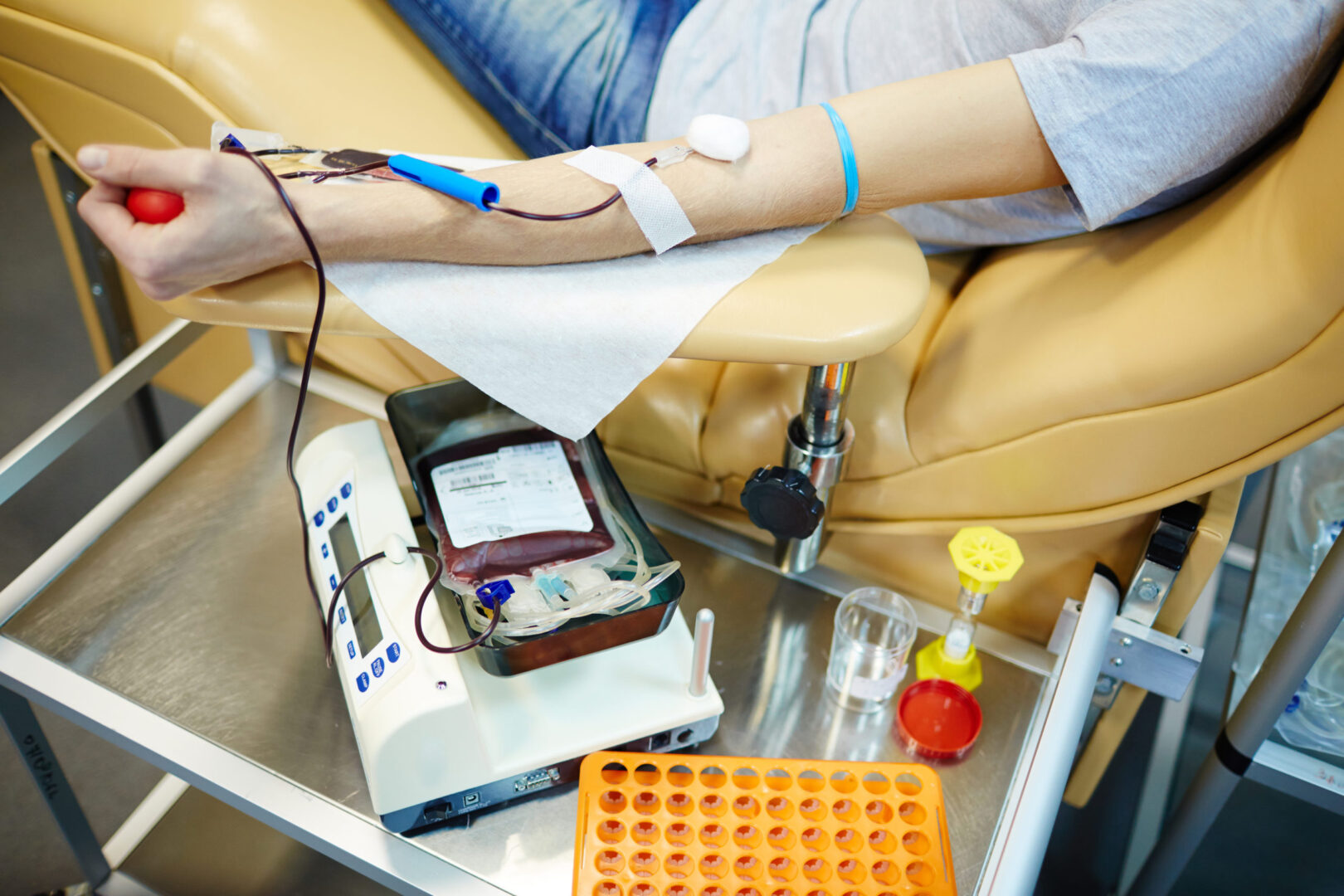
- Transfusion reactions are the most frequent adverse event associated with the administration of blood products, occurring in up to one in 100 transfusions
- There are several types of adverse reactions:
- Allergic/Anaphylactic reactions
- Acute hemolytic reactions
- Delayed hemolytic reactions
- Febrile non-hemolytic reactions
- Hyperhemolytic reactions
- Hypotensive reactions
- Massive transfusion-associated reactions
- Post-transfusion purpura
- Septic reactions
- Transfusion-associated circulatory overload
- Transfusion-associated graft versus host disease
- Transfusion-associated necrotizing enterocolitis
- Transfusion-related acute lung injury
Signs & symptoms
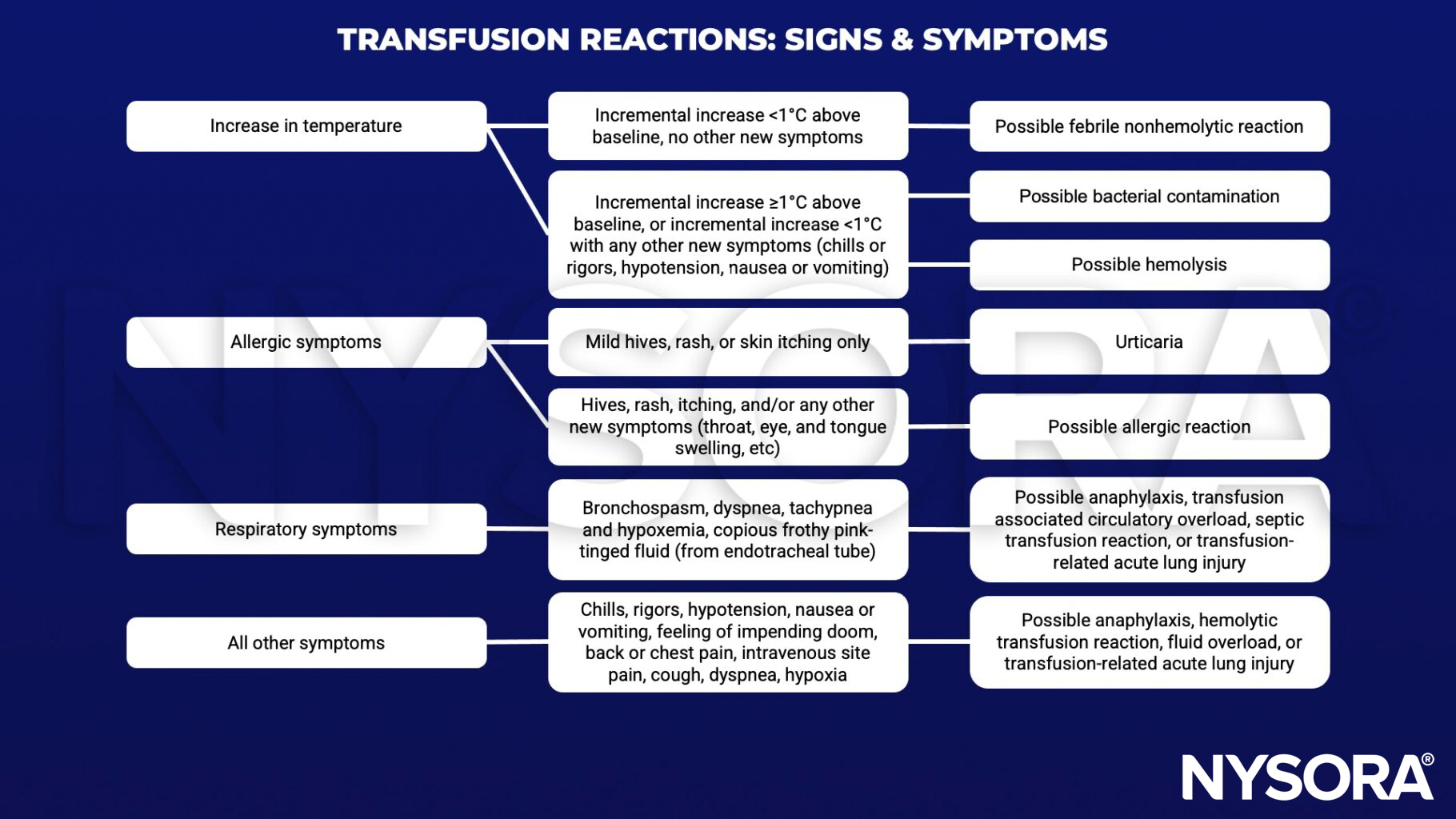
Prevention
- Comprehensive training of staff
- Close adherence to blood handling and administration policies
- Laboratory testing
- Prospective monitoring and planning
- A restrictive transfusion strategy to avoid unnecessary transfusions
Management
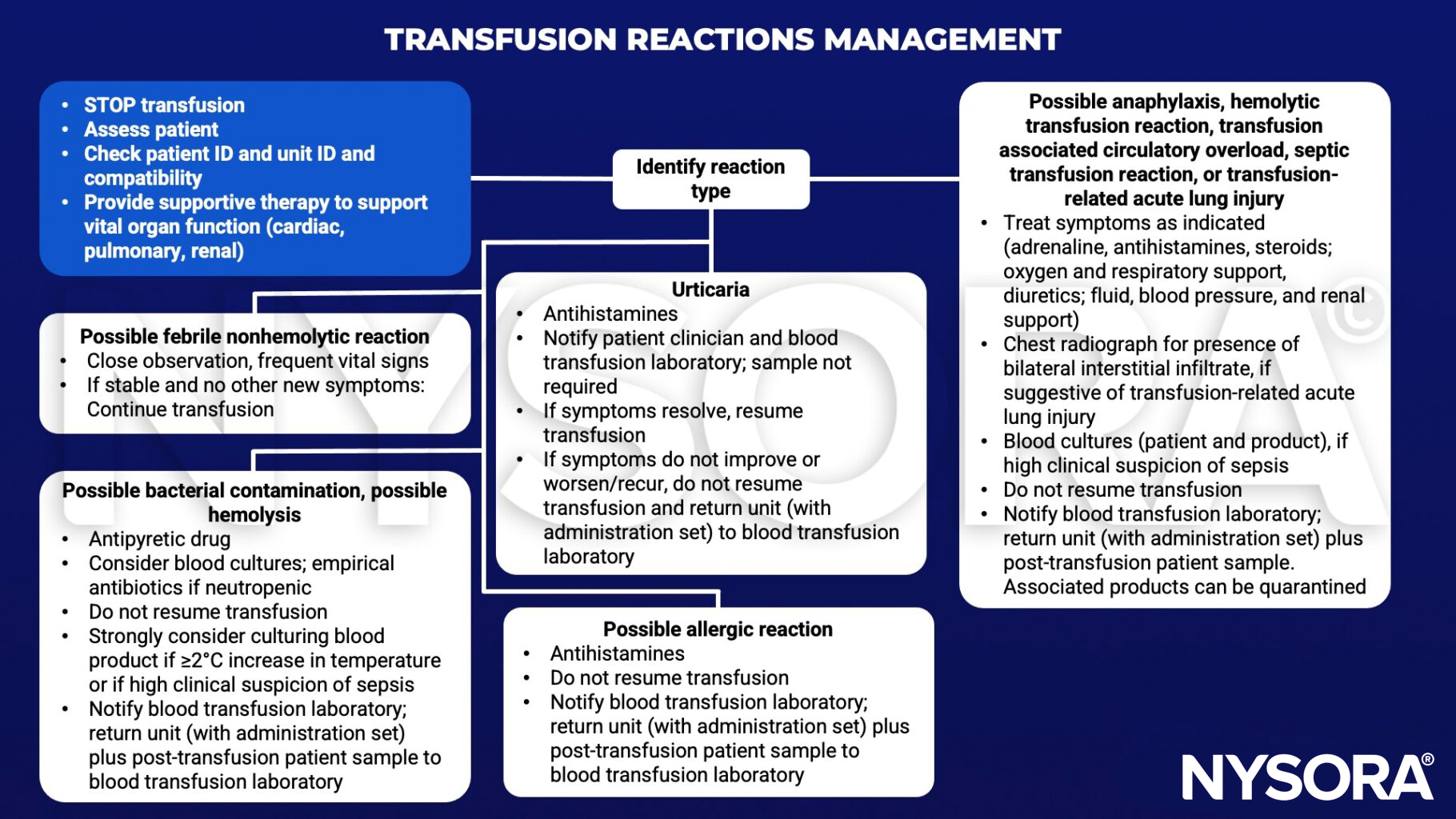
Suggested reading
- Delaney M, Wendel S, Bercovitz RS, et al. Transfusion reactions: prevention, diagnosis, and treatment. Lancet. 2016;388(10061):2825-2836.
Clinical updates
Metcalf et al. (JAMA, 2025) report updated AABB/ICTMG international platelet transfusion guidelines supporting a restrictive transfusion strategy, based on 21 RCTs and 13 observational studies showing no increase in mortality or major bleeding with lower transfusion thresholds. The recommendations lower prophylactic platelet triggers to < 10,000/μL in stable oncology and critical care patients, < 25,000/μL in non-bleeding neonates, and discourage transfusion in settings such as dengue without bleeding, cardiovascular surgery without thrombocytopenia, and intracranial hemorrhage with platelet counts > 100,000/μL. By reducing unnecessary platelet exposure, the guidelines aim to decrease transfusion-related complications while preserving limited blood product resources and improving overall transfusion safety.
- Read more about this study HERE.