Indications
An intravenous (IV) line is used to administer medication and fluids. Ultrasound-guided IV cannulation should be considered for difficult blind IV cannulation.
The following pathway can help guide the use of an ultrasound-guided technique:
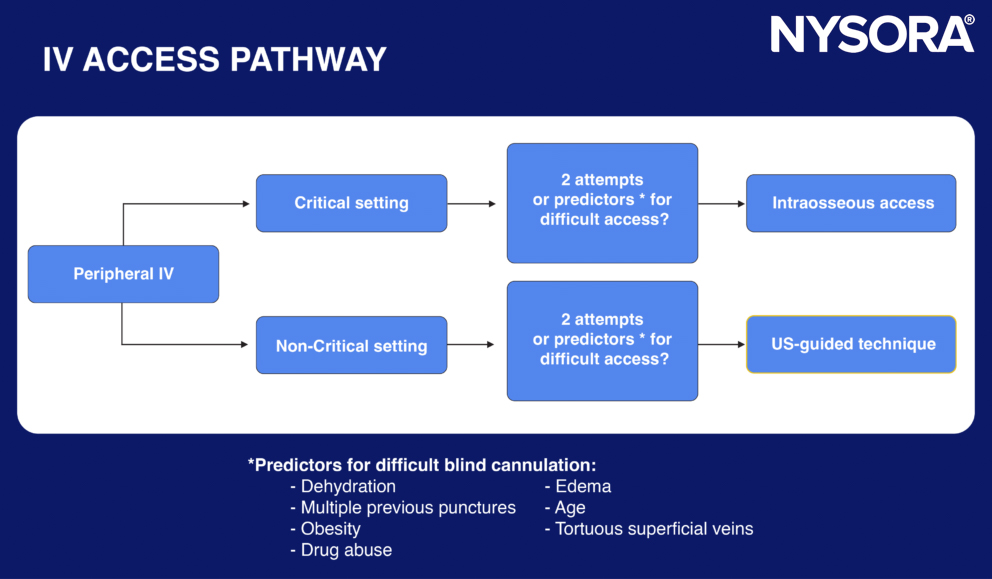
Pathway for difficult blind cannulation.
Tips
- Check with the patient if they have a history of difficult IV access.
- Prevent venous vasoconstriction: Ensure the patient is comfortable and warm to prevent vasoconstriction.
- Try to insert the catheter into the patient’s non-dominant hand.
Anatomy
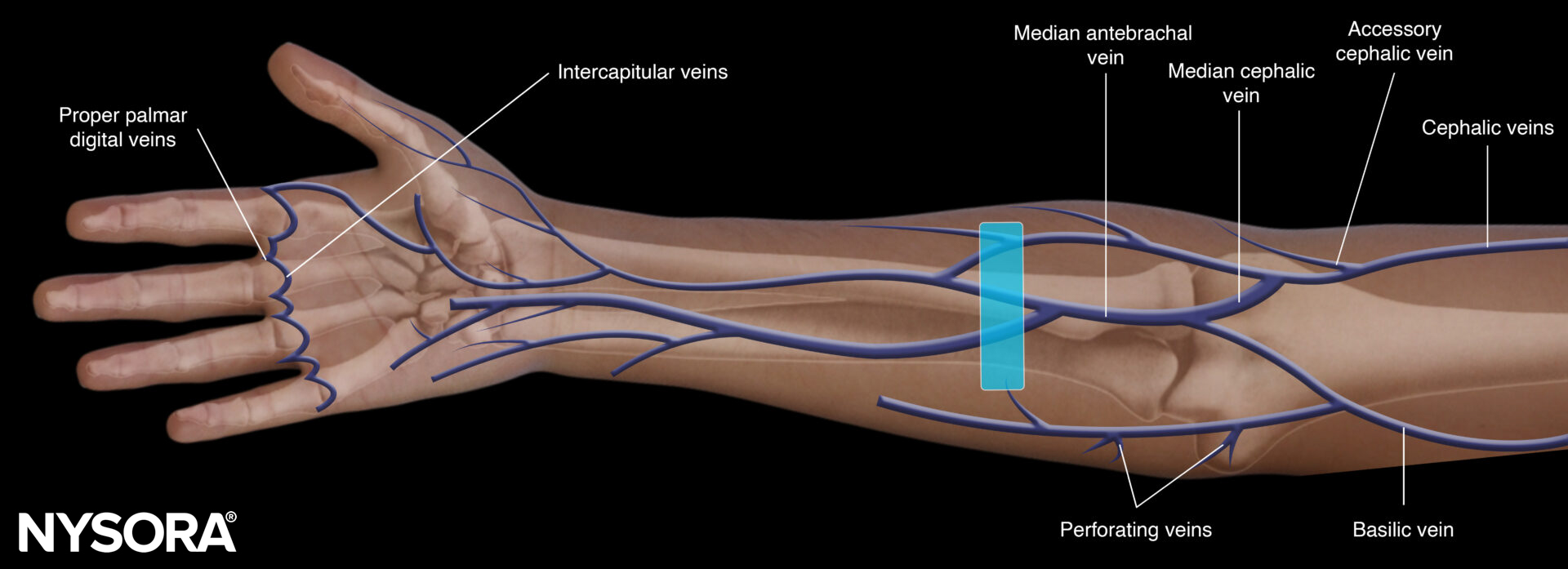
Peripheral vascular access in adults can be obtained on the upper and lower extremities.
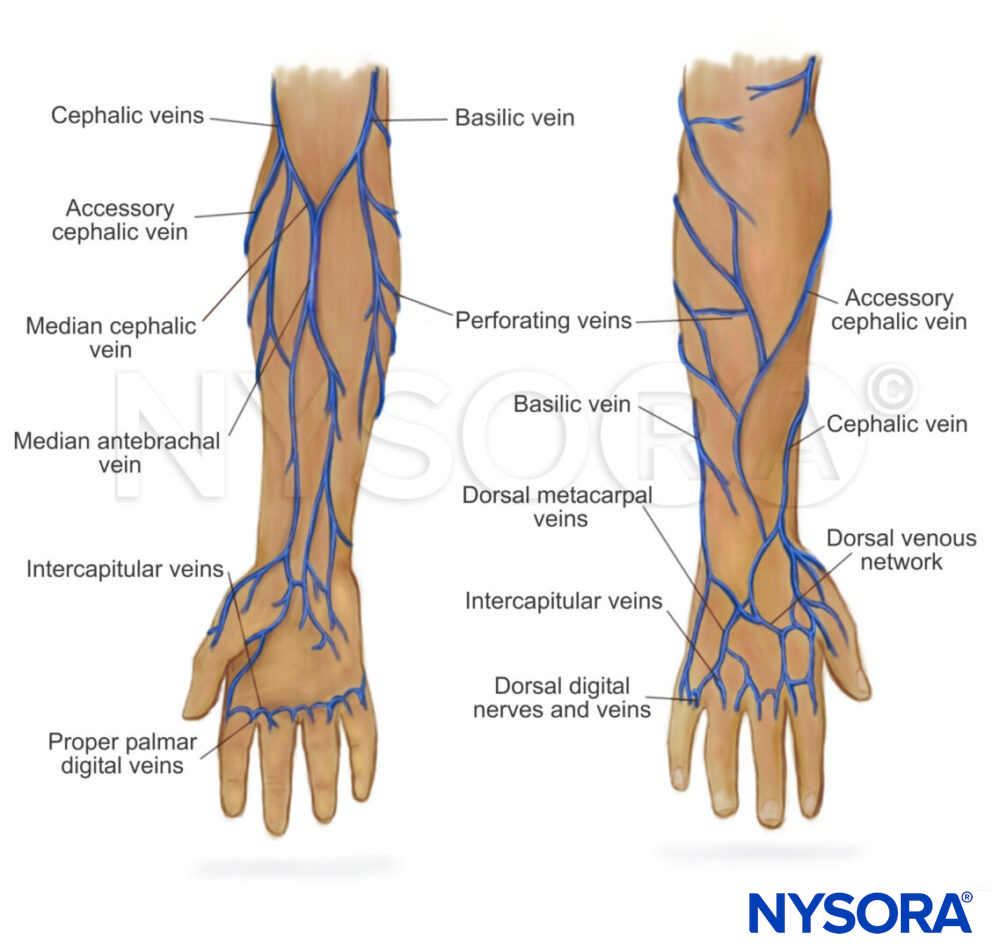

Anatomy of the veins of the upper limb and foot.
Tips
- Take sufficient time to scan the anatomic region of interest (e.g., basilic, cephalic).
- Differentiate between the superficial and deep venous structures for cannulation.
- Distal cannulation is preferred over proximal.
Preparation
- Hand hygiene
- Apply a tourniquet
- Disinfect the area of interest (2% chlorhexidine in 70% isopropyl alcohol)
- Use a sterile drape
- Use a sleeve or Tegaderm to cover the transducer
- Wear sterile gloves during the procedure
- Use sterile gel
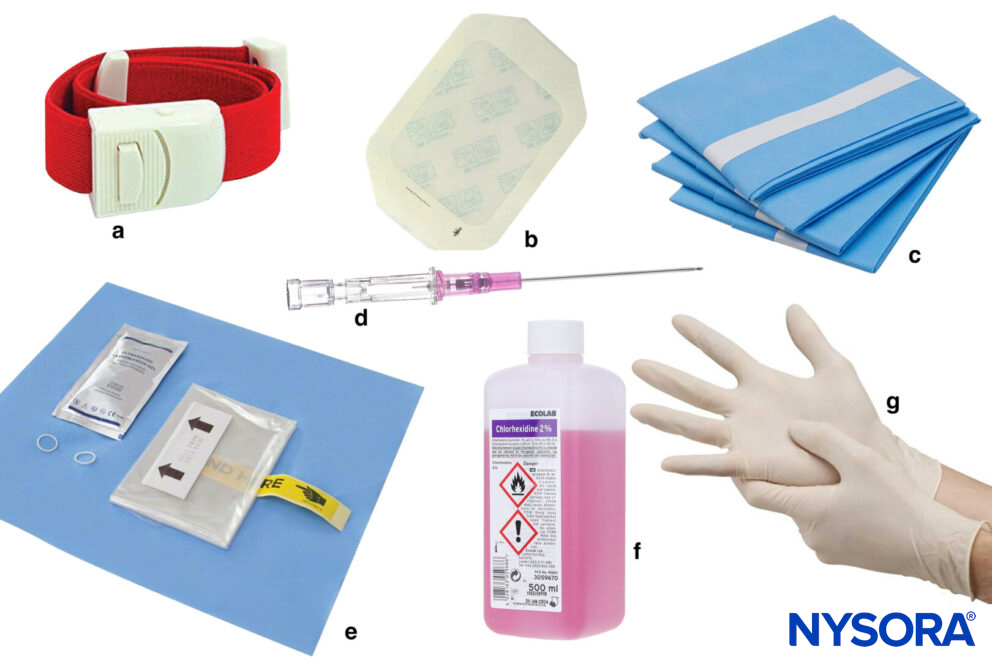
a, Tourniquet; b, Tegaderm; c, Sterile draping; d, Cannula; e, Sterile ultrasound sleeve; f, Antiseptic; g, Sterile gloves.
Tip
Always use a long cannula for ultrasound-guided IV insertion.
Patient position
- Make sure the patient is sitting or lying comfortably.
- Expose the extremity of interest.
- Position yourself at a 90-degree angle toward the structure.
Technique
The transducer is placed on the arm with a transverse orientation, and the search for the optimal puncture site is initiated.
Possible transducer position for venous cannulation.
The puncture site selection is the most important factor for successful venous cannulation. The best possible chance for successful cannulation is on a linear section of a larger peripheral vein or at the level where two smaller peripheral veins collide in a Y-junction.
Both an in-plane and out-of-plane technique can be used, but the out-of-plane technique is preferred for peripheral vascular access. Before the actual puncture, it is best to scan dynamically to image the vein’s direction. Use the creep technique to keep the needle tip in view at all times.

Out-of-plane cannulation of a peripheral vein.
Tips
- Apply minimal pressure with the transducer.
- When a tourniquet is applied, there will be no flow in the vein.
- Where possible, aim for superficial structures.
- The needle bevel needs to face up for insertion.
- Advance the needle far enough so the catheter can be threaded.
- Only check for a blood flash after the desired needle position is achieved on the US screen.
Clinical updates
- Johnston et al. (Anaesthesia, 2025) emphasize ultrasound as a central pillar of safe vascular access, recommending real-time ultrasound guidance for all central venous access and routine use for upper arm catheters, with a pre-procedure “scouting” scan and continuous needle-tip visualization to confirm intravascular wire position before dilation . The guidelines advise abandoning routine landmark-only training in ultrasound-available settings, recommend long peripheral or midline catheters when ultrasound is required for difficult peripheral access to reduce extravasation risk, and stress vessel preservation through ultrasound-based vein selection to maintain a catheter-to-vessel ratio <33% and optimize haemodilution for irritant infusions.
Johnston AJ, Simpson MJ, McCormack V, et al. Association of Anaesthetists guidelines: safe vascular access 2025. Anaesthesia. 2025;80(11):1381-1396.
- Hansen and Solbakken (BMJ Open, 2024) conducted a qualitative study of nine ICU critical care nurses and found that point-of-care ultrasound (POCUS) for peripheral IV access in patients with difficult intravenous access (DIVA) “simplifies a complicated procedure,” improving first-pass success, action readiness, workflow independence, and patient experience. Nurses reported that ultrasound enabled more appropriate vein/device selection for high-risk infusions, facilitated shared visualization with patients to reduce distress, and expanded professional role satisfaction, though skill maintenance required frequent practice.
Hansen ØM, Solbakken R. Experiences and perceptions of critical care nurses on the use of point-of-care ultrasound (POCUS) to establish peripheral venous access in patients with difficult intravenous access: a qualitative study. BMJ Open. 2024;14(6):e078106.