Current regional anesthesia procedures require two operators. An anesthesiologist who holds an ultrasound scanner in one hand and uses this to guide the needle tip placement using their other hand. A second trained operator then operates the syringe to inject the anesthetic around the target nerve bundle. The second operator is responsible for performing the aspiration and injection when instructed by the anesthesiologist while they operate the needle and ultrasound.
With the current procedure, the anesthesiologist is reliant upon 2-way communication with the assistant to ensure that the correct amount of anesthetic is injected into the patient at an acceptable pressure. This relies on the assistant making a similar subjective assessment of the injection pressure to the anesthesiologist. There may also be delays or errors in communication when there is a need to make adjustments, contributing to the potential for the procedure to encounter complications.

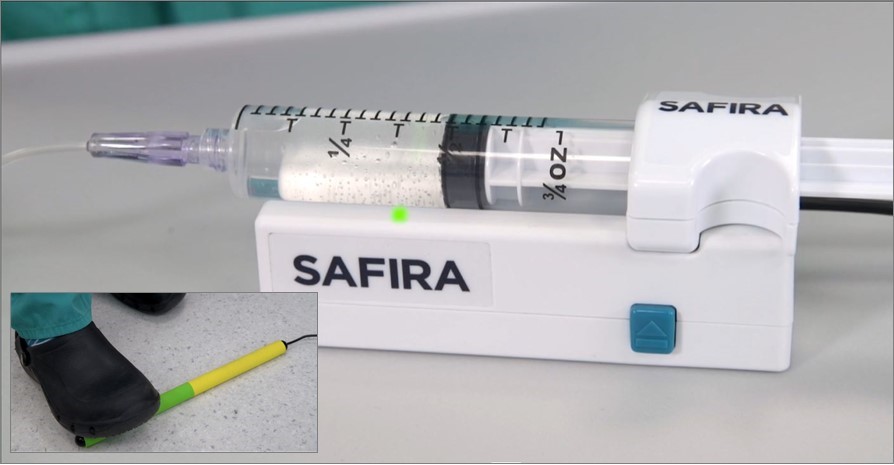
SAFIRA™: SAFer Injection for Regional Anesthesia, is a new device that enables the anesthesiologist to conduct a regional block without the need of a second operator in support. The SAFIRA™ system comprises a syringe, a syringe driver unit, and a foot pedal. Easily assembled, the system allows the anesthesiologist to hold the needle in one hand, and the ultrasound in the other while they can control the aspiration and injection themselves using the foot pedal operator.
The SAFIRA™ system also has a built-in mechanism that monitors the injection pressure and automatically stops infusion, preventing injection at pressures above 20psi. This further aids the anesthesiologist when conducting a nerve block themselves and reduces the risk of nerve damage for the patient.
Amid the current COVID-19 pandemic, recommendations by both ASRA and ESRA state that Regional Anesthesia (RA) is preferred over General Anesthesia (GA) for patients with COVID-19 to reduce the risk of transmission. Regional Anesthesia obviates the need for mechanical ventilation, preserves respiratory function, and decreases virus aerosolization and potential for viral transmission. By supporting the transition to a one-person procedure SAFIRA compliments this recommendation.
Healthcare organizations also continue to be challenged with escalating costs and decreased funding. The adoption of SAFIRA has the potential to not only improve patient safety but also to generate efficiency gains, optimize processes, and support the appropriate utilization of resources.