Learning objectives
- Describe the indications & contraindications of one-lung anesthesia
- Perform one-lung anesthesia
- Manage hypoxia during one-lung anesthesia
Background
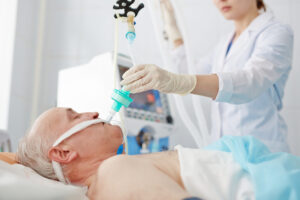
- One-lung anesthesia defines the process of complete functional separation of the lungs
- Involves ventilating one lung and collapsing the other
- Facilitates certain types of surgery, but causes significant physiological disadvantages
Indications
- Protective isolation
- Prevent contamination or spillage of infectious material (pus or secretions) from the contralateral lung
- Prevent massive hemorrhage
- Control the distribution of ventilation between the two lungs in the presence of:
- Bronchopleural fistula
- Giant unilateral cyst/bulla
- Surgical opening of major airway
- Tracheobronchial tree disruption
- Unilateral bronchopulmonary lavage (e.g., for alveolar proteinosis)
- Video-assisted thoracoscopic surgery
- Facilitate surgical exposure (e.g., pneumonectomy, lobectomy, thoracoscopy, esophageal surgery, thoracic aneurysm, thoracic spinal surgery)
Contraindications
- Patient dependent on bilateral ventilation
- Intraluminal airway masses
- Hemodynamic instability
- Severe hypoxia
- Severe COPD
- Severe pulmonary hypertension
- Known or suspected difficult intubation
Lung separation
- Double lumen tube: Allows rapid transition between one-lung ventilation and two-lung ventilation, most commonly used technique
- Bronchial blockers: Do not facilitate ventilation or suction distal to the blocker
- Uncut tracheal tube: Can be advanced into the relevant main bronchus, generally only used in emergency situations
- Papworth BiVent tube: New double lumen tube designed to facilitate rapid and reliable lung isolation using a bronchus blocker without endoscopic guidance
Technique (double lumen tube)

Complications
- Hypoxemia is one of the most important complications encountered during one-lung anesthesia
- Management of hypoxemia:
- Increase inspired oxygen to 100%
- Check the position of the tube with a fiberoptic bronchoscope
- Ensure adequate blood pressure and cardiac output
- Positive end-expiratory pressure 5-10 cmH2O to the dependent lung to decrease atelectasis and increase functional residual capacity
- Continuous positive airway pressure 5-10 cmH2O with 100% oxygen to the non-ventilated lung
- If hypoxemia is severe and does not resolve with the aforementioned steps: Abandon one-lung ventilation and intermittently ventilate the collapsed lung after warning the surgeon
- Early clamping of the appropriate pulmonary artery to stop the shunt
Suggested reading
- Mehrotra M, Jain A. Single Lung Ventilation. [Updated 2022 Jul 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538314/
- Ashok V, Francis J. A practical approach to adult one-lung ventilation. BJA Educ. 2018;18(3):69-74.
- Pollard BJ, Kitchen, G. Handbook of Clinical Anaesthesia. Fourth Edition. CRC Press. 2018. 978-1-4987-6289-2.