As life expectancy continues to rise, the healthcare system faces a critical challenge: safely managing the growing number of elderly patients undergoing surgery. In their comprehensive 2026 review, Tjeertes et al. present key updates on perioperative care for geriatric patients, with a strong focus on frailty assessment, shared decision-making, and outcome optimization.
The challenge of aging and surgery
Why are older adults more vulnerable?
Geriatric patients experience:
- Multiple comorbidities such as cardiovascular disease, diabetes, and dementia
- Reduced physiological reserve across all organ systems
- Increased susceptibility to postoperative complications such as delirium, infection, and functional decline
By 2050, more than 30% of Europe’s population will be over 65. The need for age-adapted perioperative strategies is more pressing than ever.
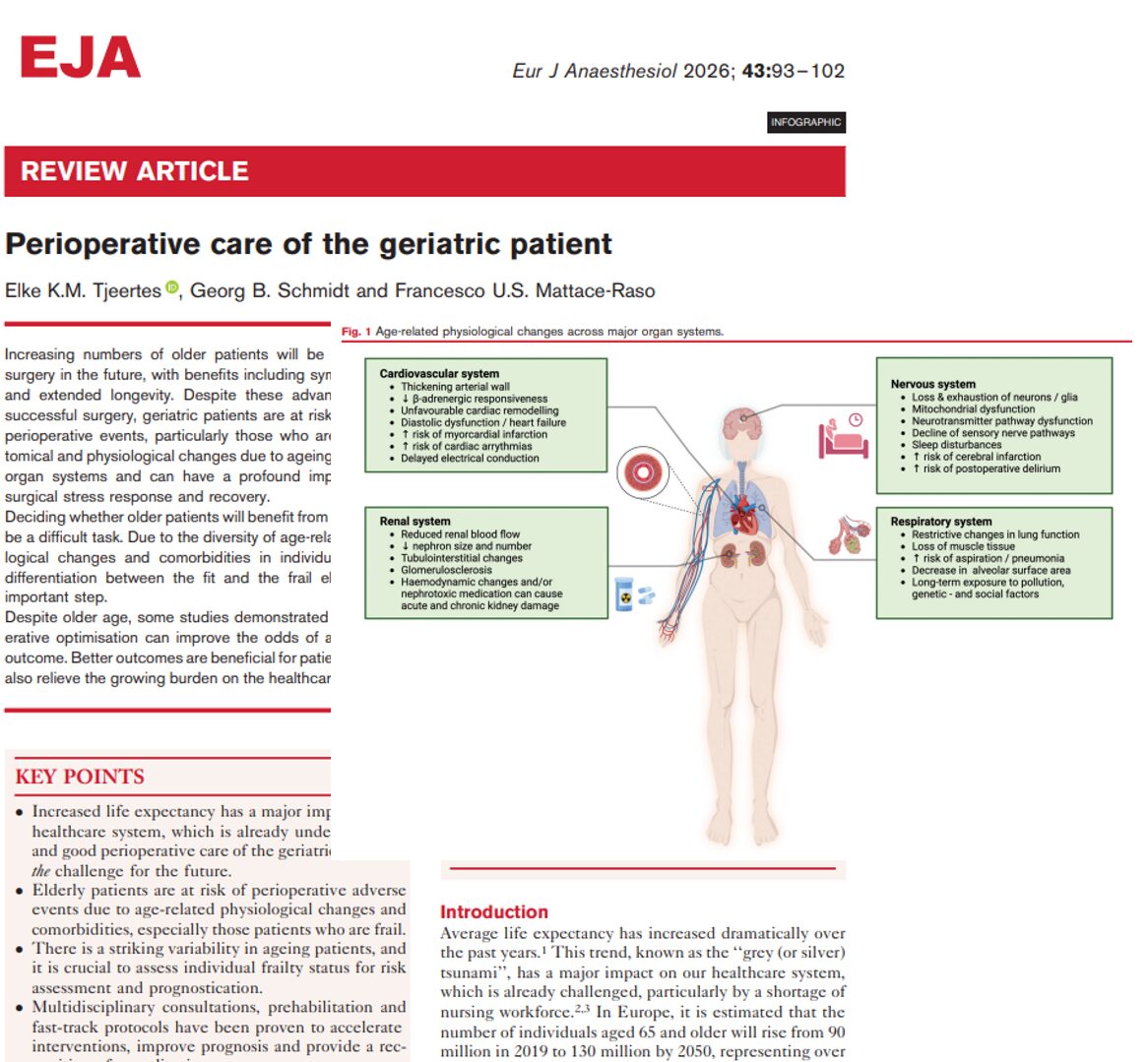
Understanding physiological changes with age
- Cardiovascular: increased arterial stiffness, impaired diastolic filling, heightened risk of arrhythmia
- Respiratory: reduced lung compliance, weakened cough reflex, aspiration risk
- Renal: decreased glomerular filtration, increased risk of drug toxicity
- Neurological: cognitive decline, vulnerability to delirium, reduced sensory perception
Frailty: a better predictor than age
Chronological age alone isn’t enough. Frailty, defined as reduced physiological reserve across multiple systems, is a stronger predictor of surgical risk.
Tools for frailty assessment:
- Clinical Frailty Scale (CFS): 9-point visual tool (see page 5) ranging from 1 (very fit) to 9 (terminally ill)
- Comprehensive Geriatric Assessment (CGA): gold standard, but resource-intensive
Frailty affects 23–53% of elderly surgical patients, depending on surgery type. It must be integrated into preoperative risk evaluation.
Step-by-step: how to optimize care for older surgical patients
-
Preoperative screening
- Assess cognitive function, nutrition, cardiopulmonary reserve, and polypharmacy
- Use frailty scales (CFS or CGA)
- Evaluate goals of care and resuscitation preferences
-
Prehabilitation programs
- Include physical training, anemia correction, and nutritional support
- Shows promise in reducing complications, even in frail patients
-
Multidisciplinary consultation
- Collaboration between anesthesiologists, surgeons, and geriatricians
- Improves outcomes and helps tailor risk-benefit analysis
-
Risk-adjusted surgical decision-making
- Consider both patient- and surgery-specific risks
- Balance potential benefits with the likelihood of functional recovery
Postoperative concerns in the elderly
Common complications:
- Delirium – highly prevalent and linked to worse outcomes
- Pneumonia and hypotension
- Renal insufficiency
- Functional loss and prolonged recovery
Enhanced Recovery After Surgery (ERAS) protocols are effective in reducing these risks and should be adapted to geriatric needs.
Advance care planning: reframing surgical intent
Surgery can be a gateway to important conversations about:
- End-of-life care
- Preferences on resuscitation and ventilation
- Quality of life versus survival
For frail patients with limited life expectancy, comfort and dignity may outweigh aggressive intervention. In carefully selected cases, nonoperative management offers humane, high-satisfaction outcomes.
Conclusion: redefining perioperative success
As the population ages, perioperative care for geriatric patients must evolve:
- Move beyond chronological age to assess frailty
- Employ multidisciplinary collaboration
- Integrate advanced care planning
- Customize prehabilitation and recovery protocols
Ultimately, success in geriatric surgery means more than survival; it means preserving dignity, function, and quality of life.
Reference: Tjeertes EKM et al. Perioperative care of the geriatric patient. Eur J Anaesthesiol. 2026;43:93-102.
Read more about geriatric patients in our Anesthesiology Module on NYSORA 360—an essential learning resource for residents with up-to-date, practical guidance across perioperative care.