Learning objectives
- Describe the physiological changes associated with aging
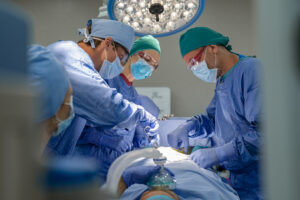
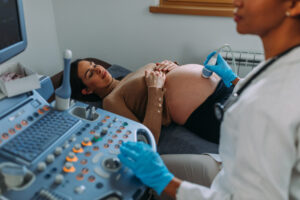
- Manage geriatric patients presenting for surgery
Background
- Geriatric patients often present with conditions requiring surgery
- Age increases perioperative risks associated with anesthesia
- Geriatric patients have a greater risk of perioperative morbidity and mortality
Physiological changes

Common surgeries in the elderly
- Cataract surgery
- Trans-urethral resection of the prostate
- Hip fracture surgery
- Knee arthroplasty
- Cholecystectomy
- Pacemaker implantation
- Colorectal excision
- Breast excision
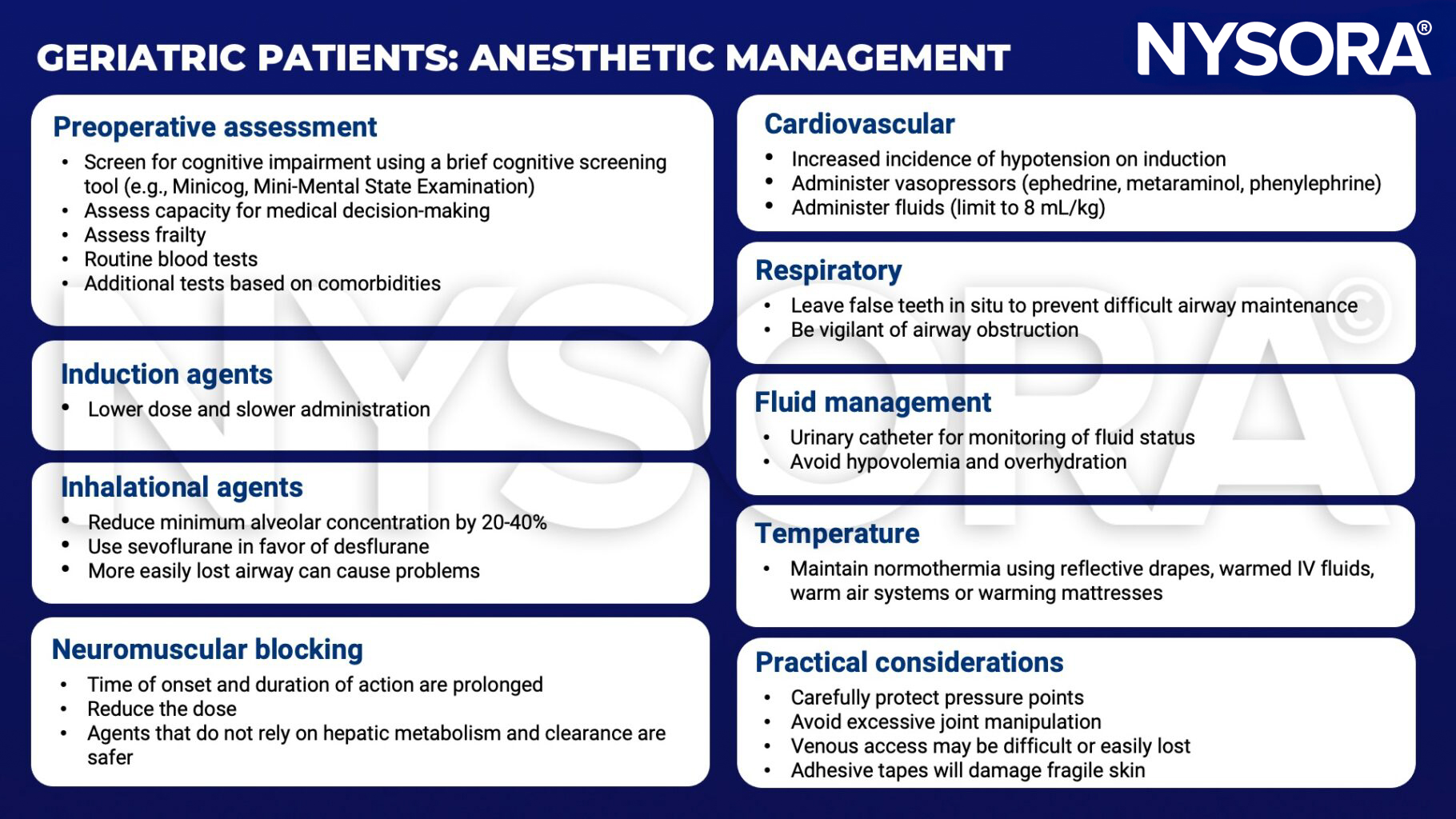
Management

Suggested reading
- Staheli B, Rondeau B. Anesthetic Considerations In The Geriatric Population. [Updated 2022 Jun 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572137/
- Murray D, Dodds C. Perioperative care of the elderly. Continuing Education in Anaesthesia Critical Care & Pain. 2004;4(6):193-6.
Clinical updates
Loggers et al. (JAMA Surgery, 2022) report from the FRAIL-HIP study that in severely frail, institutionalized adults ≥ 70 years with proximal femoral fractures, nonoperative management was noninferior to surgery for health-related quality of life, despite markedly higher short-term mortality. Nonoperative care was associated with fewer adverse events and high proxy-rated satisfaction, supporting shared decision-making and comfort-focused, palliative approaches when life expectancy is limited.
The 2024 European Society of Anaesthesiology and Intensive Care (ESAIC) guidelines emphasize that postoperative delirium is a common and preventable complication in older adults, recommending mandatory preoperative risk screening for patients ≥ 60 years. The guidelines strongly support multicomponent nonpharmacological prevention bundles (reorientation, sleep hygiene, early mobilization) and advise against routine use of antipsychotics, with dexmedetomidine reserved for selected high-risk patients.
Ardeshiri et al. (Regional Anesthesia & Pain Medicine, 2025) show that restorative neurostimulation for chronic mechanical low back pain provides durable benefit in older adults, with 62% achieving ≥ 50% pain reduction and meaningful improvements in disability and quality of life at 2 years. Outcomes in patients up to 82 years were comparable to those of younger cohorts, with marked gains in mobility and function.
- Read more about this study HERE.
Tjeertes et al. (2026, EJA) emphasize that frailty assessment is a stronger predictor of perioperative risk than chronological age and should be routinely integrated into preoperative evaluation using tools such as the Clinical Frailty Scale or Comprehensive Geriatric Assessment. The review highlights that multidisciplinary planning, targeted prehabilitation, and geriatric-adapted ERAS pathways reduce postoperative delirium, complications, and functional decline.
- Read more about this HERE.