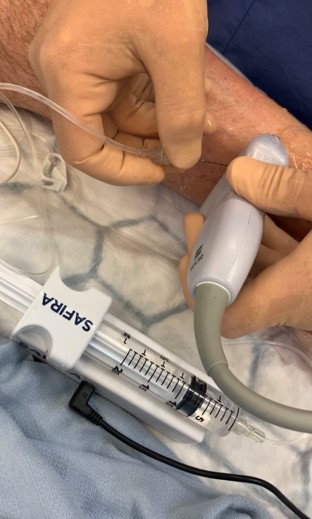
Transforming regional anesthesia into a one person procedure.
Current regional anesthesia procedures require two practitioners working closely together. An assistant controls the syringe and is required to interpret injection resistance and effectively communicate to the anesthesiologist if they feel undue resistance during injection, indicating potential high pressure.
The reliance on ‘subjective feel’ to gauge injection pressure can be problematic. By the time resistance is reported, pressure has already been applied to the system. If the needle tip is close to or in a nervous structure for example, potential nerve damage may have been caused. Studies[1] have revealed how subjective feel and sensitivity to pressure changes vary between individuals, regardless of levels of experience. Confidence that there has been no injection at high pressure levels cannot be assured.
SAFIRA™ removes the need for an assistant as the anesthesiologist can control aspiration and injection themselves using a foot pedal operator. Making regional anesthesia a one person procedure helps to remove a layer of subjectivity and gives the anesthesiologist control of the injection process. This, along with a built-in safety feature, can help support patient safety during a regional anesthesia procedure.
Unique design contributes to improved safety.
Using SAFIRA™, the anesthesiologist is in full control of the injection. This helps introduce additional objectivity, as the clinician can use their own judgements on pressure levels and the injection and apply adjustments quickly and intuitively.
SAFIRA™ also has a built in safety system which automatically prevents injection above 20psi. This helps reduce the risk of nerve damage and give clinicians more confidence around avoiding injection at pressures above 20psi. Studies have shown the risk of nerve damage occurring is higher where injection pressures are above 20psi[2].
As the Covid-19 pandemic continues to add to challenges clinical professionals face daily, SAFIRA™ supports additional safety in the clinical environment. Removing the need for an assistant, means one less person needs to be immediately present at the patient bedside or in the OR, reducing the number of individuals potentially exposed to any risk of infection. It also aids social distancing measures.
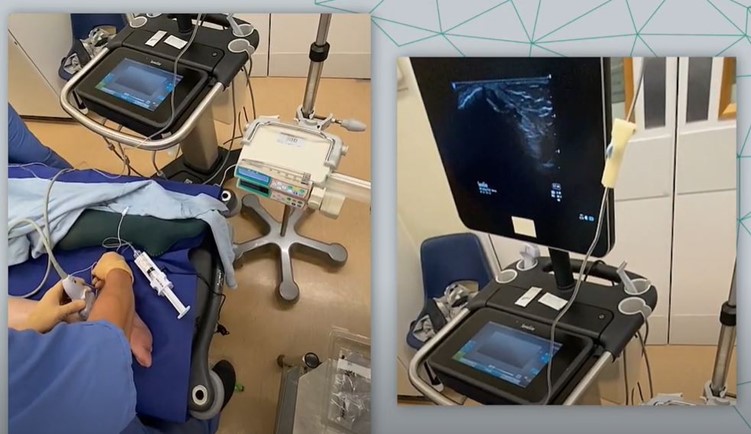
Intuitive and cost effective.
Developed by clinicians for clinicians[3], SAFIRA™ is intuitive to use and can easily be integrated into current practice. “What struck me was the simplicity, the ease of use”, observed one Consultant Orthopaedic Surgeon witnessing SAFIRA™ in use for a peripheral nerve block for the first time.[4]
SAFIRA™ also provides a cost effective solution. SAFIRA™ comprises three components: a battery powered driver and a foot pedal operator (both of which will perform approx. 200 nerve blocks before replacement), and a single-use sterile syringe. Health economics modelling has indicated a potential saving of $58 per regional block procedure[5].
Reducing the potential for nerve injury may have other cost optimisation benefits for SAFIRA™. Avoiding transient or serious nerve damage could lead to a reduced need for follow up treatments for affected patients. Fewer cases of nerve injury could potentially see a reduction in related litigation cases, lessening the cost implications and the impact of such cases on clinician wellbeing and confidence.