Herpes zoster–associated pain (ZAP) remains a major clinical challenge, particularly due to its neuropathic nature and risk of progression to postherpetic neuralgia (PHN). Patients often experience severe burning pain, electric shock–like sensations, and hypersensitivity, frequently accompanied by sleep disturbances and psychological distress. Despite antiviral therapy and conventional analgesics, pain control is often inadequate, highlighting the need for improved interventional strategies.
A recent randomized controlled trial by Li et al., published in Pain Physician (2026), evaluated an optimized ultrasound-guided thoracic paravertebral block (TPVB) incorporating parecoxib and methylcobalamin. The findings demonstrate significantly improved and sustained analgesia, along with better sleep quality, compared to standard treatment approaches.
The burden of herpes zoster–associated pain
Herpes zoster results from reactivation of the varicella-zoster virus within dorsal root ganglia. The condition progresses through distinct phases, beginning with acute neuralgia and potentially evolving into chronic PHN.
Pain mechanisms in ZAP are complex and include:
- Neuroinflammation driven by viral reactivation
- Peripheral and central sensitization
- Glial cell activation and neuroimmune dysregulation
Clinically, patients may experience:
- Persistent burning pain
- Paroxysmal electric shock sensations
- Allodynia and hyperesthesia
- Sleep disruption and reduced quality of life
Notably, long-term pain can occur in a large proportion of patients, making early and effective intervention essential.
Limitations of conventional treatment
Standard management typically includes antiviral agents, anticonvulsants such as pregabalin, antidepressants, and non-opioid analgesics. However, these approaches often fail to provide sufficient relief.
Key challenges include:
- Limited efficacy of non-opioid analgesics
- Persistent pain despite antiviral therapy
- Adverse effects from long-term medication use
- Lack of a standardized preventive strategy for PHN
These limitations have driven increasing interest in interventional pain management techniques, particularly nerve blocks.
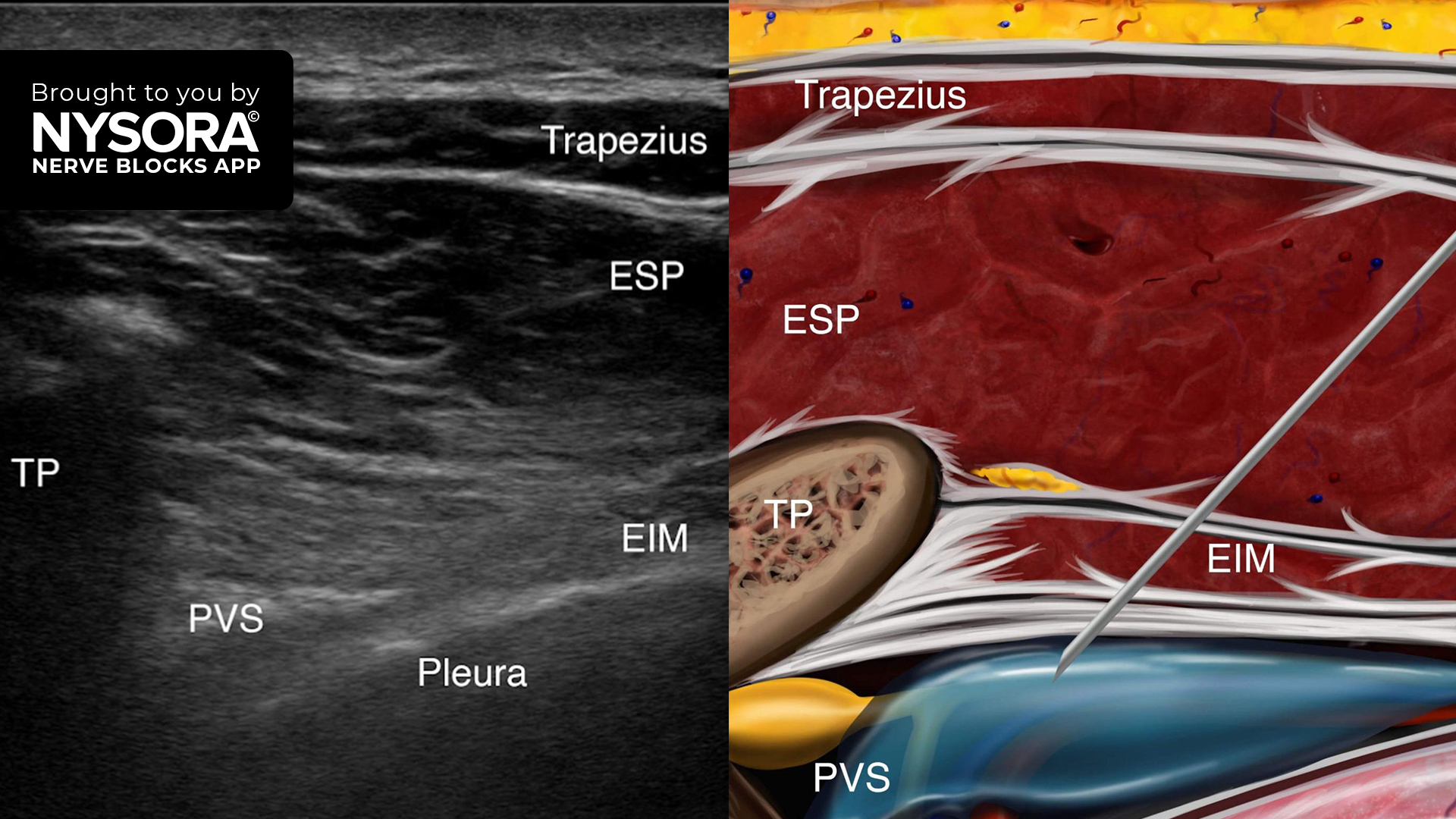
Thoracic paravertebral block: targeted analgesia
Thoracic paravertebral block is a regional anesthesia technique that delivers local anesthetic near spinal nerve roots corresponding to the affected dermatome.
Advantages of TPVB include:
- Direct targeting of affected nerves
- Reduction of peripheral sensitization
- Potential prevention of chronic pain development
- Favorable safety profile with ultrasound guidance
Study design and methodology
The study enrolled 60 patients with thoracic herpes zoster pain and randomized them into two groups.
Control group received:
- Lidocaine
- Betamethasone
- Ropivacaine
- Saline
The experimental group received:
- Same mixture plus:
- Parecoxib 20 mg
- Methylcobalamin 1000 µg
All patients were also treated with pregabalin.
Pain and sleep outcomes were measured using:
- Numeric rating scale (NRS)
- Pittsburgh sleep quality index (PSQI)
Assessments were performed at baseline, 12 hours, and 7 days post-treatment.
Superior pain control with parecoxib-enhanced block
Both groups demonstrated significant early pain reduction. However, differences emerged over time.
Key findings include:
- Rapid pain relief within 12 hours in both groups
- Sustained improvement only in the experimental group
- At 7 days:
- Experimental group NRS ≈ 2.33
- Control group NRS ≈ 3.73
Improved sleep quality outcomes
Sleep disturbance is a major consequence of ZAP and significantly impacts recovery.
Study results showed:
- Both groups improved initially
- Only the experimental group maintained improvement
At 7 days:
- Experimental group PSQI ≈ 5.40
- Control group PSQI ≈ 10.13
Safety and tolerability
A critical finding of the study was the absence of adverse events.
No patients experienced:
- Nausea or vomiting
- Respiratory depression
- Pneumothorax
- Local anesthetic toxicity
This supports the safety of combining parecoxib with standard TPVB formulations.
Why parecoxib enhances analgesia
Parecoxib is a selective cyclooxygenase-2 (COX-2) inhibitor with potent anti-inflammatory properties.
Its role in this setting likely includes:
- Reduction of inflammatory mediators
- Suppression of prostaglandin synthesis
- Enhancement of nerve block duration
When combined with:
- Local anesthetics for immediate analgesia
- Corticosteroids for anti-inflammatory effect
- Methylcobalamin for nerve repair
The result is a synergistic, multimodal analgesic strategy.
Clinical implications for practice
This study highlights several important considerations for clinicians:
- Early interventional therapy may improve outcomes in herpes zoster
- Multimodal nerve block formulations can enhance analgesic duration
- Ultrasound guidance improves precision and safety
- Improved sleep quality may accelerate recovery
Importantly, the technique may reduce the risk of progression to postherpetic neuralgia, although further research is needed.
Limitations and future directions
Despite promising results, the study has limitations:
- Small sample size
- Short follow-up duration
- Single-center design
Future research should focus on:
- Larger multicenter trials
- Long-term outcomes, including PHN prevention
- Optimization of drug combinations and dosing
Conclusion
Ultrasound-guided thoracic paravertebral block using a parecoxib-enhanced analgesic mixture represents a significant advancement in the management of herpes zoster–associated pain. By providing sustained pain relief, improving sleep quality, and maintaining an excellent safety profile, this approach offers a promising addition to multimodal pain management strategies.
As interventional pain techniques continue to evolve, integrating targeted nerve blocks with optimized pharmacologic combinations may redefine the standard of care for neuropathic pain conditions such as herpes zoster.
For more information, refer to the full article in Pain Physician.
Li D, Pan S, Huang Z, Feng T. The Efficacy of Ultrasound-Guided Thoracic Paravertebral Blocks Using a Novel Analgesic Regimen for Thoracic Herpes Zoster-Associated Pain: A Randomized Controlled Trial. Pain Physician. 2026;29(1):E19-E27.
For a detailed guide on ultrasound-guided thoracic paravertebral blocks, get your copy of NYSORA’s Ultrasound-Guided Interventional Pain Procedures Manual!