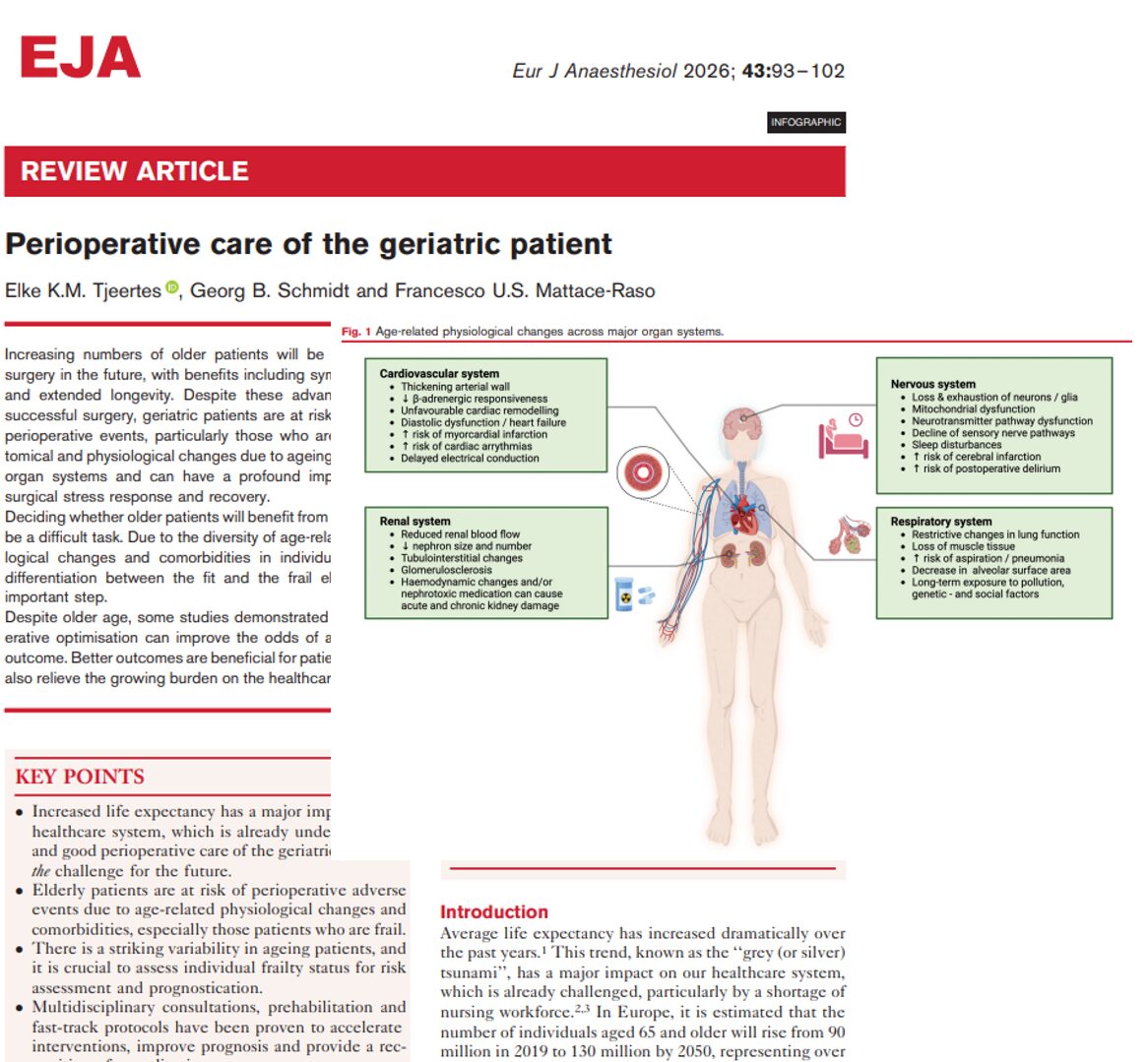
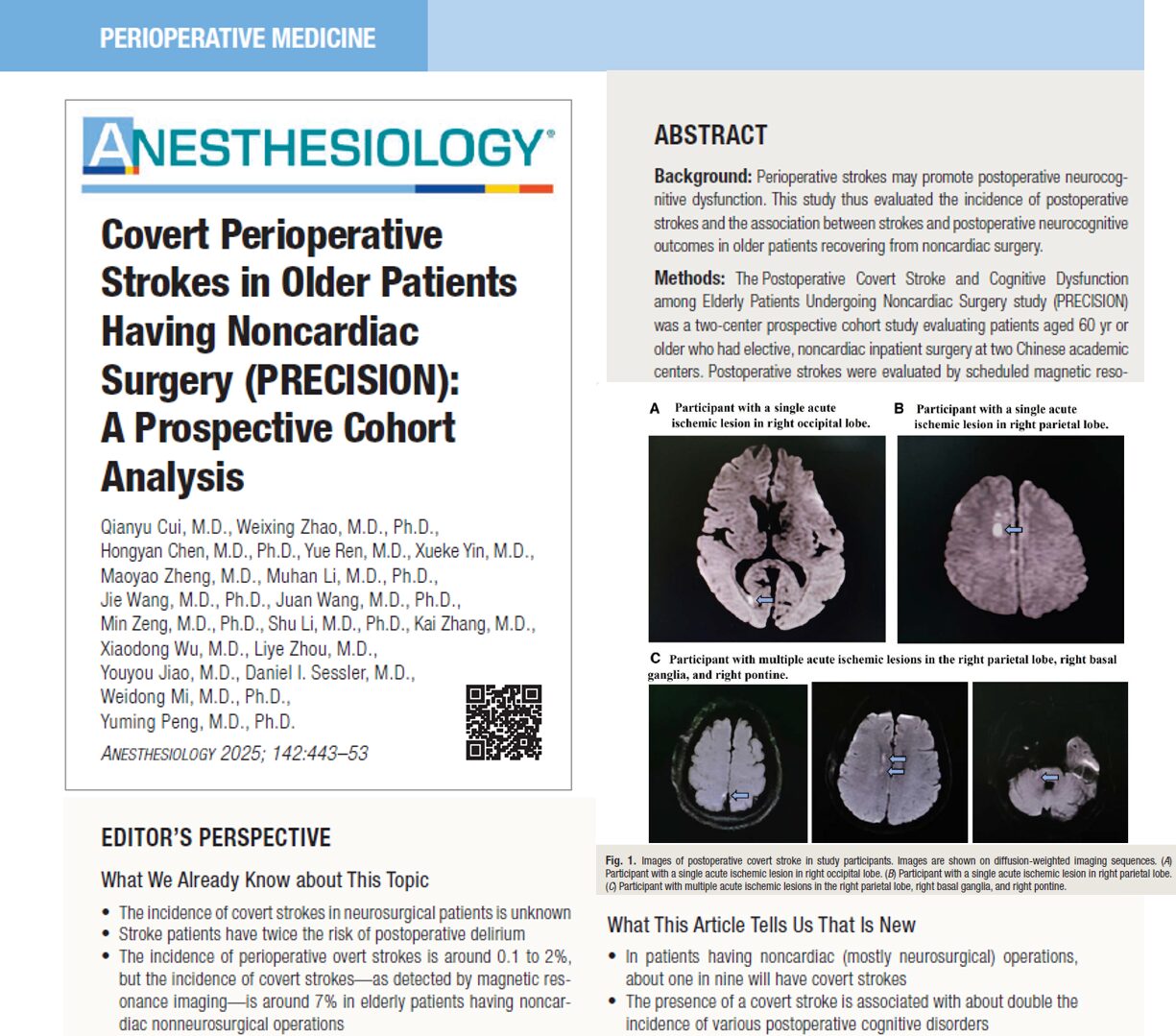
With advancements in pediatric cardiology, adult congenital heart disease (ACHD) is no longer rare. In fact, adults with CHD now outnumber pediatric patients. As this population ages, they increasingly require noncardiac surgical interventions, posing unique challenges for anesthesiologists and perioperative teams.
A 2026 review by Refakis et al. highlights the long-term outcomes, perioperative risks, and pregnancy-related considerations for ACHD patients undergoing noncardiac surgery.
Key points at a glance
- ACHD patients have tripled mortality between ages 18–68 compared to the general population.
- Many experience heart failure, arrhythmias, and multi-organ complications.
- Risk stratification is critical and now guided by composite scoring systems.
- Pregnancy in ACHD patients carries significant maternal and fetal risks.
- Multidisciplinary care and expert consultation improve surgical outcomes.
Long-term outcomes in adult congenital heart disease
ACHD patients live longer, but their complex cardiac history often leads to chronic complications:
- Common sequelae:
-
-
- Ventricular dysfunction
- Heart failure
- Valvular disease
- Arrhythmias
- Ventricular dysfunction
-
- Transplantation:
-
-
- Increased ischemic times and renal dysfunction
- Higher mortality vs. non-CHD transplant patients
- Increased ischemic times and renal dysfunction
-
- Mortality:
- ACHD patients face 3× higher mortality than general adults.
High-risk subgroups
-
-
- Prone to progressive multi-organ failure
- Survival without transplant at 35 years is <30%
- Prone to progressive multi-organ failure
-
- Tetralogy of Fallot, transposition of the great arteries:
-
- Reinterventions are often needed later in life
- Postoperative surveillance is essential but often lacking.
Assessing risk for noncardiac surgery
Refakis et al. outline a three-tiered composite risk score that integrates:
- CHD complexity
- New York Heart Association (NYHA) class
- Procedure-specific risk
Composite risk categories
- Low risk: No specific anesthetic modifications needed
- Intermediate risk: Requires anesthesia strategy adaptation and monitoring
- High risk: At elevated risk for perioperative cardiopulmonary collapse or death
Expert recommendations for perioperative care
- Refer intermediate/high-risk patients to ACHD centers
- Prefer regional/neuroaxial anesthesia when feasible
- Customize anesthesia based on risk:
- Basic monitoring for low-risk
- Invasive monitoring (arterial line, ABG) for intermediate/high-risk
- Central venous pressure monitoring for Fontan circulation
- Basic monitoring for low-risk
- Post-op ICU care for intermediate/high-risk cases
- Mandatory cardiology consults:
- For complications or emergency surgery
Common perioperative pitfalls
A landmark study outlined five “error traps” in ACHD anesthetic care:
- Poor risk communication with the team
- Inadequate ventilation strategy
- Incorrect induction approach
- Overlooked airway anomalies
- Ignoring long-term CHD complications
Pregnancy and ACHD: a high-risk intersection
Pregnancy physiologically stresses the cardiovascular system:
- ↑ Cardiac output and heart rate
- ↓ Systemic vascular resistance
- Postpartum fluid shifts
In ACHD patients, these adaptations can trigger severe complications:
- Heart failure
- Arrhythmias
- Myocardial infarction
- Thrombosis and stroke
Maternal risks
- Up to 100% risk of adverse cardiac events in WHO class IV cases
- Postpartum readmission rates are significantly elevated
Fetal risks
- Intrauterine growth restriction
- Prematurity
- CHD inheritance
- Perinatal mortality
Managing pregnancy in ACHD
Risk stratification: the mWHO classification
- Class I–II: Mild/moderate CHD – often safe
- Class III: High risk – expert center delivery required
- Class IV: Pregnancy contraindicated
Best practices for care
- Multidisciplinary cardio-obstetric team
- Prepregnancy counseling
- Use of titrated regional over general anesthesia
- Postpartum ICU admission and ≥ 1 week observation
- ECMO-capable facility for extreme cases
A 2024 study showed major cardiovascular event rates dropped from 20% to 7.7% when managed by a multidisciplinary team.
Pulmonary hypertension: a deadly comorbidity
- Prevalence in ACHD: 3.2–28%
- High maternal mortality: up to 28%
- Causes include:
- Eisenmenger’s syndrome
- Pulmonary hypertension crisis
- Right heart failure
- Eisenmenger’s syndrome
Pregnancy in this population is WHO Class IV—strongly discouraged.
Clinical workflow for ACHD surgical candidates
7-step perioperative management checklist
- Identify CHD type and previous interventions
- Assign NYHA functional class
- Assess comorbidities (renal, hepatic, pulmonary)
- Stratify surgical procedure risk
- Calculate composite risk score
- Refer to the ACHD expert if intermediate/high-risk
- Plan tailored anesthesia, monitoring, and ICU care
Conclusion
As survival improves in congenital heart disease, ACHD patients are emerging as a distinct and high-risk surgical cohort. Their care during noncardiac surgery demands:
- Advanced preoperative assessment
- Risk-based anesthesia strategies
- Multidisciplinary planning, especially during pregnancy
- Adherence to expert guidelines
With thoughtful, individualized care, the perioperative safety of this growing population can be significantly enhanced.
Reference: Refakis C et al. Patients with adult congenital heart disease presenting for noncardiac surgery. Curr Opin Anaesthesiol. 2026;39:46-51.
Read more about this study and new recommendations in NYSORA’s Anesthesia Assistant App.