Patients with a history of IV drug use often present unique challenges when establishing IV access. Adopt an empathetic approach and utilize technical solutions to establish IV access in these patients.
NOTES
Many of these patients can provide valuable feedback regarding the best IV sites, what worked in the past, where the most accessible veins are, and so on.
Here are some challenges to remember for these patients.
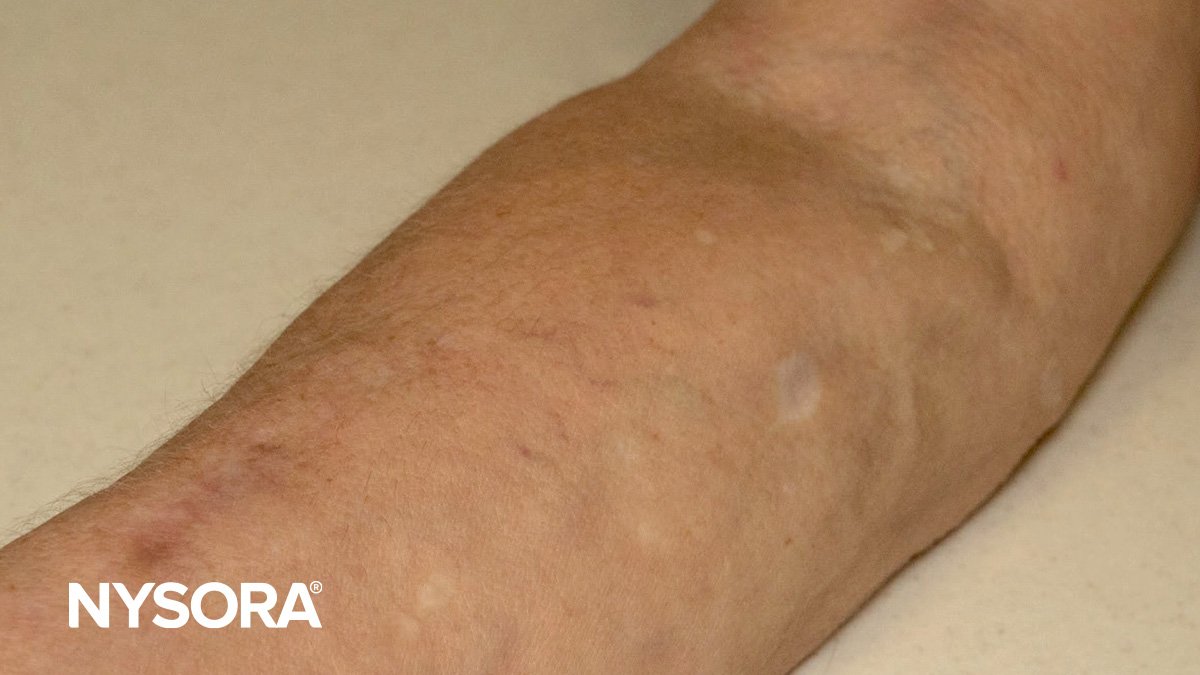
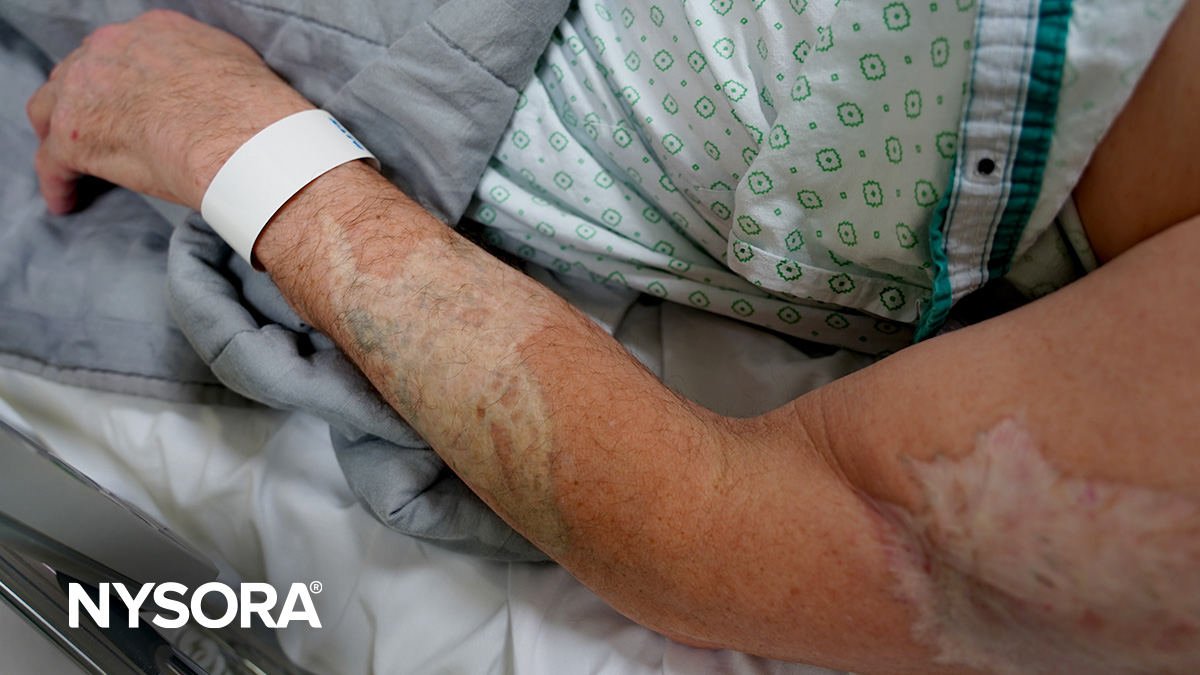
Damaged veins
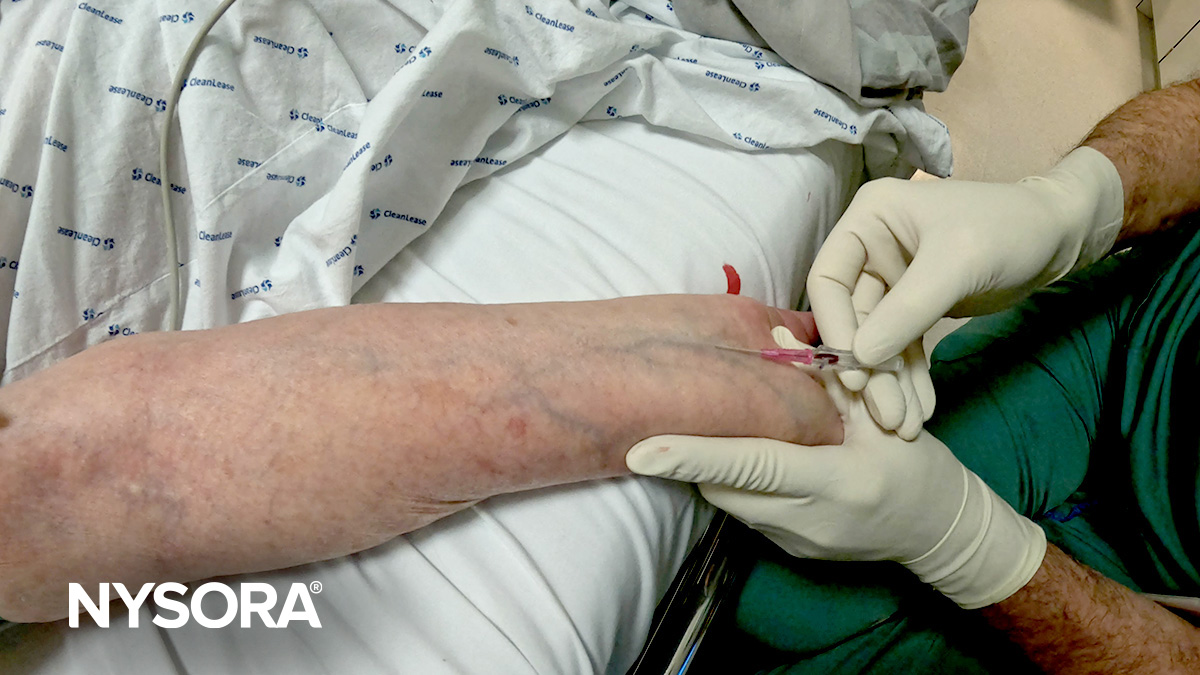
- Challenge: Frequent IV drug use can severely damage veins, leading to thrombophlebitis or scarred and collapsed veins, complicating traditional IV access.
- Solution: Use ultrasound guidance to identify viable veins in non-traditional areas, as common sites might be overused or damaged. Consider alternative access methods, such as CVCs or IO access.
Infection risk
- Challenge: Precaution: increased risk of bloodborne infections such as HIV or hepatitis.
- Solution: Use standard precautions and personal protective equipment to avert transmission. Regularly screen for and manage infectious complications.
Soft tissue infections
- Challenge: Non-sterile IV drug use can introduce pathogens, giving rise to cellulitis, abscesses, or more severe infections.
- Solution: Avoid placing IV lines near infected areas, treat infections promptly, and consider alternative sites for IV access.
Withdrawal symptoms
- Challenge: Patients with active drug dependency may undergo withdrawal symptoms, complicating their care.
- Solution: Remain vigilant and prepared to address withdrawal manifestations or facilitate referrals to specialized care providers.
Trust issues
- Challenge: Patients may be distrustful due to previous negative experiences with healthcare providers or the stigma associated with drug use.
- Solution: Approach these patients with empathy and patience, working to build trust. Engage in open communication, provide reassurance, and use short-acting anxiolytic medications if necessary.
Clinical updates
- Bahl et al. (Journal of Infusion Nursing, 2024) conducted a systematic review and Bayesian multivariate meta-analysis of 20 studies and identified five independent predictors of difficult intravascular access (DIVA): nonpalpable veins, nonvisible veins, history of DIVA, IV drug abuse, and obesity. Based on these findings, they introduced the SAFE rule (See, Ask, Feel, Evaluate BMI) to prospectively identify high-risk patients before the first cannulation attempt and recommend early escalation to ultrasound-guided or advanced access techniques. Notably, IV drug abuse emerged as an independent risk factor in pooled analysis, supporting formal pre-procedural screening and early ultrasound use in patients with a history of injection drug use to reduce multiple failed attempts and associated complications.
Reference: Bahl A et al. An Improved Definition and SAFE Rule for Predicting Difficult Intravascular Access (DIVA) in Hospitalized Adults. J Infus Nurs. 2024;47:96-107.
- Eastridge et al. (British Journal of Nursing, 2025) describe the development and pilot validation of the Substance Use Risk Assessment (SURA) tool to identify hospitalized patients at risk of vascular access device (VAD) tampering. Implemented in 566 screened patients, SURA stratifies misuse risk and links scores to targeted interventions such as urine drug screening, tamper-evident technology (TET), closer room placement, room searches, and formal care contracts. The tool demonstrated excellent content validity, and case examples showed early identification prevented potential VAD misuse and facilitated safer outpatient IV antibiotic therapy. These findings support structured risk screening and tamper-prevention strategies in patients with a history of injection drug use to reduce CLABSI, overdose risk, and against-medical-advice discharges.
Reference: Eastridge T et al. Substance use risk assessment: assessing the risk of vascular access device tampering in patients with a history of drug use. Br J Nurs. 2025;34:S18-S23.