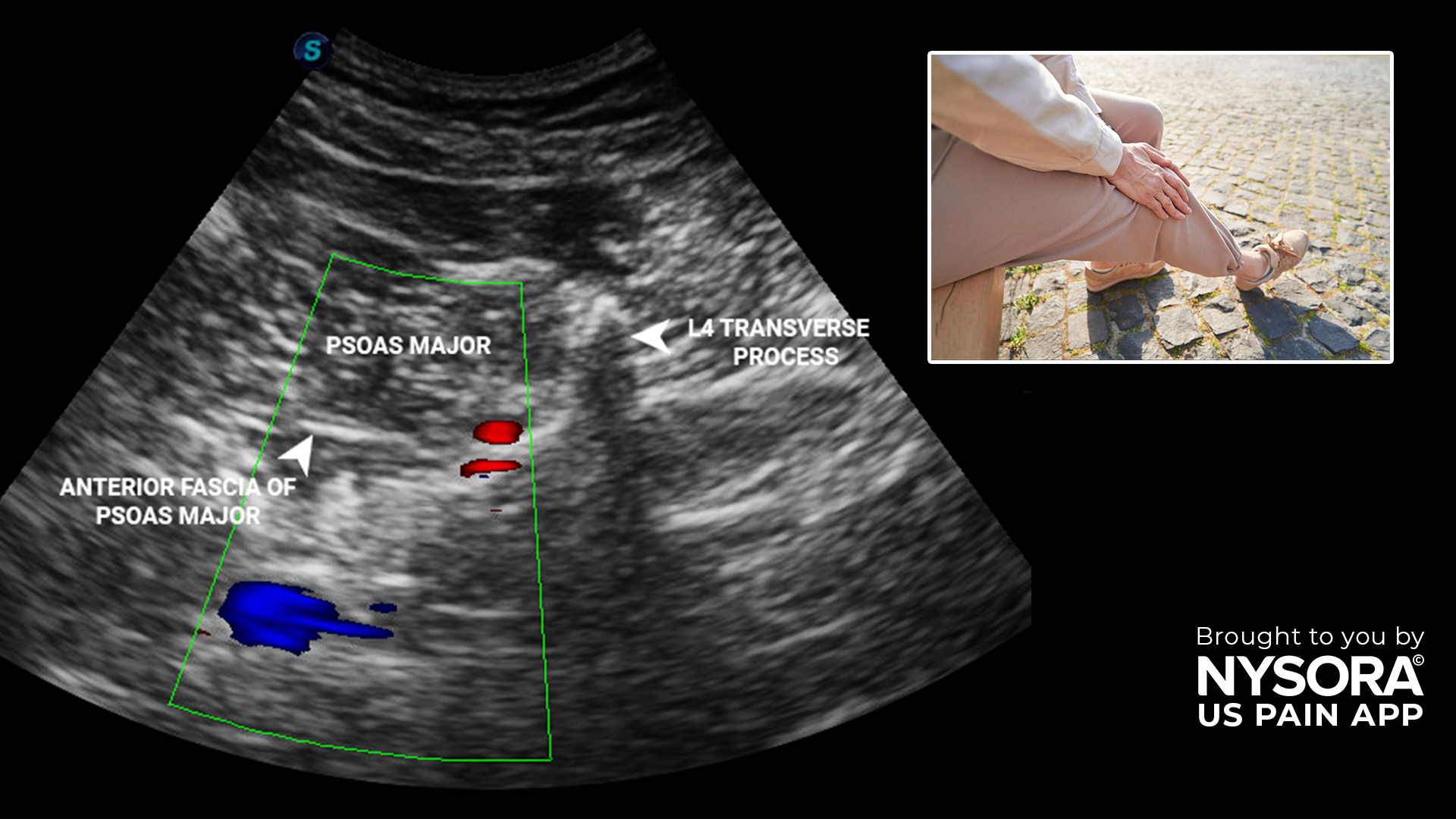
Case presentation
A 69-year-old patient, 156 cm tall, weighing 90 kg, with a long history of diabetes mellitus, presented with foot gangrene and was scheduled for wound debridement and potential amputation. The patient’s hemodynamic status was stable, and no signs of systemic infection were observed. Relevant medications included insulin and low-molecular-weight heparin, which had been discontinued 48 hours prior to the procedure. Airway assessment indicated Mallampati Class 2 (MP 2).
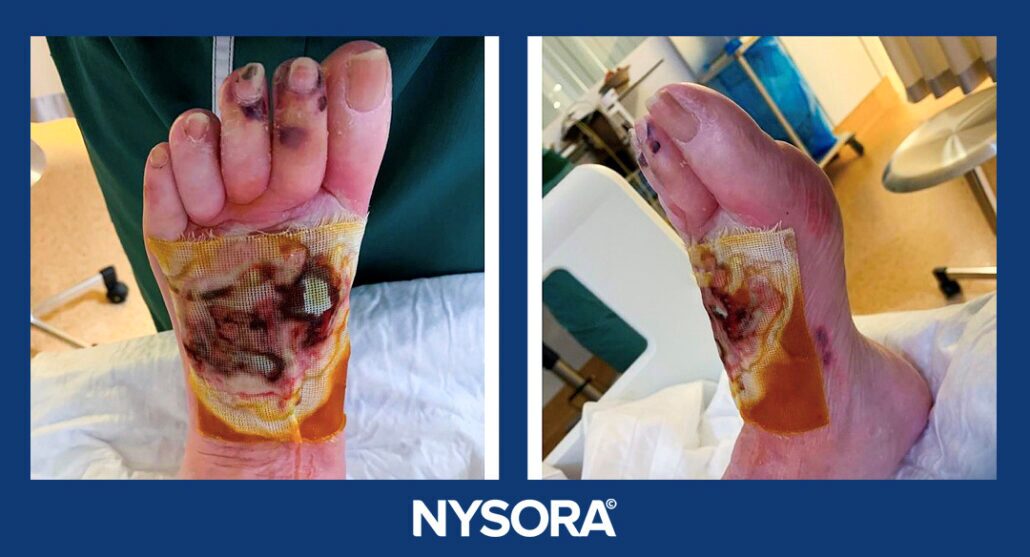
Anesthesia plan
The patient’s hemodynamic stability and absence of systemic infection allowed for the consideration of general anesthesia. However, postoperative pain management posed a challenge due to the potential need for opioids and associated risks. To mitigate these risks, the utilization of peripheral nerve blocks was explored as an alternative approach.
Specifically, a popliteal block with 20 mL ropivacaine 0.5% and a femoral triangle block for saphenous nerve territory coverage using 5 mL of ropivacaine 0.5% were performed, allowing for effective pain management and avoiding airway instrumentation, intubation, and mechanical ventilation.
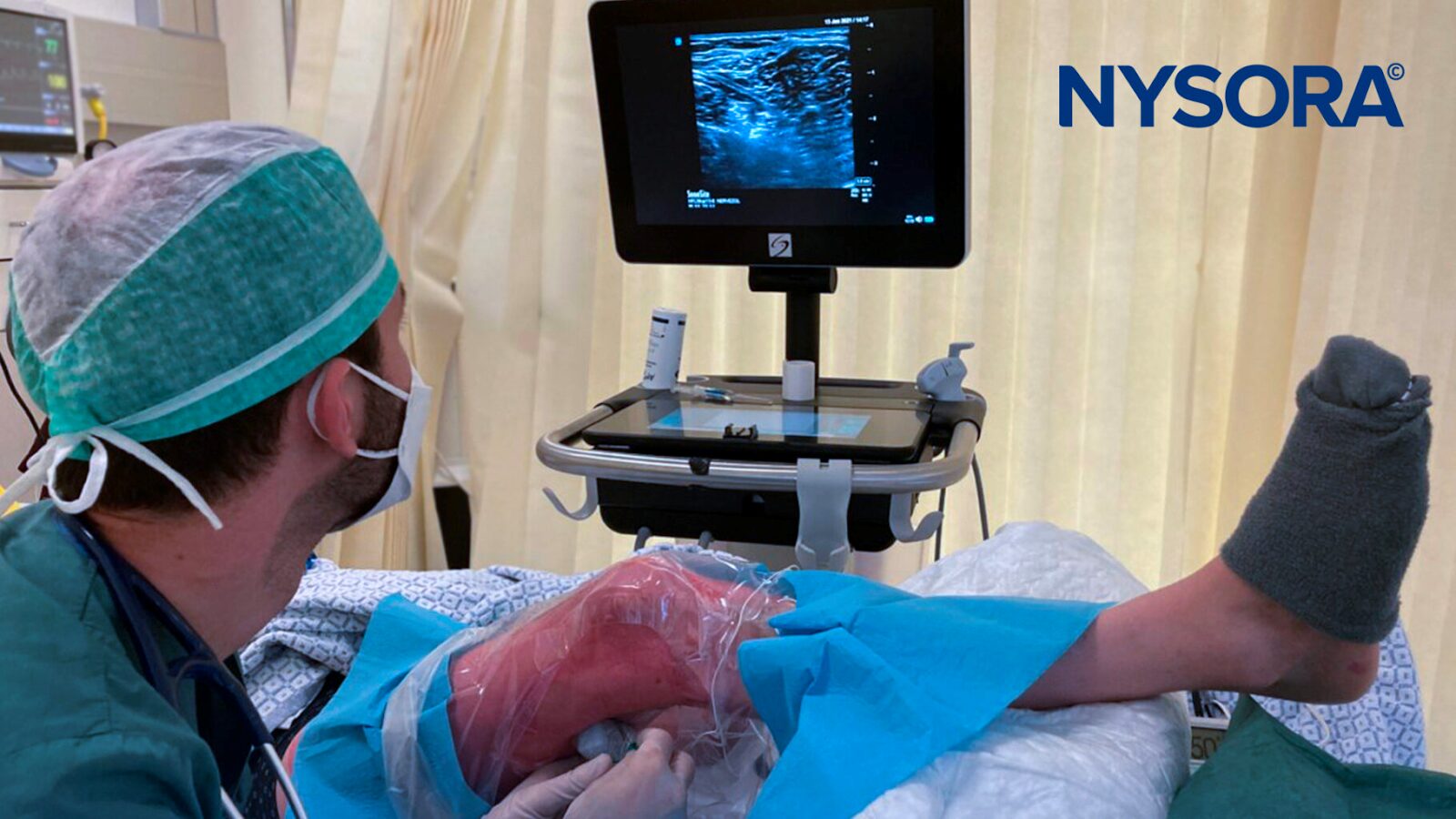
Patient outcome
The combination of the popliteal block and femoral triangle block resulted in complete pain management for 24+ hours. By utilizing nerve blocks, prolonged pain relief can be achieved, reducing the reliance on systemic opioids and lowering associated risks.
Ultrasound-guided popliteal sciatic nerve block: A game-changer in emergency lower limb surgery
In emergency medicine, rapid and effective anesthesia is critical, particularly when dealing with high-risk patients requiring urgent surgery. One promising technique is the ultrasound-guided popliteal sciatic nerve block, which is especially valuable for lower limb procedures. This method offers a safe and effective alternative to general anesthesia, minimizing the risks of cardiovascular instability, which is common in patients with severe comorbidities.
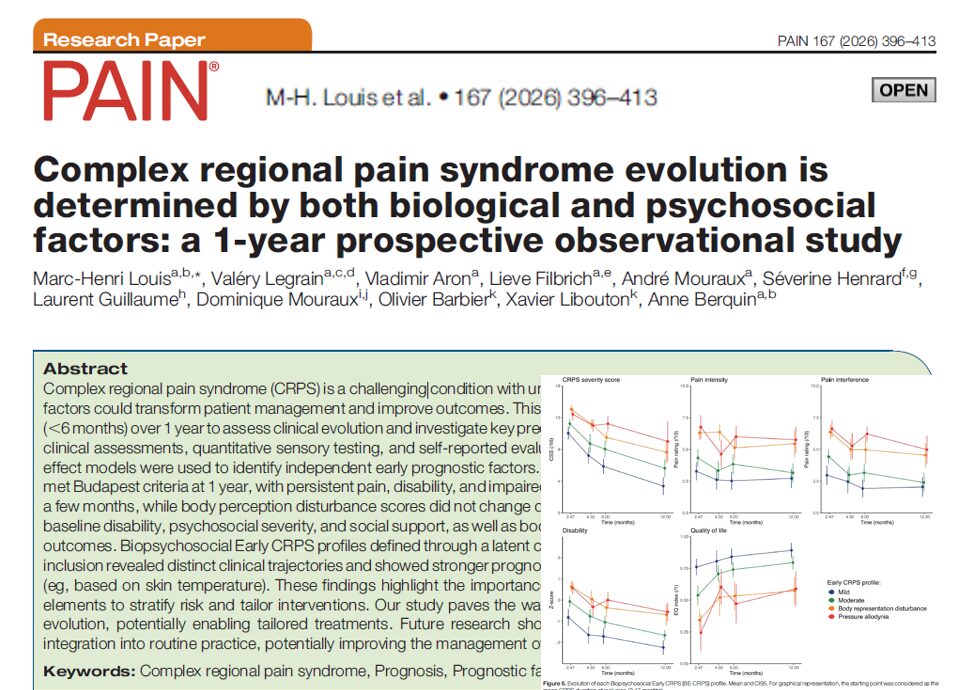
A recently published case report sheds light on the use of this anesthesia technique in a 70-year-old male patient with necrotizing fasciitis and septic encephalopathy. The patient was high-risk due to multiple comorbidities, including compromised cardiac and respiratory function, making general anesthesia dangerous. In such cases, regional blocks offer a lifesaving alternative.
What is a popliteal sciatic nerve block?
The sciatic nerve provides sensory and motor innervation to the lower leg, making it a prime target for regional anesthesia in lower limb surgeries. The block is performed by injecting local anesthetic around the sciatic nerve in the popliteal fossa at the back of the knee. This method temporarily blocks pain sensation and provides motor blockade in the lower leg, foot, and ankle.
Key advantages of popliteal sciatic nerve block
- Avoids the systemic complications of general anesthesia.
- Provides effective and long-lasting postoperative pain relief.
- Reduces the need for opioid medications.
- Minimizes the risk of respiratory or cardiovascular complications, crucial for high-risk patients.
The case presentation: Managing a high-risk patient
In this case, the patient presented with a necrotic ulcer on his left foot, sepsis, and signs of septic encephalopathy. Sepsis-associated encephalopathy (SAE) is a common but poorly understood complication, often leading to neurological dysfunction without direct central nervous system infection. The patient’s compromised state made general or central neuraxial anesthesia extremely risky due to potential profound hypotension, myocardial depression, and the need for mechanical ventilation postoperatively.
Preoperative concerns
- The patient was disoriented, delirious, and non-cooperative, complicating history-taking.
- Laboratory results indicated persistent hypoglycemia, moderate hyponatremia, and elevated creatinine, alongside a deranged coagulation profile.
- Cardiovascular evaluation revealed significant findings, including an ejection fraction of 25% and multiple valve defects, highlighting the high-risk status of this patient.
Given the patient’s condition, an ultrasound-guided popliteal sciatic nerve block and adductor canal block were chosen. These regional anesthesia techniques have become increasingly popular due to their ability to deliver precise and effective nerve blocks with minimal complications.
Step-by-step guide to popliteal sciatic nerve block
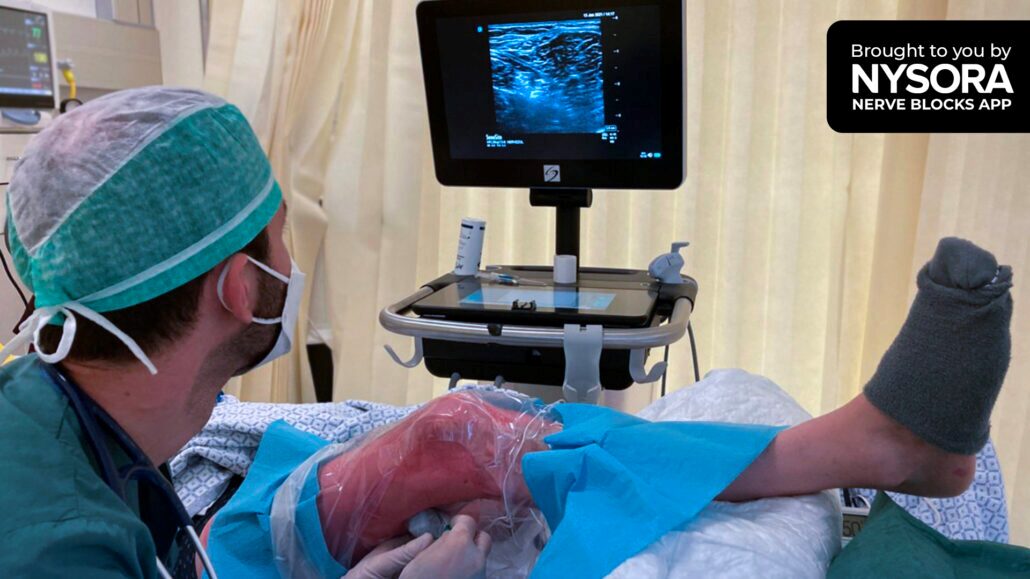
- Patient positioning: The patient was placed in a right lateral decubitus position to allow access to the left leg.
- Ultrasound setup: A high-frequency linear transducer probe visualized the sciatic nerve between the biceps femoris and semitendinosus muscles.
- Needle insertion: A 23-gauge spinal needle was inserted under ultrasound guidance to deliver 25 cc of 0.5% ropivacaine mixed with 8 mg of dexamethasone. The needle was advanced carefully to avoid vascular structures, and a doughnut-shaped spread of the anesthetic was visualized to confirm proper needle placement.
- Confirmation: The local anesthetic spread was confirmed at the injection site and 4-5 cm proximal, ensuring adequate coverage of the sciatic nerve. An additional adductor canal block was performed to cover the medial side of the thigh.
- Monitoring: The patient’s vital signs were closely monitored throughout the procedure, with fluid administration restricted due to the low ejection fraction.
Intraoperative and postoperative care
- The surgery—lower limb debridement and fasciotomy—was successful, with minimal intraoperative complications.
- Blood loss was controlled, and there was a notable release of compartment pressure after the procedure.
- The patient was transferred to the ICU for observation and postoperative care.
Postoperative outcomes
- The patient’s white blood cell count decreased from 17,400/µL to 11,000/µL.
- There was a significant reduction in pain at the surgical site, attributed to the effective nerve block.
Conclusion
In the case of this high-risk patient, ultrasound-guided popliteal sciatic and adductor canal nerve blocks provided an excellent anesthetic alternative. This approach minimized hemodynamic changes, avoided the complications of general anesthesia, and ensured a successful surgical outcome with minimal postoperative pain. As regional anesthesia techniques continue to evolve, they offer a vital tool in managing patients who would otherwise be considered too risky for surgery.
For more information, refer to the article in Cureus.
Soor B, Garg I. A Case Report of an Ultrasound-Guided Popliteal Sciatic Nerve Block: An Asset for Emergency Lower Limb Debridement in a High-Risk Patient. Cureus. 2024 Apr 7;16(4):e57752.
Explore additional case studies and access the comprehensive guide to the 60 most common nerve blocks by downloading the Nerve Blocks App HERE. Don’t pass up the opportunity to acquire the bestselling NYSORA Nerve Blocks App, now also available in book format – the ideal study companion to complement the app!