Epidural analgesia and anesthesia are commonly used for pain relief during labor, or to provide anesthesia or analgesia during surgery. Proper training and technical skills and essential for success and reducing the risk of complications[1]. Although extremely common in clinical practice (approximately 300,000 epidurals annually in the UK), teaching is often extremely difficult in busy environments[2]. Learning to perform an epidural block in patients entails a risk of procedural failure or post-dural puncture headache (PDPH) which can be disabling and may occur in up to 3% of the cases.[3]
The procedure entails inserting an epidural Tuohy needle into the lumbar spine through the skin, subcutaneous fat, supraspinous and interspinous ligaments, ligamentum flavum, and then to the epidural space. Epidural needle insertion utilizes a technique referred to as “Loss of Resistance” (LOR) to recognize proper needle placement in the epidural space.
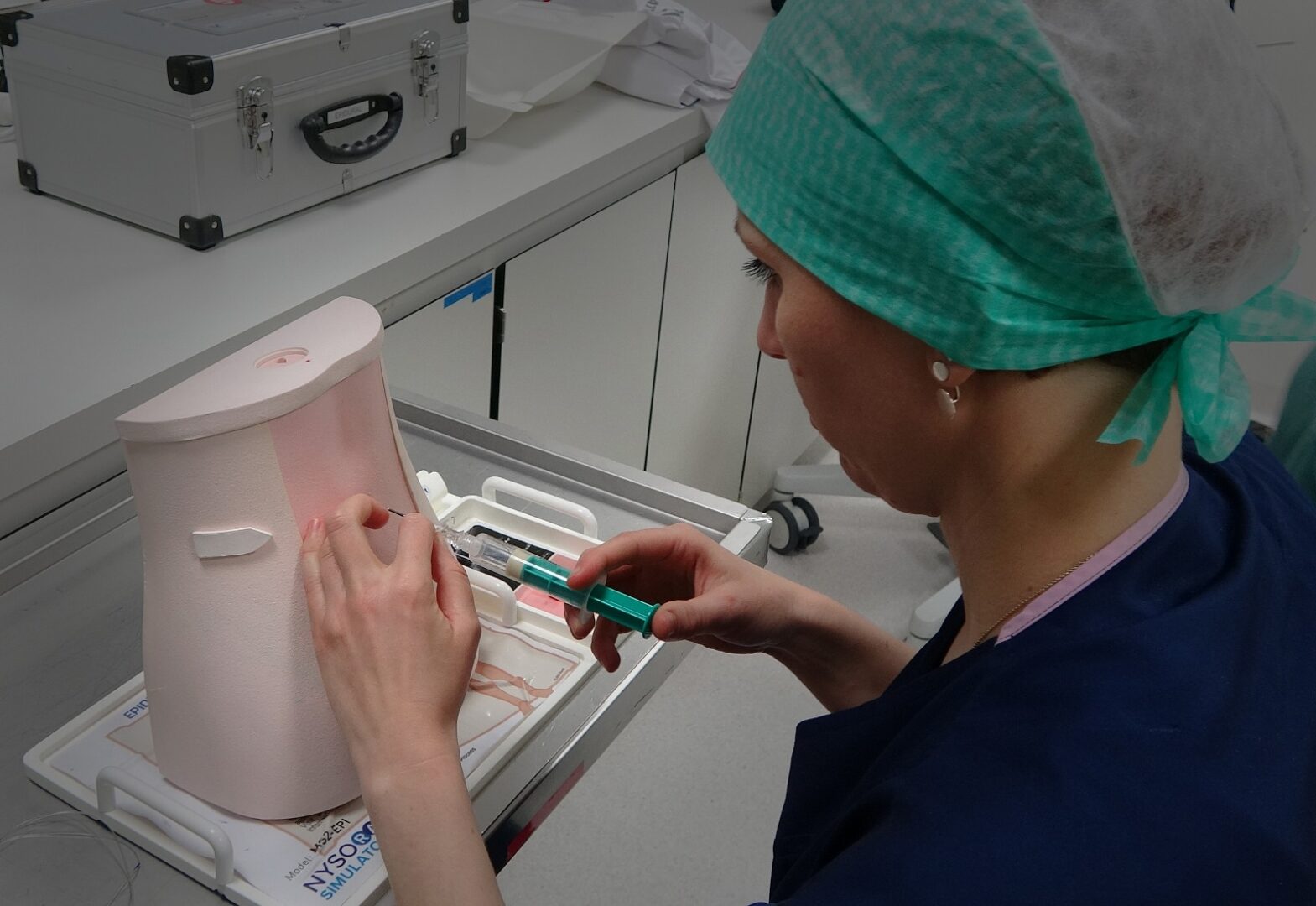
NYSORA Epidural Simulator facilitates the training of the entire procedure, including loss of resistance and catheter insertion, without placing patients at harm. Moreover, NYSORA simulators can also be used to teach or acquire ultrasound-guided regional anesthesia skills in the fastest time possible.
