Case study: Anesthetic approach for elbow surgery in an obese, COPD Gold III patient with prior MI
Case presentation
A 52-year-old obese woman with chronic obstructive pulmonary disease (COPD) Gold III and a history of acute myocardial infarction (AMI) was scheduled for elbow surgery. Due to her complex medical history, a tailored anesthetic strategy was necessary to mitigate potential risks.
For pulmonary reasons, local anesthetic spread toward the phrenic nerve should always be avoided. For cardiac reasons, an insufficient block and rescue general anesthesia should be avoided. Slow titration is best to ensure this.
An ultrasound-guided supraclavicular catheter placement was proposed. A supraclavicular block reduces the risk of phrenic nerve paralysis and the resulting diaphragmatic paresis compared to an interscalene block.
Nerve block technique
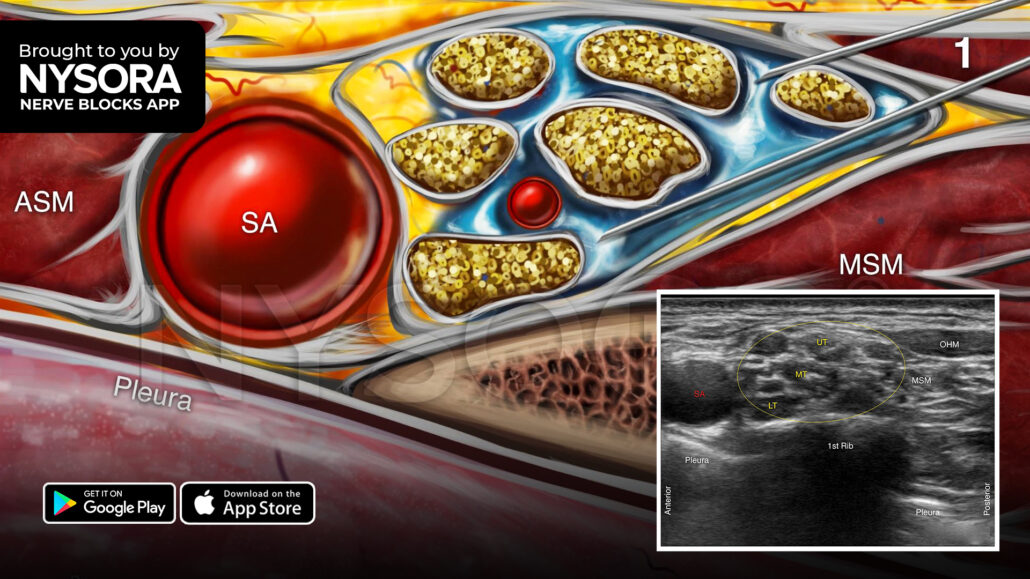
The goal is to place the catheter near the trunks and divisions of the brachial plexus adjacent to the subclavian artery. The procedure consisted of three phases: (1) needle placement, (2) catheter advancement, and (3) catheter securement. The needle was inserted in-plane, in a lateral-to-medial direction, ensuring the tip was just posterior to the brachial plexus sheath. Subsequently, the needle was advanced to pierce the sheath, followed by catheter placement. An initial dose of 10 mL of bupivacaine 0.5% was administered. After 25 minutes, the anesthesia of the arm was tested, and small increments of local anesthetic were administered if necessary.
Patient outcome
The patient recovered well without any significant complications related to the anesthesia.
The chosen anesthetic approach, considering the patient’s COPD Gold III and history of AMI, proved to be successful in providing safe and effective anesthesia for elbow surgery.
Explore additional case studies and access the comprehensive guide to the 60 most common nerve blocks by downloading the Nerve Blocks App HERE. Don’t miss the opportunity to acquire the bestselling NYSORA Nerve Blocks App, now also available in book format – the ideal study companion to complement the app!